A healthy gut is a multi-species society: it is the cooperative product of the human body with trillions of bacterial cells from a thousand or more species.
An unhealthy gut is, more often than not, the product of a breakdown in this collaboration. Often, it is triggered by displacement of cooperative, commensal species of bacteria by pathogenic bacteria, fungi, viruses, and protozoa. This is why a long course of antibiotics, killing commensal bacteria, is often the prelude to bowel ailments.
It is difficult for the immune system to defeat gut infections without the help of commensal bacteria. Think about what the immune system has to deal with. The ulcers in ulcerative colitis are essentially the equivalent of infected skin abscesses, but in the colon. Here is a description of a bowel lesion in Crohn’s disease:
Ileal lesions in Crohn’s disease (CD) patients are colonized by pathogenic adherent-invasive Escherichia coli (AIEC) able to invade and to replicate within intestinal epithelial cells. [1]
Now imagine an infected skin abscess, but with feces spread over it three times a day, or stomach acid and digestive enzymes. How quickly would you expect it to heal?
Commensal “probiotic” bacteria are like a mercenary army fighting on behalf of the digestive tract. By occupying the interior lining of the digestive tract, they deprive pathogens of a “home base” that is sheltered from immune attack. If commensal bacteria dominate the gut, the immune system can usually quickly defeat infections.
This suggests that introduction of probiotic bacteria to the gut should be therapeutic for bowel disease.
Probiotic Supplements Are Inadequate
Most supermarket probiotics contain Lactobacillus or Bifidobacterium species. These species are specialized for digesting milk; they populate the guts of infants as they start breastfeeding, and are used by the dairy industry to ferment cheeses and yogurt.
These supplements are very effective at fighting acute diarrhea from most food-borne infections. A fistful of probiotic capsules taken every hour will usually quickly supplant the pathogens and end diarrhea.
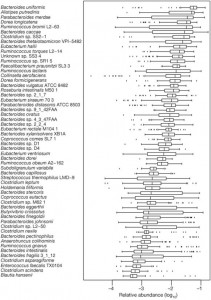
However, against more severe bowel diseases caused by chronic infections and featuring damaged intestinal mucosa, these species are usually not helpful. One issue is that they provide only a tiny part of a healthful adult microbiome. A recent study surveyed the bacterial species in the human gut, and found these species to be most abundant [2]:
As this figure shows, Bacteroides spp. are the most common commensal bacteria, with Bacteroides uniformis alone providing almost 10% of all bacterial genes in the gut. Lactobacillus and Bifidobacterium do not appear among the 57 most abundant species.
This study showed, by the way, that patients with irritable bowel syndrome have 25% fewer types of bacterial gene in their gut than healthy people, and that the composition of bacterial genes in feces clearly distinguishes ulcerative colitis, Crohn’s disease, and healthy patients. In other words, in the bowel diseases a few pathogenic species have colonized the gut and entirely denuded it of about 25% of the commensal species that normally populate the gut. This finding supports the idea that restoring those missing species might be therapeutic for IBS.
Bacterial Replacement Therapies Work
So if IBS patients are missing 25% of the thousand or so species that should populate the gut, or 250 species, and if common probiotics provide only 8 or so species and not the ones that are missing, how are the missing species to be restored?
The answer is simple but icky. Recall that half the dry weight of stool consists of bacteria. A healthy person daily provides a sample of billions of bacteria from every one of the thousand species in his gut. They are in his stool.
So a “fecal transplant” of a healthy person’s stool into the gut of another person will replenish the missing species.
Scientists have known for a long time that this was likely to be an effective therapy, but it is only now entering clinical practice. The New York Times recently made a stir by telling this story:
In 2008, Dr. Khoruts, a gastroenterologist at the University of Minnesota, took on a patient suffering from a vicious gut infection of Clostridium difficile. She was crippled by constant diarrhea, which had left her in a wheelchair wearing diapers. Dr. Khoruts treated her with an assortment of antibiotics, but nothing could stop the bacteria. His patient was wasting away, losing 60 pounds over the course of eight months. “She was just dwindling down the drain, and she probably would have died,” Dr. Khoruts said.
Dr. Khoruts decided his patient needed a transplant. But he didn’t give her a piece of someone else’s intestines, or a stomach, or any other organ. Instead, he gave her some of her husband’s bacteria.
Dr. Khoruts mixed a small sample of her husband’s stool with saline solution and delivered it into her colon. Writing in the Journal of Clinical Gastroenterology last month, Dr. Khoruts and his colleagues reported that her diarrhea vanished in a day. Her Clostridium difficile infection disappeared as well and has not returned since.
The procedure — known as bacteriotherapy or fecal transplantation — had been carried out a few times over the past few decades. But Dr. Khoruts and his colleagues were able to do something previous doctors could not: they took a genetic survey of the bacteria in her intestines before and after the transplant.
Before the transplant, they found, her gut flora was in a desperate state. “The normal bacteria just didn’t exist in her,” said Dr. Khoruts. “She was colonized by all sorts of misfits.”
Two weeks after the transplant, the scientists analyzed the microbes again. Her husband’s microbes had taken over. “That community was able to function and cure her disease in a matter of days,” said Janet Jansson, a microbial ecologist at Lawrence Berkeley National Laboratory and a co-author of the paper. “I didn’t expect it to work. The project blew me away.” [3]
Fecal transplants can be done without a doctor’s help: someone else’s stool can be swallowed or inserted in the rectum. If taking feces orally, swallow a great deal of water afterward to help wash the bacteria through the stomach and its acid barrier.
Dogs and young children sometimes swallow feces. It is unpleasant to consider, but desperate diseases call for desperate measures. Perhaps one day, healthy stools will be available in pleasant-tasting capsules, and sold on supermarket shelves. Not yet.
Attacking Pathogenic Biofilms
Most bacterial species will build fortresses for themselves, called biofilms. These are polysaccharide and protein meshworks that, like bone, become mineralized with calcium and other minerals. These mineralized meshworks are built on bodily surfaces, like the gut lining, and protect bacteria from the immune system, antibiotics, and other bacterial species.
Pathogenic species known to generate biofilms include Legionella pneumophila, S. aureus, Listeria monocytogenes, Campylobacter spp., E. coli O157:H7, Salmonella typhimurium, Vibrio cholerae, and Helicobacter pylori. [4]
Biofilms favor the species that constructed them. So, once pathogens have constructed biofilms, it is hard for commensal species to displace them.
Therapies that dissolve pathogenic biofilms can improve the likelihood of success of probiotic and fecal transplant therapies. Strategies include enzyme supplements, chelation therapies, and avoidance of biofilm-promoting minerals like calcium. Specifically:
- Polysaccharide and protease digesting enzymes. Human digestive enzymes generally do not digest biofilm polysaccharides, but bacterial enzymes that can are available as supplements. Potentially helpful enzymes include hemicellulase, cellulase, glucoamylase, chitosanase, and beta-glucanase. Non-human protease enzymes, such as nattokinase and papain, might also help. [5]
- Chelation therapy. Since biofilms collect metals, compounds that “chelate” or bind metals will tend to gather in biofilms. Some chelators – notably EDTA – are toxic to bacteria. So EDTA supplementation tends to poison the biofilm, driving bacteria out of their fortress-shelter. This prevents them from maintaining it and makes the biofilm more vulnerable to digestion by enzymes and commensal bacteria. It also tends to reduce the population of pathogenic bacteria.
- Mineral avoidance. The supply of minerals, especially calcium, iron, and magnesium, can be a rate-limiting factor in biofilm formation. Removal of calcium can cause destruction of biofilms. [6] We recommend limiting calcium intake while bowel disease is being fought, since the body can meet its own calcium needs for an extended period by pulling from the reservoir in bone. Upon recovery, bone calcium can be replenished with supplements. Iron is another mineral which promotes biofilms and might be beneficially restricted. We do not recommend restricting magnesium.
Some commercial products are available which can help implement these strategies. For instance, Klaire Labs’ InterFase (http://www.klaire.com/images/InterFase_Update_Article.pdf) is a popular enzyme supplement which helps digest biofilms, and a version containing EDTA is available (InterFase Plus).
Attacking Biofilms With Berries, Herbs, Spices, Vinegar, and Whey
Plants manufacture a rich array of anti-microbial compounds for defense against bacteria.
There is reason to believe that traditional herbs and spices, which entered the human diet during the Paleolithic and have been passed down through the generations for tens of thousands of years, were selected by our hunter-gatherer ancestors as much for their ability to promote gut health as for their taste. Dr. Art Ayers notes that:
Plants are adept at producing a wide array of chemicals with refined abilities to block bacterial functions. So when researchers sought chemicals to solve the problem of pathogens forming biofilms, it was natural to test plant extracts for inhibiting compounds. In a recent article [7], D.A. Vattem et al. added extracts from dietary berries, herbs and spices to bacterial pathogens, including the toxin producing Escherichia coli (EC) O157:H7, and checked for the ability to produce a chemical that signals the formation of a biofilm. The effective phytochemicals inhibited the bacteria from recognizing a critical density of bacteria, i.e. quorum sensing, and responding with the production of the biofilm-triggering chemical.
Blueberry, raspberry, cranberry, blackberry and strawberry extracts were effective as quorum sensing inhibitors (QSIs). Common herbs such as oregano, basil, rosemary and thyme were also effective. Turmeric, ginger and kale were also tested and found to contain QSIs. [8]
A few other remedies can weaken biofilms:
- Acetic acid in vinegar can solubilize the calcium, iron, and magnesium in biofilms, removing these minerals and weakening the biofilm; citric acid binds calcium and can disrupt biofilms. [9]
- Lactoferrin, a molecule in milk whey, binds iron and inhibits biofilm formation and growth. [10]
- N-acetylcysteine can destroy or inhibit biofilms. [11]
Conclusion
Fecal transplants are the best probiotic. Tactics to disrupt pathogenic biofilms can assist probiotics in bringing about re-colonization of the digestive tract by commensal bacteria.
Along with a non-toxic diet (discussed in Part II) and nutritional support for the immune system and gut (discussed in Part III), these steps to improve gut flora make up a natural program for recovery from bowel disease.
UPDATE: Please read the cautions by two health professionals, annie and Jesse, about potential dangers of self-treatment with fecal transplants and EDTA. It is always better to pursue these therapies with a doctor’s assistance and monitoring.
Related Posts
Other posts in this series:
- Bowel Disorders, Part I: About Gut Disease July 14, 2010
- Bowel Disease, Part II: Healing the Gut By Eliminating Food Toxins m July 19, 2010
- Bowel Disease, Part III: Healing Through Nutrition July 22, 2010
References
[1] Lapaquette P, Darfeuille-Michaud A. Abnormalities in the Handling of Intracellular Bacteria in Crohn’s Disease. J Clin Gastroenterol. 2010 Jul 7. [Epub ahead of print]. http://pmid.us/20616747.
[2] Qin J et al. A human gut microbial gene catalogue established by metagenomic sequencing. Nature. 2010 Mar 4;464(7285):59-65. http://pmid.us/20203603.
[3] Carl Zimmer, “How Microbes Defend and Define Us,” New York Times, July 12, 2010, http://www.nytimes.com/2010/07/13/science/13micro.html.
[4] Donlan RM. Biofilms: microbial life on surfaces. Emerg Infect Dis. 2002 Sep;8(9):881-90. http://pmid.us/12194761.
[5] Tets VV et al. [Impact of exogenic proteolytic enzymes on bacteria]. Antibiot Khimioter. 2004;49(12):9-13. http://pmid.us/16050494.
[6] Kierek K, Watnick PI. The Vibrio cholerae O139 O-antigen polysaccharide is essential for Ca2+-dependent biofilm development in sea water. Proc Natl Acad Sci U S A. 2003 Nov 25;100(24):14357-62. http://pmid.us/14614140. Geesey GG et al. Influence of calcium and other cations on surface adhesion of bacteria and diatoms: a review. Biofouling 2000; 15:195–205.
[7] Vattem DA et al. Dietary phytochemicals as quorum sensing inhibitors. Fitoterapia. 2007 Jun;78(4):302-10. http://pmid.us/17499938.
[8] Art Ayers, “Spices are Antimicrobial and Inhibit Biofilms,” Dec. 7, 2008, http://herbal-properties.suite101.com/article.cfm/spices_are_antimicrobial_and_inhibit_biofilms.
[9] Art Ayers, “Cure for Inflammatory Diseases,” Sept. 2, 2009, http://coolinginflammation.blogspot.com/2009/09/cure-for-inflammatory-diseases.html. Desrosiers M et al. Methods for removing bacterial biofilms: in vitro study using clinical chronic rhinosinusitis specimens. Am J Rhinol. 2007 Sep-Oct;21(5):527-32. http://pmid.us/17883887.
[10] O’May CY et al. Iron-binding compounds impair Pseudomonas aeruginosa biofilm formation, especially under anaerobic conditions. J Med Microbiol. 2009 Jun;58(Pt 6):765-73. http://pmid.us/19429753.
[11] Cammarota G et al. Biofilm demolition and antibiotic treatment to eradicate resistant Helicobacter pylori: A clinical trial. Clin Gastroenterol Hepatol. 2010 May 14. [Epub ahead of print] http://pmid.us/20478402. Zhao T, Liu Y. N-acetylcysteine inhibit biofilms produced by Pseudomonas aeruginosa. BMC Microbiol. 2010 May 12;10:140. http://pmid.us/20462423.











Did Paul ever wrote the part V?
Yikes, doesn’t sound pleasant! Very helpful post, though, nonetheless. This isn’t applicable at the moment but if it does ever become relevant it sure is good to know! Thanks for sharing.
Hi Paul, what do you think about this italian site?
http://www.omeostatica.eu/articoli/argento-colloidale.html
I can’t understand everything, but in the linked page there is a research about silver citrate complex all in English.
it looks as a very powerful anti microbial element without toxicity.
What do you think about to fix the bowel?
Hi Jules,
http://www.mayoclinic.org/healthy-lifestyle/consumer-health/expert-answers/colloidal-silver/faq-20058061
This isn’t colloidale silver.
Translating the italian page the Author sounds to be aganist colloidal-silver.
The articole and the research talk about silver citrate complex:
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2590638/?report=classic
I think they’re two different thing.
Be very careful regarding ANY medical site’s recommendations. The AMA and the FDA are criminal murderers whose guilt is addressed in almost countless articles and videos available on the Internet and so incriminating, it will be hard to believe our government is so evil.
Coincidentally, in the library yesterday, I was talking to a guy who asked me about colloidal silver and a woman who overheard his question spoke up and told him that colloidal silver had saved her life when medical malpractice would have left her dead. It was a completely unsolicited testimony but her sincerity was visible and emphatic.
Regarding searching medical crimes of the AMA and the FDA, there are dozens of keyword combinations that you will find effective, such as “crimes of the fda” or crimes of the ama… (that guidance WAS effective two years ago, but today it’s not nearly as good).
Why? Because Google is a shill for all the criminal elements of the government and this has become INCREASINGLY obvious over the last few years so that you will do much better searching specific crimes for which you have specific applicable terms because I have seen time after time that Google will post “puff” pieces when keywords specifically ask for incriminating and indicting information. Our government is our enemy and I didn’t believe that ten years ago but with Obama’s hiding his past (and the media’s collusion), I was shocked and alarmed and started doing research. After many HUNDREDS of HOURS of Internet research, the proof of our country’s betrayal of its people is beyond dispute by honest, objective evaluation. Do your own research and the more you do, the more heartbroken you will become.
If you want one example of the crime of pedophilia being covered up by the FBI and the government, use these search terms: “owen bonacci decamp pedophilia” You will see the significance of those people and the relevant video can be watched on YouTube, entitled .
That video (why the name was cut off I don’t know) is entitled “Conspiracy of Silence.”
This is more or less the translating of article:
https://translate.google.com/translate?sl=it&tl=en&js=y&prev=_t&hl=it&ie=UTF-8&u=http%3A%2F%2Fwww.omeostatica.eu%2Farticoli%2Fargento-colloidale.html&edit-text=&act=url
I have suffered from badbreath for several years. Would you suggest fecal transplant?
No. Bad breath is more likely due to acid reflux or some sort of dysbiosis of the oral/nasal/esophageal microbiome. Try improving the small intestine (not the colon, which a fecal transplant would address) and mouth.
Best, Paul
I had bad breath ALL my life! When I got my gut fixed, it went away.
Hi Gary,
I have this same issue. I know it’s bacteria related because my oral hygiene is very good AND when i was on pylera (antibiotics for h pylori) i had clean breath for the first time in my life! A few weeks later the dragon returned.
How exactly did you fix your gut?
Hi Peter,
Glad to reply. Consistent use of a fairly large variety of good probiotics and consistent use of much Aloe Vera (Verapol®) and brief but very beneficial use of Wedderspoon® Manuka honey.
Years ago I ate something that was bad and it wrecked my digestive system because I didn’t catch it (or make any attempt to rectify it) for years. When I started passing undigested food and bleeding a great deal, I realized that it was my poor digestion that was destroying my mind (I was stressed even writing a check!) and started looking for supplements to help me.
I first started taking probiotics and remembered the benefits of Manapol® and sought to get some but found the manufacturer had gone bankrupt and sold the Aloe farm (and processing facility) to some Latin American businessmen and started using it under its new name, Verapol®. The probiotics helped a great deal, but they didn’t do everything I needed and I knew from my history that Aloe was an amazing healing plant. While the Aloe cleared up 95% of the bleeding, the Manuka honey made it 100%. I have continued to take probiotics, aloe (and a wide variety of other supplements for other reasons) ever since.
I tend to credit the Aloe the most (because I like it so much for its variety of benefits) but that is opinion only and not substantiated for I never went to a physician (I despise the murderous AMA & FDA). I think the probiotics were more significant along with eating a variety of things that were gut-friendly and I started them before the Aloe. I’ve been taking quality Aloe 1-3 times a day and the noticeable daily benefit seems to be more significant in my mind than probiotics but that might mean I’m slighting them.
That was about eight years ago and I’m still taking Verapol® and because I like it so much, I might take it forever. I intend to take more Manuka occasionally and I also intend to keep taking probiotics since I’m over 60.
All three played a part.
Wedderspoon® Manuka Honey is expensive–over $40 typically for a ½ kilo but it can do amazing things with no harmful side effects like antibiotics.
If you have access to fresh Aloe and learn how to filet it (and wash all the anthraquinones off it) and enjoy eating it fresh then that’s a great way to take it. I say this because the Aloe industry as a whole cannot be trusted and I wouldn’t recommend any aloe other than Verapol® because I’ve never found any as good.
I hope that helps.
Thanks so much Gary for your detailed reply. I’ve tried many many supplements over the years to treat a general sense of malaise. Interestingly, my routine yearly physical usually has the doctor gushing at how healthy I am – 110/75 bp, good thyroid readings, all the way to very healthy cholesterol levels. Not a single reading outside of the normal range.
I have always sensed that the malaise and fatigue has something to do with my stomach – malabsorption, low stomach acid, gut flora issues etc. I found out last October that I had H-Pylori infection and after completing the Pylera protocol, I now have sinking stools(had floaters as long as I can remember 🙂 ).
A month ago, I took prescript assist – 1 capsule twice a day for 4 days and it completely knocked out pain from an arthritic elbow for the first time in 15 months – it was miraculous! I had to stop though because I started getting signs of bacteria overgrowth – post nasal drip, increased bad breath, lump in throat, smelly feet, etc. I’ve tried many other probiotics in my day but they almost always give me worse breath and/or chest pain (weird reaction I get from 75% of supplements I try. Same reaction from coffee, tea, potatoes, green peppers and Vitamin D – any dose or kind – reactions likely from stomach issues/silent reflux. My stomach no doubt needs a LOT of TLC).
Of all the things I’ve tried, aloe has not been one of them. Thanks and I’ll definitely try that first. I see Verapol on Amazon for $70. It’s rather steep for me so I’ll check other sources first.
FYI – honey gives me brain fog and causes inflammation. Sugar does the same thing, and I can tell because I get a sore lower back, joint pain and soles of feet start to peel, etc.
FYI2 – I’ve recently bought half a dozen half gallon canning jars at Walmart and filled 4 of them so far with veggies for fermentation. I’m readying for serious battle with this stomach issues! 😀 😀
You’re welcome. From what you’re saying, even with the issue you’ve had with honey, I’d definitely suggest Manuka Honey. If it won’t work for you, I’ll buy the balance of your container because I’ve intended to get more anyway. Check myspicesage.com for Manuka. Betterlife.com used to sell Verapol for $50 if you bought two at a time. See if you can find large leaf aloe. I saw some in a store today for $1.39. A few of those should tell you something. Watch YouTube videos on how to filet them. Any bitterness at all and you’re not washing the filet enough.
$70 is too high. $60 is a good price for both the supplier and the customer. Take lecithin every time you take aloe. Do some research on these things.
I’ve got to go because the Library is closing soon, but keep me updated. My email is at gmail and it’s my first initial and my last name
Try Kefir grains and make your own kefir (with milk). I add Stevia to it and love it.
My mother had very bad breath for years. They finally scoped her and found she had a yeast infection in her esophagus. After treatment, her bad breath was one.
Hi Gary,
It’s me again…Thank you for your recommendations below. I tried both the Manuka honey and Aloe Vera (George’s Always Active). Both gave me one significant and strange side effect – weight gain with gynecomastia. My body must be reacting strangely with them.
There’s a big BUT though. They, and Aloe Vera specifically, helped me learn one thing conclusively – bacteria overgrowth is the root cause of so many of my problems. I took the honey first for 14 days, then started on the Aloe. After taking the Aloe for a month, I stopped but since then, I’ve had the deepest and most consistent sleep I can remember. I’ve literally become a morning person. Up and alert at 6 am every single day, even when I’ve stayed out and up late. In addition, my body hair, especially back of legs has sprouted so long, I look like a cave man – for the first time in my life, and I’m almost 40!
The last week has made the bacteria overgrowth theory all more certain because all the old symptoms are back after I took Culturelle probiotics.
Now, after my month long Aloe treatment, I noticed that a little milk or animal fat would give me IBS-D within literally half an hour of finishing the meal. This went on for the last two months and I simply avoided milk and high fat foods. Last Sunday I was researching around and came across multiple sources indicating that lack of gut/colon bacteria can cause this and Culturelle is highly recommended. I figured the month long Aloe dosage had wiped out all my bacteria, good and bad. On Tuesday evening, I bought the Culturelle probiotics and have been taking two a day since. It’s now Sunday morning and for the last 4 mornings, I’ve woken up with horrible brain fog (ringing sound in head) and sour acid taste in my mouth. It takes until around 11am for the fog to clear. This feeling is so familiar for the last 10-15 years it was my every day status.
My question is how do I get/keep bacteria in my lower digestive system and out of my stomach and small intestines? I’m not sure if my stomach acid is strong enough to clear out the bacteria in my stomach or I need to again take the Aloe or some other antibiotics. Any ideas?
So what is the best probiotic to take – without using the above fecal proceedure?
There is no one best probiotic, but we have some recommendations on the Recommended Supplements page.
Hi Paul, I developed quite aggressive periodontitis after an antibiotic course (as well as gut dysbiosis with colon inflammation). I’m planning to have fecal transplants for my gut microbiome, but what could you suggest to improve my mouth microbiome? It seems like there is no option of “saliva transplants”. I have some hope the fecal transplants will have an impact on my mouth microbiome and halt the tooth decay. I’m only 23 so this has been quite distressing. I think my gut was largely ruined by Roaccutane that I was given as a young teenager.
Try rinsing your mouth with salt water multiple times per day. The electrolytes buffer acids and bases, moving the pH toward normal, and this should help restore a normal oral microbiome. Also salt can be antimicrobial.
Hi Paul,
Thank you for all your work and book. I’ve been following closely and I think I finally see the light at the end of the tunnel.
Long story short, I have SIBO that causes acid reflux (silent-LPR) and subsequent problems including chronic bad breath, poor sleep and general malaise and fatigue. I have taken antibiotics including pylera and every time I do, the SIBO subsides, only to return within a short time. Three months ago, I took Aloe Vera for a month and for two months after that, I’ve had the best sleep and most energy I can recall. No acid reflux at all. Apparently the Aloe cleared out my gut bacteria. However, a side effect has been loose stools which I theorized from research was caused by lack of bacteria in the colon.
After taking Culturelle probiotics in the last week, my bloating is back with acid reflux and horrible brain fog in the morning. I figure the bacteria I’ve introduced is staying in my stomach, multiplying from the carbs in my diet and causing all the symptoms again. So I need the bacteria but they also cause me so many problems.
What would you recommend?
Wait to see if my stomach acid will do it’s job – it hasn’t in the past..
Take Aloe Vera again – this will clear all bacteria?
Take Xifaxan – to clear just upper intestine bacteria and keep colon bacteria?
If Xifaxan, will the bacteria still not migrate up after a while?
This article is very detailed and informative. I have an H pylory and was misdiagnosed by gastroenterologist with IBS. I had to pay almost $400 for BioheaLth lab to give me a correct diagnosis. Antibiotics didn’t work but natural remedies did. I am almost cured with multiple remedies but primarily by Mastic gum, Manuka honey, l carnosine, berberine, NAC and intvertase plus enzymes…
You imply that people can without a doctor simply eat sh*t and get a healthy gut and this is so untrue and dangerous! The bacteria will be destroyed before it ever reaches the intestines. What is more, fecal transplant is not known to be effective long-term and is not currently a treatment for IBS, only for c-difficile. DO NOT ATTEMPT FMT WITHOUT A DOCTOR. You can get sick even when doing FMT with a physicians help.
Frequently, I am told that I am the picture of vibrant health. Beyond retirement age, I continue to work, and, yes, the job is stressful. I have a colonoscopy every 5 years because my brother died of colon cancer. All has been fine until today’s procedure. A polyp was found and taken for biopsy. It was a mere 1mm in size.
More troubling to me, however, was learning that the doctor found several diverticulosis pockets. I have always consumed a healthy diet, as described at the times across the decades. True, fiber can be difficult for me, but l am rarely constipated — maybe a couple times a year when I travel. Otherwise, I easily have 3 BM each day. So I am confounded as to what I have done, or failed to do, to bring this on. I fear that this is the beginning of a life-long battle with painful episodes. Paul, do you have any advice?
Hi lana,
I would suggest eating extracellular matrix (soups and stews made with connective tissue, or shellfish), optimizing vitamin A and D at all times, intermittent fasting, circadian rhythm entrainment, 3 egg yolks a day, and bile supports (vitamin C, taurine, glycine).
Best, Paul
Very interesting. I have a complete inability to lose weight. Personal trainer who works me hard 3 times a week, regular walking, busy life, record and consume everything I eat down to coffee/tea and have 1400 calories a day. I hardly eat wheat and very limited sugar & grain. I cannot shift a single pound or fat %. Could the fecal transplant help me or any other suggestions? I’m 3 stone overweight and a recent test showed the beginnings of fatty liver. Please help!
Yvonne,
Watch this youTube (https://www.youtube.com/watch?v=v9Aw0P7GjHE&t=713s) of Dr Jason Fung, who talks about intermittent fasting and extended fasting. He also discusses why calorie restriction, like yours is detrimental to weight loss goals because it slows down your basal metabolic rate. He also had a podcast series called “The Obesity Code Podcast” It is well worth listening to.
PS I know I have gut issues due to diarrhoea, wind and bloating and I take inner leaf aloe Vera, soaked flax seed and a good probiotic ((Cytoplan fosodopholylis) plus CQ10 and B vits but my tummy isn’t right.
Yvonne, find a gastro who will do the SIBO breath test. I had a similar experience eating 1200 calories a day and not losing weight. Found out I have over colonization of archaea – who are scrappy little organisms capable of extracting extra calories from the carbs you eat. If you are experiencing insomnia and or constipation, you need to fix those. Melatonin and magnesium for those.
Sorry, just realized you said diahrrea not constipation.
Hi Paul…
Wondering if you have any views on kefir….?
We’re generally supportive of fermented foods and fermented dairy, but those who have fungal infections should avoid yeast-fermented foods such as kefir.
Best, Paul
I’ve had ibsd all my life, over 50 years. I think it’s due to radiation I had as an infant. I’ve been on Lotronex, then viberzi and now trying xifaxan. I drink homemade dairy kefir daily. Any suggestions for me? I just want to know what a normal gut feels like for once in my life.
Thank you very much for this series of publications, Mr. Jaminet. It looks like extremely relevant and unique information, I’ve never read anything like it anywhere else. I suffer from Crohn’s disease, so I am going to put them into practice, and in the future I will tell you how it has gone.
Kind regards,
And best wishes for the new year.
Paul,
Many Ray Peat followers talk about the bowel-cleansing effects of cooked white button mushrooms. For example:
http://www.thenutritioncoach.com.au/tag/mushrooms/
In my experience, eating more than 1-2 well cooked mushrooms causes me a lot of gas and digestive upset: bowel pain in the low abdomen that I don’t typically experience.
My instinct is that this is some kind of dying off of pathogenic bacteria, but I am also hesitant to experiment more with them because i’ve seen elsewhere on this site that you recommend people with fungal infections abstain from eating fungal foods. I have symptoms of a chronic fungal infection so wanted to ask your opinion on mushrooms in this context.
Thanks
Hello again.
I am very sad, today I received the blood test values and the inflammation markers do not improve. Crohn’s disease is still active.
It has been three months since I started treatment. I thought I was getting better because now I go to the bathroom less often. But I didn’t.
I am on azathioprine (imurel) and adalimumab (Humira) (TNF-inhibiting). I also spent two months on corticosteroids. And three weeks ago I started LDN.
I follow a low-Fodmap diet and paleo-autoimmune (AIP) from the beginning. I incorporated three egg yolks a day, rice, and ghee. Also coconut oil for microbial effects. I can’t tolerate a lot of vegetables, so recently I had to give it up. My diet has no toxins. I have tried keto recently, but the analysis values showed very high TSH and somewhat low T4 values, so just in case I stopped the ketogenic diet.
I take the supplements recommended by Paul, and follow the recommendations to balance vitamin D and A, have good circadian rhythms, do intermitent fasting, and so on.
That’s why I’m so frustrated. The disease is still active and I’m afraid of the future. There are no more medications left that I can be put on. I imagine they will prescribe another course of corticosteroids again. I hope I don’t get to need surgery.
Sorry for this long message. I write it partly as an outlet, and partly with a pinch of hope in case someone reads it and has something to contribute. I don’t know what I can do anymore.
Best,
H