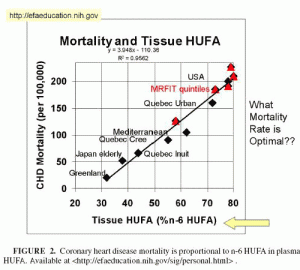
The importance of achieving a good omega-3 to omega-6 ratio has been demonstrated repeatedly in clinical trials and epidemiological studies. Cardiovascular disease mortality is especially strongly dependent on this ratio [1]:
This plot shows coronary heart disease mortality plotted against the fraction of long polyunsaturated fats in tissue that are omega-6, not omega-3. It’s best to have around 30% omega-6, 70% omega-3. But most Americans have around 78% omega-6, 22% omega-3. Their omega-6 to omega-3 ratio is 9 times the optimum, and CHD mortality is ten-fold higher than is necessary.
Dr. Bill Lands, one of the pioneers in omega-3 and omega-6 science, notes that the tissue ratio is determined by how much of each type of fat is eaten:
There seems to be no ‘corrective’ metabolic response to prevent fatal tissue combinations from being developed. As much as humans might wish for some protective re-adjustment of the metabolic promiscuity, the enzymes seem to continue assembling harmful and harmless combinations in response to supplies ingested – without much regard to or feedback from the consequences. [2]
So it’s important to eat these fats in the right ratio.
How do you do that? These steps:
- Minimize omega-6 fats by:
- Avoiding most vegetable oils, including soybean oil, corn oil, safflower oil, and canola oil.
- Using low-omega-6 oils, such as coconut oil, butter, beef tallow, olive oil, and lard, in cooking and dressings and sauces.
- Regularly eating low-omega-6 red meats, like beef and lamb.
- Get sufficient omega-3 fats by eating 1 lb per week of fatty cold-water fish, like salmon or sardines.
These simple dietary changes can reduce your risk of dying from a heart attack by a factor of ten.
Yet how many doctors recommend these steps? Indeed, many recommend the opposite: avoiding saturated fats in coconut oil, butter, and beef tallow; avoiding red meats; and eating lots of vegetable oil.
This is a great example of our First Law of Health: Every conventional dietary recommendation is wrong.
[1] Lands WE. Dietary fat and health: the evidence and the politics of prevention: careful use of dietary fats can improve life and prevent disease. Ann N Y Acad Sci. 2005 Dec;1055:179-92. http://pmid.us/16387724. Lands WE, http://efaeducation.nih.gov/sig/personal.html. Hat tip Stephan Guyenet, http://wholehealthsource.blogspot.com/2008/09/omega-fats-and-cardiovascular-disease.html.
[2] Lands WE, http://efaeducation.nih.gov/sig/composition%20maintained.pdf.











Dear Paul, greetings from Germany – email is a wonderful thing. Thank’s for offering all the great information in your blog.
While waiting for your book to be shipped, i would like to ask for your opinion on omega-3 in flaxseed oil, grounded flaxseed and its combination with low-fat or 20% fat cottage cheese with one added apple and a handful of mixed nuts and seeds.
This combination has a tradition in Bavaria where in old times the access to salmon, sardines etc. was difficult and I think there is some truth to sticking as much as possible to the regional foods one is genetically accustomed.
However in light of all the discussion about PUFAS i am not sure about the health benefits of pure flaxseed oil, grounded flax seeds (also in respect to its estrogenic character)and its combination with dairy.
In addition the above noted food combination of flaxseed oil and dairy seems to have some form of addictive character as i have tried many times to switch to a different breakfast but always come back to this.
Thank you very much for advising.
best regards
Irmgard
Dear Irmgard,
We don’t have a recommendation re flaxseed oil either pro or con. It should be healthy in moderation, but we think salmon or other cold-water marine fish are the best source of omega-3s.
It is normally fine to combine it with dairy … however:
Addictiveness may indicate the presence of food opiates. Partially digested dairy can have opioid activity. Chocolate also contains opioids, you could test to see if dark chocolate feels addictive too.
So you might want to watch out for dairy sensitivity.
Are there any good omega-6 fats?
Having reduced/dropped all my Poly fat intake, given up all oils except mct, coconut & macadamia (i don’t like olive oil or olives) & even stopped avocadoes. (i do eat fatty fish….mostly wild salmon).
I’m just wondering if i need to make sure i intake some omega-6’s, i read GLA is one of the good guys?
So i’m thinking of reintroducing avocado oil, but i don’t believe that it contains GLA. All GLA sources look to be seed sources; the only one that sounds like it may be a ‘PHD acceptable’ source is blackcurrant seed oil?
…..what do you think, your comments appreciated.
Hi Darrin,
All omega-6 fats are good in low doses, bad in high.
Some people argue for GLA supplementation because it modulates omega-6 and omega-3 conversion pathways in a way that may improve the ratio of key fatty acids. However, I think this is over-optimization and likely to backfire. I would just eat natural foods, get omega-6 and omega-3 in the proportions they are found in real foods, and let my body control which fatty acids are converted into which.
Avocado oil is a healthy oil, similar to olive oil.
I don’t object to blackcurrant seed oil in small doses, as it’s less than 30% PUFA.
Thanks Paul. I am currently fine tuning my calorie ratios based on how i feel, sleep, skin & hair quality.
I recently had some saliva tests done which indicated i had very high cortisol levels throughout the whole day, which explains my bad sleep. All other results were good; dhea, testosterone, oestradiol.
Looking back on it i was quite low carb when the tests were done (sub 50g per day) & i was not reaching the PHD min 600cals with protein.
So i think part of the reason for my high cortisol was that i was under-eating & this was putting stress on my body.
Other current symptoms (apart from the insomnia) are dry skin & increased hair loss.
So to address the cortisol issue i have now upped my ratios to 20:60:20 (i function better with a bit more protein). Before i found PHD i was following the ‘metabolic typing diet’ which flags me as a very strong ‘protein type’.
My sleep really hasn’t improved yet, but it’s only been 3 days since i corrected my ratios.
The whole cortisol sleep thing seems to be a bad feedback loop; bad sleep = higher cortisol, higher cortisol = bad sleep.
The other thing i was considering trying is melatonin supplements before bed; can you give me an idea of a protocol to use please; type/dosage/duration. would they be a long term thing, or just till my cortisol cycle was fixed.
The other supp mentioned by my naturopath was GABA, but i was reading that GABA & melatonin affect completely different pathways & they each address/help different sleep issues & melatonin is the correct one that relates to cortisol issues. (& the wrong one can make matters worse).
Thx again, Darrin
Hi Darrin,
Dry skin, hair loss, and sleep disorders are all symptoms of hypothyroidism. Do you know your TSH level? If not I would get to a doctor and get that measured.
I’d also start our supplements for hypothyroidism if you haven’t already. Copper, magnesium, selenium, iodine. Build up iodine slowly.
For melatonin, you have to adjust the dose to your own needs; too much and you’ll go to sleep quickly but wake up early.
I would try a 5 mg time-release (Natrol has this) just before bed, possibly with a 1 mg immediate-release (Source Naturals is a good brand).
I wouldn’t take GABA. Ketosis is a better way to increase brain GABA levels (http://www.ncbi.nlm.nih.gov/pubmed/19285044). The best thing for that is intermittent fasting, 16 hours per day, taking coconut oil or MCTs at the end of the fast. So you still get adequate starch and protein in your feeding period.
The 20/60/20 macronutrient ratio is good.
I expect you probably wouldn’t need melatonin once your starch intake increased and your hypothyroidism is fixed; however, chronic infections cause low melatonin, high cortisol, and iodine-deficiency hypothyroidism, so we can’t rule out that possibility yet. Address the diet and hypothyroidism first, and see what symptoms are left.
Best, Paul
Hi Paul,
My TSH level back in April 2009 was:
TSH 1.7 mIU/L (Australian numbers. range 0.5-4.5).
(Age at time 43, male).
Average Diet ratio at the time C:F:P was 28:43:29.
I had already cleaned up my diet, but it was before i went paleo….which then let me to PHD.
The copper, magnesium, selenium i have been on for quite some time now. The iodine is a new addition, started on 1st Mar 2011 @ 190mcg per day (using iodide drops), now doing about 435mcg per day.
Another supp i take that may be worth a mention, B5 at 500mg per day.
My symptoms (sleep, hair, skin) did worsen when i was on very low starch (& sometimes low protein in hindsight). This VLC diet lasted 2.5 months (13th Jan 2011 till 31st Mar 2011) till i found PHD & got my PHD ratios adjusted correctly.
I believe you are correct, that i do have thyroid issues, tho i believe my number one issue at the moment is adrenal (chronic high cortisol), from what i read the two are closely linked & i need to get my adrenals functioning normally which will also help my thyroid (reading sources http://www.stopthethyroidmadness.com/adrenal-info/ & http://www.drrind.com/).
On the melatonin subject, would the homeopathic stuff work, could it be worth giving it a go first? i can easily get that here, but for the stronger “real stuff” i need to see a Doctor & probably do some fast talking to convince the Doc (here in Australia).
When you mention ‘chronic infections cause low melatonin, high cortisol, and iodine-deficiency hypothyroidism’, i take it there is no easy way to tell if this is the case for me & would the same diet & supp recommendations fix it?
thx, Darrin
Hi Darrin,
1.7 isn’t so bad. Did the symptoms develop after that?
Since you’ve only been off VLC for a few days, and VLC raises cortisol and may have aggravated your adrenal and thyroid issues, I think diet and nutrition may make a big difference in coming weeks.
You’re right about adrenals and thyroid, thanks for the links.
I haven’t investigated homeopathic medicines for sleep but I would be cautious.
Chronic infections can produce a wide array of symptoms. In the case of brain infections, the symptoms usually encompass those of serotonin deficiency and hypoglycemia (cognitive symptoms only). If you Google those you’ll find some long lists.
Yes, the same diet and supplement recommendations would hold for dealing with chronic infections. So I would start with diet and nutrition, and see where you stand after a few months. Use your doctors for monitoring thyroid/adrenal hormone levels.
If you do have to pitch melatonin to your doctor, you might use the diagnostic angle. If melatonin relieves your sleep issues, that tells you something about its cause. Then when you know it works, it’s harder for him to say no to more.
Best, Paul
Thanks Paul,
For now i will use my sleep is an indicator, if it does not improve i will go & see the Doc about melatonin.
to answer “1.7 isn’t so bad. Did the symptoms develop after that?”
yes & no…..the hair loss increase & dry skin are more recent symptoms, which i believe are linked to diet (poor diet).
With the sleep, i think i have had a problem with sleep all my adult life. i have always been a light sleeper & tended to wake at the top of each sleep cycle (approx every 90 mins). from memory my sleep improved somewhat when i went high protein.
Right now it’s more of a biphasic sleep pattern, but i think my biphasal sleep is not the ‘natural’ one that has been discussed recently here & on other sites, because i am definitely not refreshed in the morning.
My research into my sleep history first led me to the area of thyroid & then on to the adrenals, i think (hope) that if i can get my cortisol cycle corrected everything else will follow.
Ps. My blood sugar levels are okay, i have my own meter & tested this extensively, i do not suffer from hypo or hyper.
Pps. Other symptoms/tests that have led to the adrenals are, low & erratic body temp, possible low blood pressure/postural hypotension & low morning heartbeat 50 to 60bps sometimes sub 50 (or is this normal in a fit male 45yrs with about 13% bodyfat).
i wonder if Zinc is playing a part in some of my issues?
i saw somewhere else you mentioned going easy on the zinc (my words), something along the lines of supping with 1 or 2 50mg of zinc per week.
this got me thinking, i have been supping with zinc for a while (before phd), & it seems to be ‘hidden’ in quite a few of the formulas i have. so i added up all my supp sources of zinc.
Results: Zinc 242mg per week (av 34.6mg per day).
plus i eat a lot of oysters.
other related supps:
Copper: 15.3mg per week (av 2.2mg per day).
Magnesium: av 400mg per day.
So, for now i have dropped zinc back to 7.5mg per day, which is included in my ‘Thyro Guard’ formula.
But, this will also mean that my Copper supp will drop to 1mg per day. Should i up to 2mg? i don’t eat beef liver (i do eat chicken & duck liver in the form of pate & liverwurst).
Hmmm …
On an average diet I think 35 mg/day of zinc supplements should be OK if you’re taking 2.2 mg/day copper. However, the oysters could add a fair amount of zinc, and also it might be better to alternate high and low periods of zinc. That’s why I suggested 50 mg tablets several times a week, then you get high zinc 2 days and low zinc 5 days a week, probably enabling better copper absorption.
As a target I would aim for total zinc including food around 40 mg/day and total copper around 3 mg/day.
From food most people get 15 mg zinc and 1 mg copper. Oysters have about 90 mg zinc and 4.5 mg copper per hundred grams, so they could be adding significantly to both. Chicken and duck liver have minimal copper.
Offhand, I doubt that zinc and copper are causing your problems. The only likely issue at these levels might be providing over-abundant metals to gut bacteria.
Hi Again,
I just had some more blood tests done, including TSH.
With regards to supplementation, is it possible to initially see a (temporary) rise in TSH, before it starts to drop?
I am not saying this is what has happened to me of course. As i did not know my TSH level just prior to supplementation.
My TSH is now 2.3 (was 1.7 in April 2009).
Of course the Doctor says this is normal & fine (lab range is 0.5 to 4.5) & TSH levels will naturally vary (up & down).
How often should i get my TSH levels checked, every 3 or 4 months?
Hi Darrin,
I’d say it’s not uncommon. Most of the thyroid’s adaptation to supplements will be complete in 3-4 weeks but full adaptation can take months.
I think TSH should be checked in routine annual physicals for most people and anytime there are hypothyroid symptoms or if you’re concerned about effects of supplementation. It’s not bad to monitor it more frequently.
It’s possible to have hypothyroid symptoms with a TSH of 2.3; certainly your well-being is likely to be higher with a better TSH.
If you have hypothyroid symptoms, I would get a full panel.
thanks, i do have some hypothyroid symptoms at the moment (as mentioned above).
I’ll wait for a while to give the diet & supps some time to ‘kick in’. & I only just corrected (increased) my copper intake a few days ago.
When you get a moment, could you just recommend (list) which Thyroid related blood tests to get done. I know there are a few, & i am unsure which ones i should discuss with (convince) my Doctor to request.
Hi Paul,
Very good to see the web site back up & running.
Could you repost your reply to my last post, i’m hoping you still have it saved somewhere, it was very detailed.
I did see your response on the feed on my phone, but i was unable to copy, save or forward it to myself. & when i went to manually (old school) jot down your answer it had alreadly scrolled away in to the ether.
Hi Darrin, here it was:
Well, a fairly complete list would be:
-T3, T4, and reverse T3;
-antibodies: anti-TPO (thyroid peroxidase), anti-Tg (thyroglobuline)
– adrenal panel, esp cortisol
– serum ferritin, since iron deficiency causes hypothyroidism directly, while high iron can promote infections that can cause hypothyroidism
How many of these tests to get is up to you and your doctor … most doctors will resist all the tests since your TSH is in the “normal” range. In terms of which would be most actionable, might be cortisol and ferritin. For the full thyroid panel you might want to wait until you see what the effect of supplements is.
If you hypothyroidism was due to copper deficiency you may notice some hyperthyroid symptoms upon copper supplementation.
Best, Paul
Hi Paul,
Do you know anything about Doxylamine succinate?
I have seen it advertised as a Night-time sleep-aid (one 25mg tablet 30 mins before bed).
I have also seen it advertised as “Doxycycline without a prescription”.
I was wondering whether to give this a go.
At this stage the melatonin does not seem to work for me, but i am still experimenting with dosing; i started very low.
The other thing i have just discovered that may be a factor with my cortisol &/or insomnia (& may be even hair & skin)is MSM. I have been supplementing a half tablespoon MSM a day (about 6 grams) for a while now (5 ½ months) after reading so many good things about the stuff.
But after doing a lot more digging over last few days, I wonder if i am one of the (supposedly) few people that has a problem with sulfur (or MSM) & it is the MSM that may be chronically elevating my cortisol, which is subsequently causing all my other issues (insomnia, hair, skin). Anyway i stopped the MSM today, so i’ll see how things go from now. I may go back to a much lower dose of MSM (1g per day) in a couple of days.
Hi Darrin,
I’m afraid I don’t know anything about Doxylamine succinate.
I would recommend sulfur-containing foods like onion and garlic and N-acetylcysteine as a supplement, but avoiding MSM – especially in such high doses. Not that I know of any reason to fear MSM, but I don’t know of any benefits either, and food is the more natural way to get sulfur.
Best, Paul
I stopped taking MSM altogether as I think it effected my TSH.
Have your Free T3 checked as well-TSH tells us very little.
Check out http://www.stopthethyroidmadness.com
I went grain free a few months ago, and started on the PHD diet only a couple of weeks ago. I became very fond of flax crackers which are very simply whole flax seeds soaked in water overnight to generate maximum “flax slime” mixed with a bit of grated carrot and other seeds and spices/flavorings as desired. The soupy mixture is then dehydrated in a food dehydrator or an oven set to low with the fan on and door cracked open. I have read a lot back and forth about the value of flax as a source of omega-3 so I don’t count on it as a source of omaga-3 in my diet (I use salmon and makadrel for that). However, does eating whole flax seeds contribute to PUFA to my diet? If so I guess I will have to restart the search for a grain free cracker/flatbread alternative. :/
Hi Erika,
Flax seeds are fine and flax crackers are OK. Do you make them yourself or buy them? I’d like to give them a try.
Paul, do you have any information about how long it takes to reduce tissue HUFA percentage after curtailing dietary intake per PHD recommendations? I recall a comment in your book about results of one study being muddied by a crossover design. Do you have any thoughts about ways one might accelerate elimination of tissue HUFA? Intermittent fasting?
Thank you.
Hi Capri,
HUFA levels in cell membranes should adjust on the order of months, but it will vary by cell type. Blood cells, in maybe 2 months. PUFA levels in adipose tissue take longer, typically 4 years in clinical trials. PHD probably accelerates that by minimizing omega-6 intake and total calorie intake and improving mitochondrial health, but there is no data yet. Possibly supplementation of tocotrienols might help by enabling greater mitochondrial oxidation of omega-6 fats, but this is untested to my knowledge.
If manually setting the daily nutritional targets on a nutrition tracker, what would the percentages be for Omega-3 and Omega-6?
(I use Cron-o-metter. It keeps track of how many grams of each micronutrient it thinks are in your food and what percentage of your day’s calories each one comes to. At the automatic setting, it gives 1.1g as the minimum for Omega 3s and 12g for Omega 6s. That seems wrong?)
Hi Paul
I have read your book and understand you recommend eating mostly ruminants meat, 1lb fatty fish per week, and poultry just two times for variety. what would that mean in the case on my eating habits, which are: breakfast with eggs always, then I have a meal for Lunch and an early dinner, does that mean I could eat lunch and dinner with ruminants meat for most of the days of the week? consider I eat 8oz serving per each meal, I’m very active and need the protein, in place of red meat I also eat liver and heart once per week.
consider 7 days, I could do for lunch red meat everyday, with two days switching it with Organs, then two days dinner with fish, two days dinner with chicken, and 3 dinner with meat again? making 4 days of the week eating read meat lunch and dinner?
thank you
I meant “making 4 days of the week eating read meat lunch and dinner”
What about expeller-pressed canola oil?
I see you never got a reply to your question about experrer-pressed canola oil. Paul is involved in many endeavors and I don’t think he monitors this site frequently. What I can say is that canola oil, regardless of how it is processed is a toxic seed oil and it is best to be avoided. Hope you’re doing well.