If we were to rank popular meats by their healthfulness, the order would be (1) fish and shellfish, (2) ruminants (beef, lamb, goat), and (3) birds (duck, chicken, turkey). In last place would be pork.
Given the iconic place of bacon in the Paleo movement, it’s worth exploring the evidence against pork. George Henderson has given us a great place to start: “Nanji and Bridges identified possible problems with pork plus moderate alcohol in 1985 and other researchers have confirmed the pattern since.”
Pork Consumption and Liver Cirrhosis
Pork consumption has a strong epidemiological association with cirrhosis of the liver. Startlingly, pork may be even more strongly associated with alcoholic cirrhosis than alcohol itself!
The evidence was summarized by Francis Bridges in a recent (2009) paper [1], building on earlier work by Nanji and French [2]. A relation between pork consumption and cirrhosis of the liver is apparent across countries and has been consistently maintained for at least 40 years.
Here is the correlation between pork consumption and mortality from liver cirrhosis in 2003 [1]:
The correlation coefficient of 0.83 is extremely high – rarely seen in epidemiology. Correlation coefficients range from -1.0 to 1.0, and a coefficient of 1.0 would indicate that cirrhosis mortality was strictly proportional to pork consumption. The very low p-value confirms the statistical association.
Here is the relation between alcohol consumption and mortality from liver cirrhosis:
The correlation coefficient is lower than for pork consumption.
In epidemiological studies, beef, lamb, and pork are often grouped together as “red meat.” However, this may conceal differences between pork and the ruminant meats. Bridges found that beef actually appeared protective against cirrhosis:
In the present study using 2003 data, a significant negative association between dietary beef and rates of cirrhosis mortality was found…. [D]ietary beef may be a protective factor regarding the pathogenesis of alcoholic cirrhosis. [1]
This would be consistent with considerable evidence, discussed in our book (pp 57-58), showing that saturated fat is protective against liver disease, while polyunsaturated fat causes it. Epidemiological data confirms that saturated fat is protective; here is Bridges again [1]:
[A]nalysis of data from 17 countries indicated that diets high in cholesterol and saturated fat protected (i.e., inversely correlated) against alcoholic cirrhosis while polyunsaturated fats promoted (positively correlated) cirrhosis [8].
Beef is high in saturated fat, low in polyunsaturated fat. Pork is relatively high in polyunsaturated fat.
If the fat composition is playing a role, perhaps it is not that surprising that pork is more strongly related to cirrhosis than alcohol.
Either fructose or alcohol can react with polyunsaturated fat to produce liver disease. Sugar consumption, for example in soft drinks, may be just as likely to combine with pork to cause a cirrhotic liver as alcohol. But no other common dietary component can substitute for the role of polyunsaturated fat in causing liver disease.
Here Nanji and French summarize the correlation of pork with liver disease even in the absence of alcohol:
In countries with low alcohol consumption, no correlation was obtained between alcohol consumption and cirrhosis. However, a significant correlation was obtained between cirrhosis and pork. A similar relationship was seen in the ten Canadian provinces, where there was no correlation between cirrhosis mortality and alcohol consumption, but a significant correlation was obtained with pork. [2]
But fat composition is hardly likely to be the sole issue with pork. Most polyunsaturated fats in modern diets are derived from vegetable oils, not pork. It seems that there must be something else in pork besides polyunsaturated fat that is causing liver disease.
Pork and Liver Cancer
We would expect that if pork can cause liver cirrhosis it will also promote liver cancer, since injured and inflamed tissues are more likely to become cancerous.
Indeed, there is an association between pork consumption and the primary liver cancer, hepatocellular carcinoma. Nanji and French [3] write:
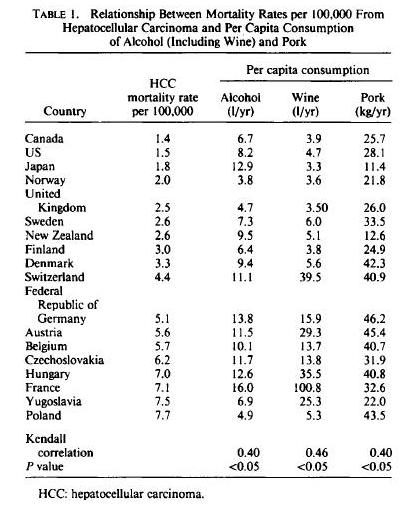
The authors investigated the possibility that dietary fat, meat, beef, and pork consumption might be factors that would, in addition to alcohol, correlate with mortality from hepatocellular carcinoma (HCC) in different countries….
The correlation between HCC and alcohol was 0.40 (p < 0.05); that with pork consumption was also 0.40 (p < 0.05). There was no correlation with total fat meat, beef, and cigarette and tobacco consumption.
Here is the raw data by country:
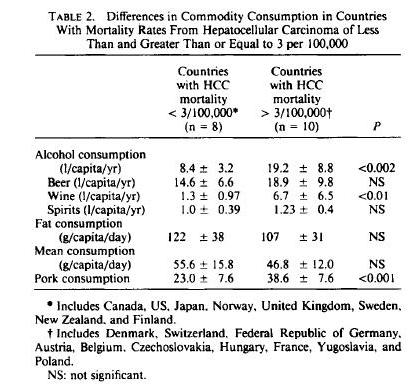
Another way of looking at the data is based on countries with low and high incidence of HCC. Countries with high incidence of HCC eat more pork and drink more alcohol, but actually eat less animal fat:
Pork and Multiple Sclerosis
Nanji and Norad [4] looked for other diseases that correlate with pork consumption, and hit upon multiple sclerosis. The connection is remarkable:
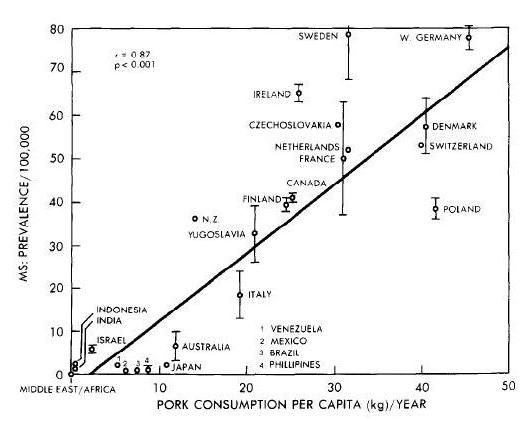
A significant correlation was obtained between prevalence of multiple sclerosis and … pork consumption (r = 0.87, p less than 0.001). There was no significant correlation with beef consumption. [4]
As noted earlier, a correlation coefficient of 0.87 is extremely high, and a p-value below 0.001 also shows a very strong relationship. MS is much more likely to befall pork eaters. Such a strong correlation makes it look like pork, or something found in pork, is the cause of MS.
Nanji and Norad further note that beef, the “other red meat,” is not associated with MS:
The correlation between pork consumption and MS prevalence was highly significant. Also, of major significance was the absence of a significant correlation between MS prevalence and beef consumption. This is consistent with the observations that MS is rare in countries where pork is forbidden by religious customs (e.g. Middle East) and has a low prevalence in countries where beef consumption far exceeds pork consumption (e.g. Brazil, Australia). [4]
The correlation between pork and MS may be seen here:
Lauer [5] verified the pork-MS link, but found it to be characteristic of processed pork:
When … quantitative data are taken into account, and a combined factor “smoked meat” or “smoked pork” is formed, the association is very high throughout. This factor is also compatible with the high risk of multiple sclerosis in Scotland and particularly in the Orkney and Shetland Islands and with the only transitorily high incidence in the Faroe Islands [6], whereas coffee can hardly explain both epidemiological features.
Arguments for the biological plausibility of some agents occurring in smoked and cured meat (in particular nitrophenol haptens and their protein conjugates) have been put forward [7]. There appears at present to be no plausibility for the factor “margarine”, which was also not compatible with the temporal pattern of multiple sclerosis in the Faroe Islands. [6]
Conclusion
There are remarkably strong correlations between pork consumption and liver disease, liver cancer, and multiple sclerosis.
What can be behind those relationships? The relatively high omega-6 fat content of pork may be a contributing factor, but it can’t be the whole story. It seems there is something else in pork that makes pork consumption risky.
What is it about pork that is so dangerous, and what does it mean for our dietary advice? That will be the topic of my next post.
Related Posts
Posts in this series:
- Pork: Did Leviticus 11:7 Have It Right?, Feb 8, 2012
- The Trouble with Pork, Part 2, Feb 15, 2012
- The Trouble With Pork, Part 3: Pathogens, Feb 22, 2012.
References
[1] Bridges FS. Relationship between dietary beef, fat, and pork and alcoholic cirrhosis. Int J Environ Res Public Health. 2009 Sep;6(9):2417-25. http://pmid.us/19826553.
[2] Nanji AA, French SW. Relationship between pork consumption and cirrhosis. Lancet. 1985 Mar 23;1(8430):681-3. http://pmid.us/2858627.
[3] Nanji AA, French SW. Hepatocellular carcinoma. Relationship to wine and pork consumption. Cancer. 1985 Dec 1;56(11):2711-2. http://pmid.us/2996744.
[4] Nanji AA, Narod S. Multiple sclerosis, latitude and dietary fat: is pork the missing link? Med Hypotheses. 1986 Jul;20(3):279-82. http://pmid.us/3638477.
[5] Lauer K. The food pattern in geographical relation to the risk of multiple sclerosis in the Mediterranean and Near East region. J Epidemiol Community Health. 1991 Sep;45(3):251-2. http://pmid.us/1757770.
[6] Lauer K. Dietary changes in relation to multiple sclerosis in the Faroe Islands: an evaluation of literary sources. Neuroepidemiology. 1989;8(4):200-6. http://pmid.us/2755551.
[7] Lauer K. Environmental nitrophenols and autoimmunity. Mol Immunol. 1990 Jul;27(7):697-8. http://pmid.us/2395440.
[8] Nanji AA, French SW. Dietary factors and alcoholic cirrhosis. Alcohol Clin Exp Res. 1986 Jun;10(3):271-3. http://pmid.us/3526949.














Recent Comments