A healthy gut is a multi-species society: it is the cooperative product of the human body with trillions of bacterial cells from a thousand or more species.
An unhealthy gut is, more often than not, the product of a breakdown in this collaboration. Often, it is triggered by displacement of cooperative, commensal species of bacteria by pathogenic bacteria, fungi, viruses, and protozoa. This is why a long course of antibiotics, killing commensal bacteria, is often the prelude to bowel ailments.
It is difficult for the immune system to defeat gut infections without the help of commensal bacteria. Think about what the immune system has to deal with. The ulcers in ulcerative colitis are essentially the equivalent of infected skin abscesses, but in the colon. Here is a description of a bowel lesion in Crohn’s disease:
Ileal lesions in Crohn’s disease (CD) patients are colonized by pathogenic adherent-invasive Escherichia coli (AIEC) able to invade and to replicate within intestinal epithelial cells. [1]
Now imagine an infected skin abscess, but with feces spread over it three times a day, or stomach acid and digestive enzymes. How quickly would you expect it to heal?
Commensal “probiotic” bacteria are like a mercenary army fighting on behalf of the digestive tract. By occupying the interior lining of the digestive tract, they deprive pathogens of a “home base” that is sheltered from immune attack. If commensal bacteria dominate the gut, the immune system can usually quickly defeat infections.
This suggests that introduction of probiotic bacteria to the gut should be therapeutic for bowel disease.
Probiotic Supplements Are Inadequate
Most supermarket probiotics contain Lactobacillus or Bifidobacterium species. These species are specialized for digesting milk; they populate the guts of infants as they start breastfeeding, and are used by the dairy industry to ferment cheeses and yogurt.
These supplements are very effective at fighting acute diarrhea from most food-borne infections. A fistful of probiotic capsules taken every hour will usually quickly supplant the pathogens and end diarrhea.
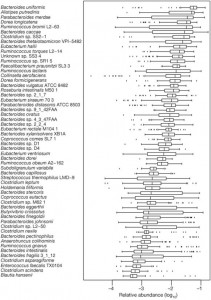
However, against more severe bowel diseases caused by chronic infections and featuring damaged intestinal mucosa, these species are usually not helpful. One issue is that they provide only a tiny part of a healthful adult microbiome. A recent study surveyed the bacterial species in the human gut, and found these species to be most abundant [2]:
As this figure shows, Bacteroides spp. are the most common commensal bacteria, with Bacteroides uniformis alone providing almost 10% of all bacterial genes in the gut. Lactobacillus and Bifidobacterium do not appear among the 57 most abundant species.
This study showed, by the way, that patients with irritable bowel syndrome have 25% fewer types of bacterial gene in their gut than healthy people, and that the composition of bacterial genes in feces clearly distinguishes ulcerative colitis, Crohn’s disease, and healthy patients. In other words, in the bowel diseases a few pathogenic species have colonized the gut and entirely denuded it of about 25% of the commensal species that normally populate the gut. This finding supports the idea that restoring those missing species might be therapeutic for IBS.
Bacterial Replacement Therapies Work
So if IBS patients are missing 25% of the thousand or so species that should populate the gut, or 250 species, and if common probiotics provide only 8 or so species and not the ones that are missing, how are the missing species to be restored?
The answer is simple but icky. Recall that half the dry weight of stool consists of bacteria. A healthy person daily provides a sample of billions of bacteria from every one of the thousand species in his gut. They are in his stool.
So a “fecal transplant” of a healthy person’s stool into the gut of another person will replenish the missing species.
Scientists have known for a long time that this was likely to be an effective therapy, but it is only now entering clinical practice. The New York Times recently made a stir by telling this story:
In 2008, Dr. Khoruts, a gastroenterologist at the University of Minnesota, took on a patient suffering from a vicious gut infection of Clostridium difficile. She was crippled by constant diarrhea, which had left her in a wheelchair wearing diapers. Dr. Khoruts treated her with an assortment of antibiotics, but nothing could stop the bacteria. His patient was wasting away, losing 60 pounds over the course of eight months. “She was just dwindling down the drain, and she probably would have died,” Dr. Khoruts said.
Dr. Khoruts decided his patient needed a transplant. But he didn’t give her a piece of someone else’s intestines, or a stomach, or any other organ. Instead, he gave her some of her husband’s bacteria.
Dr. Khoruts mixed a small sample of her husband’s stool with saline solution and delivered it into her colon. Writing in the Journal of Clinical Gastroenterology last month, Dr. Khoruts and his colleagues reported that her diarrhea vanished in a day. Her Clostridium difficile infection disappeared as well and has not returned since.
The procedure — known as bacteriotherapy or fecal transplantation — had been carried out a few times over the past few decades. But Dr. Khoruts and his colleagues were able to do something previous doctors could not: they took a genetic survey of the bacteria in her intestines before and after the transplant.
Before the transplant, they found, her gut flora was in a desperate state. “The normal bacteria just didn’t exist in her,” said Dr. Khoruts. “She was colonized by all sorts of misfits.”
Two weeks after the transplant, the scientists analyzed the microbes again. Her husband’s microbes had taken over. “That community was able to function and cure her disease in a matter of days,” said Janet Jansson, a microbial ecologist at Lawrence Berkeley National Laboratory and a co-author of the paper. “I didn’t expect it to work. The project blew me away.” [3]
Fecal transplants can be done without a doctor’s help: someone else’s stool can be swallowed or inserted in the rectum. If taking feces orally, swallow a great deal of water afterward to help wash the bacteria through the stomach and its acid barrier.
Dogs and young children sometimes swallow feces. It is unpleasant to consider, but desperate diseases call for desperate measures. Perhaps one day, healthy stools will be available in pleasant-tasting capsules, and sold on supermarket shelves. Not yet.
Attacking Pathogenic Biofilms
Most bacterial species will build fortresses for themselves, called biofilms. These are polysaccharide and protein meshworks that, like bone, become mineralized with calcium and other minerals. These mineralized meshworks are built on bodily surfaces, like the gut lining, and protect bacteria from the immune system, antibiotics, and other bacterial species.
Pathogenic species known to generate biofilms include Legionella pneumophila, S. aureus, Listeria monocytogenes, Campylobacter spp., E. coli O157:H7, Salmonella typhimurium, Vibrio cholerae, and Helicobacter pylori. [4]
Biofilms favor the species that constructed them. So, once pathogens have constructed biofilms, it is hard for commensal species to displace them.
Therapies that dissolve pathogenic biofilms can improve the likelihood of success of probiotic and fecal transplant therapies. Strategies include enzyme supplements, chelation therapies, and avoidance of biofilm-promoting minerals like calcium. Specifically:
- Polysaccharide and protease digesting enzymes. Human digestive enzymes generally do not digest biofilm polysaccharides, but bacterial enzymes that can are available as supplements. Potentially helpful enzymes include hemicellulase, cellulase, glucoamylase, chitosanase, and beta-glucanase. Non-human protease enzymes, such as nattokinase and papain, might also help. [5]
- Chelation therapy. Since biofilms collect metals, compounds that “chelate” or bind metals will tend to gather in biofilms. Some chelators – notably EDTA – are toxic to bacteria. So EDTA supplementation tends to poison the biofilm, driving bacteria out of their fortress-shelter. This prevents them from maintaining it and makes the biofilm more vulnerable to digestion by enzymes and commensal bacteria. It also tends to reduce the population of pathogenic bacteria.
- Mineral avoidance. The supply of minerals, especially calcium, iron, and magnesium, can be a rate-limiting factor in biofilm formation. Removal of calcium can cause destruction of biofilms. [6] We recommend limiting calcium intake while bowel disease is being fought, since the body can meet its own calcium needs for an extended period by pulling from the reservoir in bone. Upon recovery, bone calcium can be replenished with supplements. Iron is another mineral which promotes biofilms and might be beneficially restricted. We do not recommend restricting magnesium.
Some commercial products are available which can help implement these strategies. For instance, Klaire Labs’ InterFase (http://www.klaire.com/images/InterFase_Update_Article.pdf) is a popular enzyme supplement which helps digest biofilms, and a version containing EDTA is available (InterFase Plus).
Attacking Biofilms With Berries, Herbs, Spices, Vinegar, and Whey
Plants manufacture a rich array of anti-microbial compounds for defense against bacteria.
There is reason to believe that traditional herbs and spices, which entered the human diet during the Paleolithic and have been passed down through the generations for tens of thousands of years, were selected by our hunter-gatherer ancestors as much for their ability to promote gut health as for their taste. Dr. Art Ayers notes that:
Plants are adept at producing a wide array of chemicals with refined abilities to block bacterial functions. So when researchers sought chemicals to solve the problem of pathogens forming biofilms, it was natural to test plant extracts for inhibiting compounds. In a recent article [7], D.A. Vattem et al. added extracts from dietary berries, herbs and spices to bacterial pathogens, including the toxin producing Escherichia coli (EC) O157:H7, and checked for the ability to produce a chemical that signals the formation of a biofilm. The effective phytochemicals inhibited the bacteria from recognizing a critical density of bacteria, i.e. quorum sensing, and responding with the production of the biofilm-triggering chemical.
Blueberry, raspberry, cranberry, blackberry and strawberry extracts were effective as quorum sensing inhibitors (QSIs). Common herbs such as oregano, basil, rosemary and thyme were also effective. Turmeric, ginger and kale were also tested and found to contain QSIs. [8]
A few other remedies can weaken biofilms:
- Acetic acid in vinegar can solubilize the calcium, iron, and magnesium in biofilms, removing these minerals and weakening the biofilm; citric acid binds calcium and can disrupt biofilms. [9]
- Lactoferrin, a molecule in milk whey, binds iron and inhibits biofilm formation and growth. [10]
- N-acetylcysteine can destroy or inhibit biofilms. [11]
Conclusion
Fecal transplants are the best probiotic. Tactics to disrupt pathogenic biofilms can assist probiotics in bringing about re-colonization of the digestive tract by commensal bacteria.
Along with a non-toxic diet (discussed in Part II) and nutritional support for the immune system and gut (discussed in Part III), these steps to improve gut flora make up a natural program for recovery from bowel disease.
UPDATE: Please read the cautions by two health professionals, annie and Jesse, about potential dangers of self-treatment with fecal transplants and EDTA. It is always better to pursue these therapies with a doctor’s assistance and monitoring.
Related Posts
Other posts in this series:
- Bowel Disorders, Part I: About Gut Disease July 14, 2010
- Bowel Disease, Part II: Healing the Gut By Eliminating Food Toxins m July 19, 2010
- Bowel Disease, Part III: Healing Through Nutrition July 22, 2010
References
[1] Lapaquette P, Darfeuille-Michaud A. Abnormalities in the Handling of Intracellular Bacteria in Crohn’s Disease. J Clin Gastroenterol. 2010 Jul 7. [Epub ahead of print]. http://pmid.us/20616747.
[2] Qin J et al. A human gut microbial gene catalogue established by metagenomic sequencing. Nature. 2010 Mar 4;464(7285):59-65. http://pmid.us/20203603.
[3] Carl Zimmer, “How Microbes Defend and Define Us,” New York Times, July 12, 2010, http://www.nytimes.com/2010/07/13/science/13micro.html.
[4] Donlan RM. Biofilms: microbial life on surfaces. Emerg Infect Dis. 2002 Sep;8(9):881-90. http://pmid.us/12194761.
[5] Tets VV et al. [Impact of exogenic proteolytic enzymes on bacteria]. Antibiot Khimioter. 2004;49(12):9-13. http://pmid.us/16050494.
[6] Kierek K, Watnick PI. The Vibrio cholerae O139 O-antigen polysaccharide is essential for Ca2+-dependent biofilm development in sea water. Proc Natl Acad Sci U S A. 2003 Nov 25;100(24):14357-62. http://pmid.us/14614140. Geesey GG et al. Influence of calcium and other cations on surface adhesion of bacteria and diatoms: a review. Biofouling 2000; 15:195–205.
[7] Vattem DA et al. Dietary phytochemicals as quorum sensing inhibitors. Fitoterapia. 2007 Jun;78(4):302-10. http://pmid.us/17499938.
[8] Art Ayers, “Spices are Antimicrobial and Inhibit Biofilms,” Dec. 7, 2008, http://herbal-properties.suite101.com/article.cfm/spices_are_antimicrobial_and_inhibit_biofilms.
[9] Art Ayers, “Cure for Inflammatory Diseases,” Sept. 2, 2009, http://coolinginflammation.blogspot.com/2009/09/cure-for-inflammatory-diseases.html. Desrosiers M et al. Methods for removing bacterial biofilms: in vitro study using clinical chronic rhinosinusitis specimens. Am J Rhinol. 2007 Sep-Oct;21(5):527-32. http://pmid.us/17883887.
[10] O’May CY et al. Iron-binding compounds impair Pseudomonas aeruginosa biofilm formation, especially under anaerobic conditions. J Med Microbiol. 2009 Jun;58(Pt 6):765-73. http://pmid.us/19429753.
[11] Cammarota G et al. Biofilm demolition and antibiotic treatment to eradicate resistant Helicobacter pylori: A clinical trial. Clin Gastroenterol Hepatol. 2010 May 14. [Epub ahead of print] http://pmid.us/20478402. Zhao T, Liu Y. N-acetylcysteine inhibit biofilms produced by Pseudomonas aeruginosa. BMC Microbiol. 2010 May 12;10:140. http://pmid.us/20462423.











Very well done Paul! Great information, thanks!
Besides the fantastic Art Ayers, the most informative and complete text on biofilms I have read was Anju Usman M.D. “Gut Recovery Program: A New Approach To Treating Chronic Gastrointestinal Infections” that can be viewed and downloaded here:
http://www.autismone.com/content/gut-recovery-program-new-approach-treating-chronic-gastrointestinal-infections
Many of your suggestions and much, much more are there!
Thanks, Mario! Great link. It’s nice to see doctors looking to natural healing methods that cooperate with the body instead of fighting it as many drugs do.
Its interesting that his autism program is entirely focused on the gut, and he got autism improvements from a gut health program: 8 of 20 parents noted language improvements, and 11 of 20 behavior improvements. I wasn’t aware that autism kids were so severely affected by intestinal problems.
One point which is tangentially touched on in Dr. Usman’s presentation: Pathogenic biofilms can collect heavy metals like lead, mercury, and others in addition to calcium, iron, and magnesium. When biofilms are disrupted these toxic metals can be released at once, creating poisoning symptoms. Toxicity can be relieved with charcoal (which has a large surface area which binds metals, and is excreted with the stool). In general, exposure to heavy metals will make gut problems worse due to concentration of the toxins in biofilms. So people who have gut problems and a history of exposure to heavy metals should keep that in mind when working on their gut.
Again, it’s great to see this type of medicine gaining currency. This is what really works. Note that Dr. Usman is a family practitioner in Naperville, Illinois, not a big-shot doctor at a research hospital! But a smart man who reads the literature and synthesizes it creatively for the good of his patients.
Yes, it’s really amazing the variety of problems/diseases gut dysbiosis can be involved!
Only a small correction: Dr. Usman is not a guy, she is a woman!
(http://www.autismpedia.org/wiki/index.php?title=Protocols/Usman)
Oops! Thanks, Mario.
paul, i found the following probiotic species to be of special benefit:
http://en.wikipedia.org/wiki/Saccharomyces_boulardii
i just recently switched from the standard garden of life “primal defense” probiotic to the “ultra” version, which is basically the same, but also includes Saccharomyces Boulardii.
what a difference this one species has made! i now can eat stuff like certain fruits or even egg-white protein powder that i knew instantly created an inflamed and swollen belly, without any such effect whatsoever! and this after only a 24h phase of heavy “loading” with the new ultra formula. so it definitely makes a difference, and everyone that suspects a gut infection should try it! Saccharomyces Boulardii is also available as a separate supplement of course.
with regard to biofilm, i just recently listened to an episode of byron richards (way underrated) “weekly wellness update” podcast, where he mentions that a new study found niacinamide to be a very effective biofilm disruptor (surprisingly). his always fun and informative podcasts can be found here: http://www.wellnessresources.com/rss/podcast/
Paul,
I’m Chris from The Healthy Skeptic.
I just wanted to complement you on this fantastic series. I’ve been researching gut health for more than ten years, and it’s rare for me to come across a body of work that I so thoroughly agree with. I’m impressed by the depth of your investigation and you have certainly covered all of the important bases.
I was planning on writing a series on gut health after the “diabesity” series I just started, but now I don’t have to. I can just refer my readers and patients here!
I’m a huge believer in fecal bacteriotherapy, and I think it will be much more common as a treatment in the coming years. The clinic in Sydney, Australia that developed the procedure (Centre for Digestive Disease) likes to refer to it as an organ transplant. They argue, quite defensibly, that the gut flora should be considered as an internal organ as it meets all of the defining criteria.
The only trouble with it as a treatment is that there are so few people these days with good gut flora. Nearly every patient I see has gut symptoms, which are indicative of dysregulated flora. Almost everyone alive in the modern world has taken antibiotics, eaten a poor diet, or engaged in any number of other behaviors that adversely affect the gut flora. This means that the pool of truly suitable donors is quite small.
I bought the book for the same reason I will refer people here. I thought I’d have to write a guide for my patients with gut problems, but I’m hoping your book has relieved me of that burden. I use the GAPS diet with them now, which is effective, but needs some refinement IMO.
Thanks again for your great work. I’ll be in touch, as I had quite a few thoughts and questions after reading this series and other articles on your blog that I’d love to discuss.
Chris
Hi Chris,
I’m so delighted to hear from you, since I discovered The Healthy Skeptic a few months ago I’ve become a big fan. I’m glad you like these posts.
I’ll send you an email separately, but please make yourself at home!
Paul
Interesting post ! I’d hoped there was an alternative to… well, shit. Aren’t there any commercial probiotics of some utility ?
Hi Albedo,
Some probiotics are helpful, just not as helpful as feces. Qualia’s suggestion above of the Garden of Life Primal Defense Ultra is good, that has B. subtilis which is good at fighting a number of gut pathogens, as well as the beneficial yeast S. boulardii. I used Threelac, which has B. subtilis, for a long time with some benefit. Whether these will help depends on your specific gut pathology.
Best, Paul
Woah, this post is very, very informative, especially the section about fecal transplant.
I first eliminated the thought of trying that to heal my gut of whatever is causing my leaky gut/dysbiosis because I though it would have to be done by a doctor and no here will go for that.
My diet as been very similar to the perfect health diet now for close to a year and I tried every probiotic and macronutrient ratio out there. Nothing does. Doctors are of no help either.
I knew about the SCD diet (specific carbohydrate diet) for a while and that they don’t recommend bifidus strains, especially for those with flora problems in their small intestines (bifidus is said to colonize the colon, but can overgrow in the small intestine when someone doesn’t have to right bacteria present). I didn’t listen to that though and I’ve always had probiotics containing bifidobacterium as well as acidophilus.
I’ve cut the bifidobacterium and now have about 1 trillion CFUs of acidophilus per day (the custom probiotics brand) and I now start to see marginal relief, but only very marginal.
I’m now pretty sure bifidobacterium was hindering my results.
What I’m interested to know is if undergoing some kind of home fecal transplant treatment could cause to same problem of colon species invading the small intestine.
Also, as Chris from the Healthy Skeptic mentioned, the fact that nobody today seem to have a healthy diet, can this be a problem to get a good fecal sample? Should I choose a relative that seem to have the best diet or one who seem to be the healthiest, regardless of health?
Any danger associated to possible pathogens present in the donor’s fecal matter?
I understand that this is a lot of specific questions, but feel free to shoot me an email if the comment board is not a good place for such discussion. Any advice on this could possibly help heal a problem that I’ve been dealing with for the last 16 years and that has made my whole life close to a nightmare.
I am glad that I found this website. Lots of great information. I have a quick question if you don’t mind, I am pretty desperate.
About five years ago I began antibiotic treatment for acne. Over the course of the next year and a half I was prescribed one antibiotic after another. After none of that worked to improve my acne I was on Accutane for 3 months.
Roughly 6 months after starting the antibiotics I began getting some GI problems. Some light cramps, some light bloating, LOTS of borborygmi/stomach noises. I also just felt sub-par generally. But the stomach noises have been the biggest problem. Bowel movements have always been good. There is normal gas levels, but there seems to be a correlation between the amount of stomach noise and the amount gas; lots of gas, lots of stomach noise. I found beer and some other foods to make it much worse.
I was a pretty shy guy before any of this, and the stomach noises were lifestyle crippling. Social gatherings and classrooms have become terrifying.
Originally, I thought that it was SIBO, but an endoscopy a couple of weeks ago ruled that out. Now candida is the main suspect, especially since the problem started before my course of antibiotics was finished. A white tongue, jock itch and a toenail fungus suggest that a systemic fungal infection might be involved.
The endoscopy didn’t see any candida in the small intestine, but it wasn’t tested for in the culture, and only the duodenum was checked.
Since the noises are generated by gas getting squashed, might candida impair the rhythm of peristalsis?
My doctor wants me to take an colonoscopy next, for obvious reasons I don’t want to take one, nor do I think that it would be useful.
I have been following a lot of your diet recommendations. I do include high fat dairy products, like butter and cream and I also include live yogurt and kefir. I also go a lot higher in starch as I have seen you recommend on your blog for fungi. I supplement vitamin D and magnesium. The yogurt and kefir have all but cleared by jock itch, so it’s some progress at least.
Why do you recommend high dose iodine over an anti fungal for fungal infections? Would a large amount of iodine not also kill bacteria? What are the problems with an anti fungal, do fungi have an important role in the gut?
I realize that this is a lot to expect you to read through, I would be happy to pay for your help.
Greg.
Hi Greg,
This is very similar to what happened to me. I developed an apparently systemic candidal infection and rosacea during 1-yr antibiotic treatment for acne (which was followed by Accutane), and that was the precursor to a Chlamydophila pneumoniae infection of the brain and nerves that progressed for the next 15 years. During that time I would have frequent flare-ups of the fungal infection including skin infections and thrush.
I recommend all sorts of things against fungal infections, including anti-fungal drugs if you can get your doctor to prescribe them. However, anti-fungal drugs have a poor record against these infections, and the longer you take them the less well they work. Rotate antifungal drugs if you can. But for a cure you have to have a complete diet, nutritional, probiotic, and antifungal effort. And it will take time.
So it’s not that I recommend iodine “over” anything, it’s just that iodine is a free benefit, it will help and won’t hurt anything else.
Yes, iodine also helps against bacteria.
Fungi are not known to be important to gut health. Some people get benefit from probiotic fungal species like Saccharomyces boulardii, others are harmed by them. I don’t recommend such supplements if you have any problems with fungi, they can produce a damaging fungemia.
A colonoscopy could be helpful and isn’t dangerous, but colonoscopies don’t have a good record of detecting fungal infections. I’m not sure why.
I don’t know what causes the noises, I had noises too but not so loud that they would prevent me from socializing.
Things I found helpful were whey powder, B. subtilis / Threelac supplements, kolorex/horopito, iodine, vitamin C, selenium, starch. But there is no magic bullet.
Thanks very much, Paul. I appreciate it. Lots of information there, I will order those supplements today.
For stomach noise, check out the medical term
borborygmi
I know, it is very odd word and it looks like spam, but it is sometimes present with gluten intolerance/celiac.
If there’s a list of the most common species then why not make a supplement of them? Moreso, as per Peter’s FIAF posts, it would be interesting to take samples from very lean individuals and see what they have in common. Everything takes such a long time…
Late to the discussion, but…
Before considering a fecal transplant, the donor would be evaluated for quality of stool flora. Just because someone appears healthy, doesn’t necessarily translate into healthy gut flora.
Second, I have to quibble just a bit with the advice on how to orally ingest feces. Patients would have a nasal intestinal tube inserted and the solution (donor fecal material in normal saline solution) would be injected through the tube to be delivered directly into the small intestine. They would not taste or come into direct contact with the solution until it was delivered directly to the small intestine.
Fecal material should not make contact with the mouth, as there would be increased risk of aspiration (gag reflect, anyone?), as well as flora destruction by saliva and gastric acid.
Rectal instillation would be most likely, and that would be with a rectal tube which is inserted far beyond what a fleets enema type nozzle would reach, so as to effect maximal retention of the solution.
This is NOT a DIY procedure – at least, as of yet.
Congrats on your book launch! Will you be doing any in person book signings?
Hi annie,
Thank you very much for your professional advice!
It will be nice to see this procedure become more common, so that doctors can optimize both samples and procedure.
We’ve planned for online distribution only, so no in-person signing events are planned. But if any bookstores are interested, we’d be delighted to do an event. We are signing books however, see http://perfecthealthdiet.com/?p=804.
Best, Paul
I’ve dealt with crohn’s disease (primarily of the small bowel-jejunum, ilium) for years. i’ve avoided meds and have instead focused on dietary and lifestyle changes as my medicine. i was on antibiotics for 6 years for acne and believe this led to my disease. studies are now just coming out showing a link to antibiotics (for acne) and crohn’s even though just about every GI doc will say there is no association. i’ve read the research regarding stool transplants (primarily in treating c diff infections) and have also thought it would be of benefit for IBD as well (although the research is not there yet). i have a 3 year old daughter, who has never been on antibiotics, eats a healthy diet and is very healthy with no GI issues and still happens to be in diapers. curiosity and desperation finally got the best of me one day when I was changing diapers and I decided to go for it. I ate about a tablespoonful for her stool along with plenty of water. 2 days later I became very sick with severe diarrhea, fever/chills and body aches. this lasted about 2 days and then resolved. my Crohn’s symptoms have since improved some, but are still present. i have 2 questions…what role do stool transplants play in diseases of the small bowel? one would think they would be more beneficial in treating large bowel disease. none of the literature regarding stool transplants mention the symptoms that I developed. could this have been some type of “die off” reaction? i’ve toyed with trying another round in the near future to see if things would continue to improve. thoughts?
Hi Steve,
I was on antibiotics for acne for one year and that was the start of all my troubles.
If you have a damaged gut, then any new bacteria is likely to give you trouble. When I first started the Threelac B. subtilis probiotic that I mentioned to Greg, I had a two-day infection/fever. So I’m not too surprised to hear of a few-day illness until your immune system got the hang of those new germs.
I do think the new species may have played a part in your Crohn’s improvement.
However, stool transplants are much more likely to help ulcerative colitis / colonic problems than small bowel disease, since most fecal species are derived from the colon.
As annie has just warned us, the risks are higher and rewards lower for oral ingestion intended for the small intestine. Also, you may have gotten a lot of the benefit from the first round, so the second round might not do as much good.
On the other hand, as annie suggests, if a professional did it it might be more effective.
You have to weigh pros and cons and risks for yourself. It would be great if you could find a specialist with clinical experience in this matter to advise you.
Hey Paul,
Reading through this article, I noticed some things you might want to revise. Up until the section on bacterial replacement therapies, everything looks good. I can even agree that fecal transplantation DOES work well for certain cases, but do you really think it’s wise to suggest that people can try it without the supervision of a physician? There’s a reason that separating our waste from our food and water is so effective at preventing many diseases. Granted, we don’t see polio or cholera much in the US, and it would be crazy to consume the feces of someone who was obviously suffering from E. coli O157:H7 or some other diarrheal disease, but it’s not safe to assume that someone’s gut microbes are harmless and beneficial just because the person looks healthy.
Remember Typhoid Mary? http://en.wikipedia.org/wiki/Typhoid_Mary She was a healthy woman who continuously spread Salmonella typhimurium, typhoid fever, to other people, leading to the deaths of at least three. I would venture to say that swallowing her feces would definitely not make anyone feel better. That’s one risk.
Another is the pork tapeworm, Taenia solium. Having the worm itself is not too bad, and might actually help alleviate certain diseases such as Crohn’s. But if you swallow the eggs, which are continually coming out of someone who carries the worm, they will migrate to various tissues and form cysts there, including the brain, causing neurocysticercosis, a serious condition: http://en.wikipedia.org/wiki/Neurocysticercosis. If you swallow the feces of someone who carries such a tapeworm, who seems healthy outwardly, it is a risk.
Now, it is possible to test someone’s feces for these organisms, but does the average person have the knowledge and resources to do such tests without help from a doctor? It seems wise to warn your readers of these risks, at least.
Next, I have a some questions about the sections on biofilms. First, about chelation and mineral avoidance. All organisms, including good and bad microbes in addition to we ourselves, require minerals such as iron. Keeping iron away from microbes is actually one way in which our body defends itself from harmful bacteria. It seems like extended use of EDTA and mineral avoidance could lead to mineral deficiency; it seems wise to warn about this.
The paper you cite for evidence of vinegar as a biofilm disruptor didn’t study vinegar, nor did it study gut biofilms. Also, the citation for lactoferrin was not studying gut biofilms either. Is it certain that treatments that work in the respiratory system also work in the gut?
Please let me know what you think of my suggestions.
Hi Jesse,
Those are all excellent suggestions/critiques.
1) On self-treatment.
In writing this I came more from the perspective of a former chronic disease patient who faced frequent resistance from doctors to providing any kind of speculative care. I think you know how cautious health professionals are about experimental treatments.
Obviously it would be better if this therapy could be obtained from a doctor, with careful screening of the transplant. I hope the therapy becomes more available! Everyone who is considering a fecal transplant should try to get it from a doctor first.
But what is someone to do who has ulcerative colitis and conventional therapies are not working, and doctors refuse to offer a fecal transplant?
He has to balance the risks of self-treatment against the benefits.
As the Typhoid Mary example illustrates, the risks are real. Yet, on the other hand, coprophagia is very common among animals and not uncommon even among humans, and rarely leads to disease.
And tests to date on ulcerative colitis have been very positive.
So, if people are in the position of having to choose between self-treatment and no treatment, they should at least be aware that there is an option that might help them.
Now maybe fecal bacteriotherapy is entering the mainstream and people can find doctors to do it. If so, I withdraw my suggestion and recommend that everyone find a doctor or specialist for the procedure.
2) Yes, mineral deficiencies are a risk. I would not recommend very long-term EDTA supplementation for that reason. So yes, I should have a warning. Hopefully this is being done under doctor’s monitoring, with an eye out for anemia or other dangers.
3) Cites: That’s cite [9] which cites two sources, an Art Ayers post and a paper. The vinegar idea comes from the Art Ayers post. The biofilms were studied in vitro which is where nearly all biofilm disruptors are studied; it’s hard to study the gut in vivo, even in animals.
There is always uncertainty whether treatments that work in vitro will translate in vivo. I think that’s an open question for research.
So, I like all of your comments/suggestions. I’ll do a brief update to the post encouraging readers to look at the comments for cautions about dangers.
Best, Paul
Hey Paul,
Thank you for considering my comments. I’m glad they were helpful, though I’m not a health professional so much as a research microbiologist who takes an interest in this subject. I suppose in some cases the benefits of unsupervised fecal transplant may outweigh the risks, as long as one is duly cautious.
With regard to the acetic acid recommendation, I recently came across this article: http://www.ncbi.nlm.nih.gov/pubmed/19903265?dopt=Abstract
It suggests that increased production of acetic acid and other organic acids by gut microbes may play a role in inflammatory bowel disease. It seems to me that trying to treat this condition with additional acetic acid may not be helpful (since the microbes must be able to tolerate the acid they produce), and may exacerbate the disease. At best, the benefits are uncertain. What do you think?
Thanks, Jesse, for the very interesting link.
I recall that at the time of this post I had difficulty finding papers showing a benefit for acetic acid, but I included vinegar out of respect for Art Ayers and traditional remedies.
It does seem that acetic acid is positively harmful in rats.
Malic acid, found in apple cider vinegar, is more likely to be helpful, but poorly tested.
It’s interesting that in your paper Lactobacillus is correlated with IBS. Maybe probiotics and yogurt aren’t so good for you!
I found the trend of Lactobacillus interesting too. It might be that certain species, or even just certain strains, are beneficial while others aren’t. Or perhaps they are helpful for some conditions but not others. I expect that as research continues, though, we’ll find more surprises, and may discover that many things we thought at first turn out to be wrong. But that’s how science works!
I had a fecal test that showed 2+ lactobacillus and 0 Bifido, yet 3+ klebsiella pneumoniae
It also showed low elastase (120), low butyrate, and high inflammatory factors.
Would probiotics be warranted or not and which strains should I avoid (like lactobacillus?)?
Should I take capryllic acid to kill the Klebsi (which the lab said it is sensitive to)?
How do i fix the low elastase, which indicated low pancreatic enzyme production (and any enzyme brands u recommend)?
Hey Paul,
I have been following your suggestions and I have noticed some success. I have another question for you if you don’t mind.
Do you think prebiotics can be useful against fungal infections? I have been thinking about trying a combination of inulin, FOS, lactulose, pectin and Bimuno (the brand name of a “second generation” GOS).
I am confident that my problem is with fungi, so the prebiotics won’t favour a pathogenic bacteria. The question is will they favour the probiotics or the fungi.
I intend to limit the prebiotics to about 10g total per day, as too many probiotic bacteria could also be a problem.
Thanks,
Greg.
Hi Greg,
I don’t know whether they will hurt or help.
Personally I prefer foods to prebiotics. Many foods have pectin and other fibers, but also a lot of toxins that specifically target fungi. That’s why I’ve eaten so many cranberries the last few months.
As a result of my belief that food is superior, I’ve never experimented with prebiotics.
If you want to experiment, I won’t discourage you. Let me know how it goes.
Best, Paul
It depends on the gut pathogens. Klebsiella feeds off of FOS and starch, so it is best to avoid those foods and eat foods that feed good flora, like fruits, veggies, and low-starch squash. Legumes contain resistant starch, which the good flora benefit from greatly, as this is a “food” source for good flora, but not for pathogenic bacteria. Pathogens tend to favor starches and putrefied proteins, thus a highly plant-based diet (fruits, veg, legumes, nuts/seeds, squashes) is beneficial
I find this most interesting. As a tropical agronomist I have spent all my working life (and school life) in developing countries. Have always believed that ‘squeaky clean’ was not sensible, and always clean teeth with tap or river water. Walking in Nepal way back I used river water unheated, but with 1 drop of iodine, to make up cold coffee, and milk for uncooked oats. It is only now after having a colonoscopy that I discover the problems of having one’s gut emptied! Not easy here in During my entire working life I have had a few bouts of ‘tummy bug’ often associated with eating ‘Western type food’ which I dislike over traditional food, often on streets and in remote areas of the countries where I have lived and worked.Local cures (Guava leaf tips and green coconut milk, and well cooked toast)have good for everything besides Amoebic dissentry or typhoid (the former killed by the iodine!). Hurrah for practical research, thank you.
this is a very informative article. thank you. I have been having GI issues for 30 years since a large round of antibiotics. I was wondering if the treatment for candida biofilms is different than for bacterial biofilms ? I have read that teh structure of the 2 may be different. Regareds, Suzy
Hi Suzy,
Yes, it is different. There are not many good treatments for Candida.
Candida occupies the colon, and the main strategy is to try to help probiotic bacteria overtake it in the colon and to improve immune function.
So probiotics and fermented foods, to supply bacteria; antifungal foods and spices like cranberries, coconut oil, and oregano; and immune-supporting nutrients like glucose/rice, iodine, selenium, vitamin D, magnesium, vitamin C, NAC, chromium, copper, zinc. There are various other things one can do, but I think these are the essentials.
I had lifelong fungal infections but haven’t had symptoms for a year now. Cross my fingers.
Best, Paul
Hi Paul,
Many of the suggestions you give, I am already doing and have been for quite some time. I do feel fruits and glucose raise my immediate concerns as would they not feed the candida?
I suffer from both the direct (bloating, extreme gas etc) as well as indirect symptoms (by products of candida metabolis such as fatigue and spaciness)
I am concerned that the candida not only exists in the descending colon, but also in the cecum and possibly small intestine (including the ilocecal valve)
I am wondering, in your opinion, what would you consider to be the best way to breakdown/dislodge/remove the candida biofilm that contains and sustains the candida?
I am also considering human fecal biotherapy and would like to hear your thoughts regarding using encapsulated fecal samples as a way to reach the small intestine ans direct infusion as a way to reach the colon/cecum.
Many thanks for your insights on this methodology and recommendations.
Suzy
Hi Suzy,
I do worry about fructose, so I keep fruit fairly low. Fiber will feed the gut dysbiosis. So I would avoid both.
But low-fiber glucose sources I think are helpful. For me they have been – in moderation anyway. I needed at least 200 glucose calories a day to keep my fungi under control.
Are you sure it’s Candida (only)? The only time I had a fungal infection in the small intestine / gallbladder area I had red fungal patches all over my skin. If you don’t have oral thrush and/or skin symptoms then there’s probably not Candida in your small intestine – more likely to be a bacterial infection.
They’ve found that there are some unknown bacterial infections which behave symptomatically rather like Candida but aren’t, and that these more commonly produce the small bowel problems.
The fecal infusions to the colon work well and I think are well worth trying in bowel diseases. I am not familiar with experiences with encapsulated fecal samples in the small intestine. What does your doctor say? I assume you are seeing a specialist about this?
Gut problems are always hard to figure out. I guess I would like to hear what your doctors say.
In general, fungal biofilms are best removed by bacteria and bacterial biofilms by removal of metals, polysaccharide digesting enzymes, and probiotic bacteria.
Hi Paul,
The reason(s) we feel that it is candida is that I have done the hydrogen breath challenge for SIBO and no hydrogen was in the sample. (bacteria metabolites include hydrogen) So this precluded SIBO as a diagnosis.
I produce prodigious amounts of gas and suffer from severe abdominal distention (bloating) if I ingest ANY mono saccharides, disaccharides and most polysaccharides. The expulsion of gas is violent and ongoing for up to an hour after ingestion and the gas expelled has no sulphur and appears to be mostly CO2. These manifestations lead me to believe that it must be an intestinal yeast of sorts…
Whether it is candida albicans or another type(s) is hard to ascertain without a biopsy.
The problem I see in treating this condition, which has taken ten years of my life away, is that the yeast exists in a biofilm matrix which will both, inhibit the development of a healthy gut flora and prevent anti-yeast medications from reaching the offending invader…
Encapsulating fecal matter was my idea actually as a way to get the bacteria past the acid of the stomach and into the upper GI tract.
A doctor? I think Chris Rock was right. Doctors can’t cure shit…!
I have run the gamet of natural-paths, traditional doctors and specialists to no avail. No one has been able to provide a treatment plan that worked so I am on my own on this.
Best Regards and Thanks
Suzy
Hi Suzy,
The study I mentioned was for non-hydrogen SIBO-like diseases; they found that the causal agent was bacterial unless there was also a colonic Candida infection, in which case the small bowel problem could be Candidal. I’ll look for that paper, I can’t seem to find it at the moment.
The other side of this is that there is rarely only one problem. One aspect of Candida is that it aggravates and prevents the cure of other bowel injuries or diseases. See, e.g., http://www.ncbi.nlm.nih.gov/pubmed/18622701. So you could have both bacterial infections and Candida, and the Candida might prevent the body from healing the bacterial infection.
I would avoid putting fecal matter into the small intestine. It’s normally a pretty “clean” environment and adding bacteria could easily produce an infection. It’s better to just put them in the colon and let them migrate up to the small intestine if they can flourish there.
Some of the other things I’ve found helpful are mentioned earlier in this thread, e.g. Threelac, horopito.
Re foods, you might try buying dextrose (pure glucose) and using that as your sole source of carb calories. Pure glucose is rapidly digested so that’s your best chance to nourish your body while leaving as little as possible for gut pathogens. Then I would look for plant foods with a lot of antifungal toxins but little fiber. You could try high-dose probiotic supplements, an example is http://vsl3.com. I haven’t used those.
You might want to get a blood test for candidemia/fungemia, just to see if this has gone systemic. If so you should definitely get treated with antifungal drugs. Unfortunately these tests are not very sensitive, by the time they detect the infection many patients are about 30 days from dying. Still, even if the probability of detection is low the reward for detecting a systemic infection and getting treatment is very high.
All chronic disease patients are on their own, because every disease is a bit different (different mix of pathogens, different nutritional and toxin state), and symptoms aren’t enough for diagnosis, so experimentation is necessary. I know doctors are difficult to deal with. Mine were good only for ruling possibilities out until I figured everything out and could tell them what to do – and even then it was hard to get them to prescribe the appropriate drugs. Still, if you can manage them properly they can help.
What happens when you fast (coconut oil, water, micronutrient supplements and salt/electrolytes only)? I might try long fasts, possibly adding in probiotics and Interfase (maybe Interfase Plus), and see what happens. Another thing to experiment with is charcoal – removing toxins from the digestive tract might promote healing.
Best, Paul
PS – Abdominal bloating is one of the symptoms of Candida/fungal infection of the colon … but small bowel infections are the most damaging to health and you may find fixing that first should take priority. Even if you have a severe Candida infection, the small bowel problems might be of mixed origin. Something to consider.
I’d like to share my (limited) experience with gut infections.
A few years ago, I had a GI stool test done (Diagnos-Techs Lab). It showed a +4 (out of 5) fungal infection identified as Geotrichum candidum.
I also had “abundant” overgrowths of bacteria which should have been present in trace amounts.
Per my MD’s instructions, I took an herbal supplement called ProEnt2 by Interplexus. 2 capsules, taken twice daily, taken with fatty food. I went through two bottles and then retested.
The follow-up test showed “no yeast isolated”, so that was quite an improvement over the first test!
The bacteria overgrowths improved dramatically as well, going from “abundant” to “moderate” and “rare”.
Dear Michelle,
Thank you!
I hadn’t heard of Geotrichum candidum (http://en.wikipedia.org/wiki/Geotrichum_candidum), or of ProEnt2.
ProEnt2 Plus has oregano leaf, artemesia leaf, ginger grass, and cloves. Oregano is my top antifungal herb. I’ll have to look into the activity of the others.
Perhaps Suzy should ask for that test. Sounds useful.
Hi Paul,
I would love to see that study. I did do the methane breath test as well and it was negative for SIBO. That leaves carbon dioxide and hydrogen sulfide as the remaining gases. I did a hydrogen sulfide test and it was also negative. And I did test positive for both candida and giardia in a colon swab.
Susan
Hi Suzy,
I’ll look, and do a blog post at some point. It may not be relevant to you since abdominal bloating suggests a colonic Candidal infection.
Giardia too! You are unlucky. Were you treated for it?
Hi Paul,
I do have abdominal bloating but I also have a lot of burping nad instant spaciness with carbs. If I’m reading what you are saying about the non-hydrogen SIBO type illnesses the candida could be in the small bowel too which would explain the burping. Of course it could be the giardia too.
i was treated for giardia but my symptoms did not change. I have never had classic giardia symptoms. I have heard that the cysts are in many water sourcew so I’m not sure if the cysts they foundin me indicate infection or not.
any thoughts on the use of red wine for dealing with small intestinal bacterial overgroth? wikipedia linked to a study discussing this and it caught my eye. i’ve tested postive for this, but apparently its something that tends to reoccur even after being treated.
Odd my bloating and burping started when I cut back drastically on carbs to lose weight about a year ago. I felt great while pigging out on biscotti, cheese and crackers, bread and butter, mac and cheese, etc. and washing it all down with skimmed milk.
In the fall, I started the PHD and it helped a lot, but about a month ago I cut back on fruit and nuts and started eating only in a six or seven hour window and it’s practically stopped completely now.
I feel hungry in the evenings, but I think it’s just habit and I’m learning to repress it.
Appreciate the time and letting us know about it. Keep up wonderful work. http://www.starflower.com/face-and-skin-care
paul,
i have a lengthy history of crohn’s, which is pretty mild relatively speaking, but enough to make some days interesting. just started working with a new functional medicine MD and had a stool test showing h pylori. i really don’t have any upper gi complaints, but wonder if the h pylori could be causing the inflammation in the middle to lower part of my small bowel (where the crohn’s is). my doc wants to treat with conventional abxs.
any thoughts on treating this aggressively with antibiotics vs a more natural approach (mastic gum)?
Thanks in advance.
steve
Hi Steve,
I would say first of all that Crohn’s is sort of a catch-all diagnosis for ileal / small intestinal problems that could be infectious as well as autoimmune. So it’s possible that antibiotics for H. pylori might fix your Crohn’s, even if it’s not the H. pylori specifically that is causing the Crohn’s.
It’s thought that H pylori, by suppressing mucus production, may have a role in causing Crohn’s. See http://www.ncbi.nlm.nih.gov/pubmed/21304476.
For H pylori, they’ll often they’ll do an endoscopy to see if you have ulcers in the stomach or duodenum. If so I would definitely recommend antibiotics. You might consider asking for more diagnostic steps. Endoscopy is easy and safe.
If you do go with antibiotics, be sure to take probiotics, eat fermented foods, and consider a biofilm-busting supplement like Interfase plus while you’re doing it.
I doubt the mastic gum would be effective, but no harm in giving it a try while you’re making up your mind.
Be sure to be on a good diet before starting antibiotics, otherwise pathogens may take advantage of the antibiotics to enter the body and create systemic infections.
You may have more to gain than lose by taking antibiotics, but be careful to do everything possible to stack the odds in your favor.
Best, Paul
My problem definitely seems to be in the small bowel. I had an SIBO test done and it was “borderline” and the doc gave me abx. This was a couple years ago. But that didn’t cure my bloating and gas in the small intestine (just gave me diarrhea). It seems like most people have problems with their colon. For me, it’s the small bowel mostly and I’m trying to find answers as to why. I cannot take anything with cellulase as it gives me awful bloating/pain and if I take too much (like Candex to get rid of yeast), I vomit profusely. So I know something is going on; I just have to figure out what. This is really hard. I’m just going to be strict with the PHD for awhile and then try to add some supplements.
Hey Paul,
Hope you are well. Quick question if you don’t mind. Do most of the probiotic species build biofilms as well?
I am right in thinking that the methods you propose for attacking biofilms could reduce probiotic numbers and therefore should only be used when you have a confirmed gut pathogen and not as a intermittent ‘cleansing’ gig?
Should the approach in dealing with a gut pathogen be to break down the biofilms, remove as much of the pathogen as you can and then just leave the biofilms alone.
Hi Greg,
Bacteria can live either in biofilms or in planktonic forms as free-living individuals. Commensal species usually are tolerated by the immune system and do better in the planktonic state than pathogens.
So anti-biofilm steps, carried out routinely or intermittently, are likely to help maintain a healthy gut flora.
Best, Paul
Hi Paul:
I have a nine year old daughter on the autism spectrum that has begun having bowel problems and a manifestation of motor tics. We have been eating “paleo” for about a year now and I think she may be developing sensitivities to salicylates (nuts, fruit, coconut and olive oil, nightshades, spices). I have been feeding her a diet lower in salicylates, which worked for about a week, but now her symptoms are returning. In looking around at different protocols for eliminating intestinal biofilms I found your site, and this as well:
http://autoimmunityresearch.org/transcripts/AR-Albert-VitD.pdf
in another:
http://bacteriality.com/about-the-mp/
Do you think there is any validity in the discontinuation of vit D supplementation? I supplement her with 1000IU/day per doctor’s instruction. I live in Canada and am trying to track down the InterFase. Thank you for all the great information.
Hi Louise,
You might be on to something with the salicylate sensitivity. There is some reason to believe that autism may be caused by a viral infection and salicylates may aggravate viral infections. (For instance, aspirin may have aggravated the 1918 flu epidemic, http://www.ncbi.nlm.nih.gov/pubmed/19788357.)
I think the Marshall Protocol is wrong. They are probably right that pathogens interfere with vitamin D action, but their prescription is almost certainly erroneous. Its premise is that 25OHD does not properly activate the vitamin D receptor and that Benicar, a pharmaceutical drug, does better. But there’s no evidence for this, except computer modeling by Marshall that no one but him believes. Anecdotally, people on the Marshall Protocol do poorly long-term. (So I have heard from chronic disease patients who tried it.)
Adequate activation of the vitamin D receptor is important for viral immunity.
John Cannell has claimed some successes going the other way, to extraordinarily high doses of D. I discussed that in several posts, see especially http://perfecthealthdiet.com/?p=448 and the earlier post it links to. I would suggest measuring your daughter’s 1,25D as well as 25OHD and calcium levels to see if she fits the chronic infection pattern.
The science of vitamin D in autism, and bowel trouble in autism, is at this point almost non-existent. Everything is patient experimentation at this point. Hanging out at autism parent forums and trading experiences can sometimes generate ideas. I’m sure you’ve done that.
A few ideas: Good diet and nutrition should help, just on general principles. Intermittent fasting, and either ketogenic or low-protein diets can be helpful against viral neurological diseases.
I’ll do my best to answer any questions you may have.
Best, Paul
Hi Paul,
I’ve had Crohn’s disease for almost 2 years now that won’t respond to anything besides antibiotics and steroids. My GI doc will usually only follow standard medical procedures, but he’s seen me suffer through the last 2 years of flares and has been very generous with helping me try alternatives. He has actually found me a doctor who will preform a fecal transplant on me. It sounds weird to say, but I’m honestly excited! I have Crohn’s colitis, so I’m hoping that it helps as well as I’ve read about it helping Ulcerative Colitis patients.
I have a couple questions, if you don’t mind answering.
I didn’t know about calcium and biofilms. I eat a lot of yogurt for the probiotics, especially since I’m on antibiotics. Do you recommend that I stay away from yogurt or any calcium rich food and stop taking my multi-vitamin with calcium before I have the transplant? If so, how long? I just purchased some kefir grains hoping they may help, but I’m wondering if I should hold off. Is there anything else you recommend I do in preparation for the transplant to have it best take effect? (I’m obviously going to discuss this with my doctor as well.)
Secondly, just out of curiosity, I’ve read the research that the fecal transplants helps specifically people with Ulcerative Colitis (and of course C. Diff, but I’m focusing on IBD). Do you happen to know why this doesn’t seem to be researched on Crohn’s patients? My thoughts are that possibly it’s because many Crohn’s patients have small intestine involvement, but I’m wondering if hopefully you think it will be as beneficial for Crohn’s patients who only have the colon involved.
Hi Cg,
Since the bacteria from feces come from the colon and generally don’t colonize the small intestine much, a fecal transplant is much less likely to help in Crohn’s than in ulcerative colitis. However, I think some people have begun to try it and there have been some success cases. The farther your problem is located toward the colon, the greater the likelihood of success I would think.
I would definitely minimize calcium. You should stop the multivitamin. I’m not sure about the kefir. I would keep calcium down even after the transplant, we’re not fans of supplemental calcium.
Things I would do:
1. I would get a fecal pathogen profile before and after the procedure. The “before” test may give you some idea what is causing your Crohn’s. This test looks for DNA from ~40 pathogens. An example is http://www.metametrix.com/test-menu/profiles/gastrointestinal-function/gi-effects-microbial-ecology. Comparing “before” and “after” will give you an idea how well it took. You might consider a profile of your donor before the transplant, to verify that there are no obvious pathogens. Also, based on the results you might consider some preparatory antimicrobials. For instance, if the profile shows fungal pathogens, you might take nystatin or some such anti-fungal to help clear the bowel before the procedure. (If you’re really in luck, this might clear the Crohn’s and save you the procedure!)
2. Test your serum 25OHD for vitamin D status, and make sure you get plenty of sunshine before and after. Vitamin D should be around 40 ng/ml for best gut barrier integrity.
Hope the procedure gives you a cure! Come back later and let us know how it turns out.
Best, Paul