It’s always a pleasure to hear from readers who report improved health.
Some of these emails are poignant: distressing because of the pain of their diseases, yet heartening because of the improvements a good diet brings.
It can’t get more poignant than to hear that children with a painful, deadly, and untreatable disease have, thanks to diet, begun smiling, laughing, and getting better.
Last week Kindy Flyvholm, who bought our pre-publication e-book, wrote with just such a report. I’m delighted to be able to pass it on, and hopeful that this report will help other children escape unnecessary suffering and enjoy life more abundantly. Thank you, Kindy, for sharing your story!
Ketogenic diets as therapy for neurological dysfunction
In our book and on this blog, we advise everyone with a neurological or brain disorder to try a ketogenic (“ketone generating”) diet. The book spells out how to tweak the Perfect Health Diet to make it ketogenic: basically, reduce carbs and add copious amounts of coconut oil.
Ketogenic diets can be surprisingly helpful with brain and nerve dysfunctions. The reason is that neurons have very limited metabolic options: they can burn only glucose or ketones. Glucose metabolism is complex and prone to failure; ketone metabolism is simple and robust. Especially in disease states, a neuron on glucose can be a totally different creature from a neuron on ketones. Neurological diseases that are disastrous on a glucose-rich diet can become mild when neurons are fed ketones.
It doesn’t work for every brain disease, in part because ketones don’t diffuse through the brain all that well. Ketones reach the subcortical and inner cortical layers of the brain easily, but don’t readily reach superficial layers. [1] However, in some diseases the places reached by ketones are the ones in trouble. The evolutionarily oldest parts of the brain, such as the brain stem, are the most likely to benefit from a ketogenic diet. Thus, neurodegenerative diseases that cripple the body may be top candidates for a therapeutic ketogenic diet.
NBIA (Neurodegeneration with Brain Iron Accumulation)
One such disease is NBIA, short for Neurodegeneration with Brain Iron Accumulation. NBIA is most commonly caused by a mutation in the gene PANK2, which codes for the mitochondrial enzyme that converts vitamin B5 (pantothenic acid) into CoenzymeA (a crucial metabolic substrate). This version of NBIA is called PKAN, for pantothenate kinase-associated neurodegeneration.
NBIA/PKAN is characterized by an accumulation of iron in the basal ganglia of the brain. The iron is readily visible in brain MRIs, producing an “eye of the tiger” brightness pattern. [2] It produces symptoms that overlap with those of Parkinson’s disease. [3] About 1 in 500 people carries a PANK2 mutation, so some form of the disease strikes 1 in 250,000 people.
The disease typically first presents itself about age 3, when leg dystonia and spasticity causes an impaired gait, sometimes including toe-walking. The disease progresses and children lose the ability to walk. Dystonia extends to the hands and the face; the head cannot be held upright, and swallowing becomes difficult. Blindness from retinopathy and hearing loss often develop. Premature death occurs usually in the teens, often by age 10 or younger. The last years are excruciatingly painful.
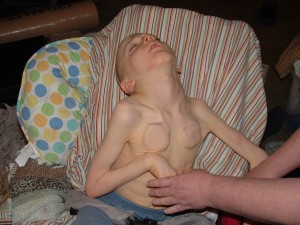
Here is a picture of Zach, age 12:
You can see his inability to hold his head upright, and the hand position characteristic of dystonia. Zach cannot swallow naturally and has to be tube-fed.
The bumps in his chest are from the battery packs used to drive a deep brain stimulation device. The idea is to introduce signals that counter the excruciatingly painful dystonic spasms. Like other therapies for NBIA, deep brain stimulation is often ineffective. In Zach’s case, the device worked for less than one month. It is now turned off but is not removed because the operation would be too traumatic.
Ketogenic Diet Therapy
Kindy writes:
It was in desperation that we began researching options (ANY OPTION) to prevent the horrible pain that precedes death especially in the case of children with early-onset NBIA.
Many research paths led to the ketogenic diet being an option. A lot of discouraging information was presented as well (like how impossible it is to follow or how disruptive it is to family life, etc).
It’s remarkable, but doctors are so divorced from dietary science that they do not know how simple and natural a ketogenic diet can be, and assume that only absurdly onerous formulations are needed. As we point out in the book, a large fraction of mammals eat ketogenic diets as their natural diet; and all mammals including humans subsist on ketones during starvation.
Doctors were pessimistic about its chances, but a ketogenic diet produced amazing results:
My son, who is 6, … has been on the diet for less than one month and his hands have relaxed enough for him to regain his pointing ability (which had been lost).
Zach, the 12 year old on the diet, is much further progressed in the disease. Zach has been on the diet since late October, 2010, reaching 80% fat levels towards mid-December. The following are the improvements that have been noted by Zach’s family and therapists: Zach has begun holding up his head even though his neck has been hyper extended backwards since he was 9, he has begun pointing with his finger again instead of the palm of his hand, he is moving his right arm again some, and the latest thing is that he is now able to go from a laying position to a sitting position on his own by hanging on to something or someone. He has not done this since he was 9 years old.
Both boys have begun smiling and laughing all the time.
I know just how they feel!
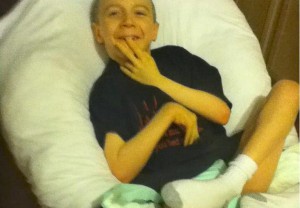
The previous picture was Zach before starting the ketogenic diet. Here he is on the diet:
Kindy continues:
Zach has gotten off all pain medicine and only has a small amount of 3 [anti-spasmodic] medicines left which hopefully he can get off of over the next year.
Going in and out of ketosis has immediate effects, as this anecdote shows:
Zach had a recent day where his muscle spasms returned severely. Bad enough he needed to go to the hospital for morphine. At the last minute (before going to the hospital), the parent looked at her recipe for that day and realized she had used a lot of white chicken meat. She added in some more coconut oil into his next few tube feedings and the spasms went away immediately. This is extremely powerful.
Kindy concludes:
We are not under any delusions. Our children may be taken from us at any time. If they are taken pain free, then we are blessed compared to the alternative. The situation thus far with our ‘experiment’ has proven much more than we could have hoped.
Conclusion
Kindy, it’s wonderful that your research and perseverance has bought hope to your son, and that you’re spreading the word to help others find the same hope. I’m so grateful that you’ve shared your story with us. Hopefully your experiences will reach the NBIA community, save children from unnecessary pain, and maybe extend their lives significantly!
We salute every parent who has to deal with neurological and genetic diseases in their children. As this disease illustrates, anyone with a neurological disorder should experiment with a ketogenic diet. Ketogenic diets have been tested in very few diseases, and there is no telling how many neurological diseases may prove amenable to this therapy. But there is already considerable evidence that neurological diseases of the elderly, such as Alzheimer’s and Parkinson’s, are treatable with a ketogenic diet.
Last Thursday, I defended the idea of a healthy diet as the best therapy for disease (“Therapy AND Life”). The NBIA kids illustrate just how powerful dietary therapies can be.
Medical doctors seem to have great misapprehensions and fear of experimenting with this diet. They do not understand it, don’t know how it should be implemented, and have never tried it themselves. Many of the medical ketogenic diets are malnourishing and generate terrible side effects. Not surprisingly, many patients quit the diets.
This coming Thursday, I’ll discuss how to implement a safe, healthy, and pleasurable-to-eat ketogenic diet. There’s no reason for an unpalatable or malnourishing diet to stop patients from enjoying the benefits that Zach has seen!
References
[1] Hawkins RA, Biebuyck JF. Ketone bodies are selectively used by individual brain regions. Science. 1979 Jul 20;205(4403):325-7. http://pmid.us/451608.
[2] Gregory AM, Hayflick SJ. Neurodegeneration with brain Iron Accumulation. Orphanet Encyclopedia, September 2004. http://www.orpha.net/data/patho/GB/uk-NBIA.pdf.
[3] Klein C et al. Hereditary parkinsonism: Parkinson disease look-alikes–an algorithm for clinicians to “PARK” genes and beyond. Mov Disord. 2009 Oct 30;24(14):2042-58. http://pmid.us/19735092. Paisán-Ruiz C et al. Early-onset L-dopa-responsive parkinsonism with pyramidal signs due to ATP13A2, PLA2G6, FBXO7 and spatacsin mutations. Mov Disord. 2010 Sep 15;25(12):1791-800. http://pmid.us/20669327.











Recent Comments