A healthy gut is a multi-species society: it is the cooperative product of the human body with trillions of bacterial cells from a thousand or more species.
An unhealthy gut is, more often than not, the product of a breakdown in this collaboration. Often, it is triggered by displacement of cooperative, commensal species of bacteria by pathogenic bacteria, fungi, viruses, and protozoa. This is why a long course of antibiotics, killing commensal bacteria, is often the prelude to bowel ailments.
It is difficult for the immune system to defeat gut infections without the help of commensal bacteria. Think about what the immune system has to deal with. The ulcers in ulcerative colitis are essentially the equivalent of infected skin abscesses, but in the colon. Here is a description of a bowel lesion in Crohn’s disease:
Ileal lesions in Crohn’s disease (CD) patients are colonized by pathogenic adherent-invasive Escherichia coli (AIEC) able to invade and to replicate within intestinal epithelial cells. [1]
Now imagine an infected skin abscess, but with feces spread over it three times a day, or stomach acid and digestive enzymes. How quickly would you expect it to heal?
Commensal “probiotic” bacteria are like a mercenary army fighting on behalf of the digestive tract. By occupying the interior lining of the digestive tract, they deprive pathogens of a “home base” that is sheltered from immune attack. If commensal bacteria dominate the gut, the immune system can usually quickly defeat infections.
This suggests that introduction of probiotic bacteria to the gut should be therapeutic for bowel disease.
Probiotic Supplements Are Inadequate
Most supermarket probiotics contain Lactobacillus or Bifidobacterium species. These species are specialized for digesting milk; they populate the guts of infants as they start breastfeeding, and are used by the dairy industry to ferment cheeses and yogurt.
These supplements are very effective at fighting acute diarrhea from most food-borne infections. A fistful of probiotic capsules taken every hour will usually quickly supplant the pathogens and end diarrhea.
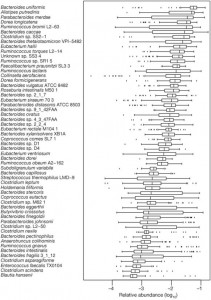
However, against more severe bowel diseases caused by chronic infections and featuring damaged intestinal mucosa, these species are usually not helpful. One issue is that they provide only a tiny part of a healthful adult microbiome. A recent study surveyed the bacterial species in the human gut, and found these species to be most abundant [2]:
As this figure shows, Bacteroides spp. are the most common commensal bacteria, with Bacteroides uniformis alone providing almost 10% of all bacterial genes in the gut. Lactobacillus and Bifidobacterium do not appear among the 57 most abundant species.
This study showed, by the way, that patients with irritable bowel syndrome have 25% fewer types of bacterial gene in their gut than healthy people, and that the composition of bacterial genes in feces clearly distinguishes ulcerative colitis, Crohn’s disease, and healthy patients. In other words, in the bowel diseases a few pathogenic species have colonized the gut and entirely denuded it of about 25% of the commensal species that normally populate the gut. This finding supports the idea that restoring those missing species might be therapeutic for IBS.
Bacterial Replacement Therapies Work
So if IBS patients are missing 25% of the thousand or so species that should populate the gut, or 250 species, and if common probiotics provide only 8 or so species and not the ones that are missing, how are the missing species to be restored?
The answer is simple but icky. Recall that half the dry weight of stool consists of bacteria. A healthy person daily provides a sample of billions of bacteria from every one of the thousand species in his gut. They are in his stool.
So a “fecal transplant” of a healthy person’s stool into the gut of another person will replenish the missing species.
Scientists have known for a long time that this was likely to be an effective therapy, but it is only now entering clinical practice. The New York Times recently made a stir by telling this story:
In 2008, Dr. Khoruts, a gastroenterologist at the University of Minnesota, took on a patient suffering from a vicious gut infection of Clostridium difficile. She was crippled by constant diarrhea, which had left her in a wheelchair wearing diapers. Dr. Khoruts treated her with an assortment of antibiotics, but nothing could stop the bacteria. His patient was wasting away, losing 60 pounds over the course of eight months. “She was just dwindling down the drain, and she probably would have died,” Dr. Khoruts said.
Dr. Khoruts decided his patient needed a transplant. But he didn’t give her a piece of someone else’s intestines, or a stomach, or any other organ. Instead, he gave her some of her husband’s bacteria.
Dr. Khoruts mixed a small sample of her husband’s stool with saline solution and delivered it into her colon. Writing in the Journal of Clinical Gastroenterology last month, Dr. Khoruts and his colleagues reported that her diarrhea vanished in a day. Her Clostridium difficile infection disappeared as well and has not returned since.
The procedure — known as bacteriotherapy or fecal transplantation — had been carried out a few times over the past few decades. But Dr. Khoruts and his colleagues were able to do something previous doctors could not: they took a genetic survey of the bacteria in her intestines before and after the transplant.
Before the transplant, they found, her gut flora was in a desperate state. “The normal bacteria just didn’t exist in her,” said Dr. Khoruts. “She was colonized by all sorts of misfits.”
Two weeks after the transplant, the scientists analyzed the microbes again. Her husband’s microbes had taken over. “That community was able to function and cure her disease in a matter of days,” said Janet Jansson, a microbial ecologist at Lawrence Berkeley National Laboratory and a co-author of the paper. “I didn’t expect it to work. The project blew me away.” [3]
Fecal transplants can be done without a doctor’s help: someone else’s stool can be swallowed or inserted in the rectum. If taking feces orally, swallow a great deal of water afterward to help wash the bacteria through the stomach and its acid barrier.
Dogs and young children sometimes swallow feces. It is unpleasant to consider, but desperate diseases call for desperate measures. Perhaps one day, healthy stools will be available in pleasant-tasting capsules, and sold on supermarket shelves. Not yet.
Attacking Pathogenic Biofilms
Most bacterial species will build fortresses for themselves, called biofilms. These are polysaccharide and protein meshworks that, like bone, become mineralized with calcium and other minerals. These mineralized meshworks are built on bodily surfaces, like the gut lining, and protect bacteria from the immune system, antibiotics, and other bacterial species.
Pathogenic species known to generate biofilms include Legionella pneumophila, S. aureus, Listeria monocytogenes, Campylobacter spp., E. coli O157:H7, Salmonella typhimurium, Vibrio cholerae, and Helicobacter pylori. [4]
Biofilms favor the species that constructed them. So, once pathogens have constructed biofilms, it is hard for commensal species to displace them.
Therapies that dissolve pathogenic biofilms can improve the likelihood of success of probiotic and fecal transplant therapies. Strategies include enzyme supplements, chelation therapies, and avoidance of biofilm-promoting minerals like calcium. Specifically:
- Polysaccharide and protease digesting enzymes. Human digestive enzymes generally do not digest biofilm polysaccharides, but bacterial enzymes that can are available as supplements. Potentially helpful enzymes include hemicellulase, cellulase, glucoamylase, chitosanase, and beta-glucanase. Non-human protease enzymes, such as nattokinase and papain, might also help. [5]
- Chelation therapy. Since biofilms collect metals, compounds that “chelate” or bind metals will tend to gather in biofilms. Some chelators – notably EDTA – are toxic to bacteria. So EDTA supplementation tends to poison the biofilm, driving bacteria out of their fortress-shelter. This prevents them from maintaining it and makes the biofilm more vulnerable to digestion by enzymes and commensal bacteria. It also tends to reduce the population of pathogenic bacteria.
- Mineral avoidance. The supply of minerals, especially calcium, iron, and magnesium, can be a rate-limiting factor in biofilm formation. Removal of calcium can cause destruction of biofilms. [6] We recommend limiting calcium intake while bowel disease is being fought, since the body can meet its own calcium needs for an extended period by pulling from the reservoir in bone. Upon recovery, bone calcium can be replenished with supplements. Iron is another mineral which promotes biofilms and might be beneficially restricted. We do not recommend restricting magnesium.
Some commercial products are available which can help implement these strategies. For instance, Klaire Labs’ InterFase (http://www.klaire.com/images/InterFase_Update_Article.pdf) is a popular enzyme supplement which helps digest biofilms, and a version containing EDTA is available (InterFase Plus).
Attacking Biofilms With Berries, Herbs, Spices, Vinegar, and Whey
Plants manufacture a rich array of anti-microbial compounds for defense against bacteria.
There is reason to believe that traditional herbs and spices, which entered the human diet during the Paleolithic and have been passed down through the generations for tens of thousands of years, were selected by our hunter-gatherer ancestors as much for their ability to promote gut health as for their taste. Dr. Art Ayers notes that:
Plants are adept at producing a wide array of chemicals with refined abilities to block bacterial functions. So when researchers sought chemicals to solve the problem of pathogens forming biofilms, it was natural to test plant extracts for inhibiting compounds. In a recent article [7], D.A. Vattem et al. added extracts from dietary berries, herbs and spices to bacterial pathogens, including the toxin producing Escherichia coli (EC) O157:H7, and checked for the ability to produce a chemical that signals the formation of a biofilm. The effective phytochemicals inhibited the bacteria from recognizing a critical density of bacteria, i.e. quorum sensing, and responding with the production of the biofilm-triggering chemical.
Blueberry, raspberry, cranberry, blackberry and strawberry extracts were effective as quorum sensing inhibitors (QSIs). Common herbs such as oregano, basil, rosemary and thyme were also effective. Turmeric, ginger and kale were also tested and found to contain QSIs. [8]
A few other remedies can weaken biofilms:
- Acetic acid in vinegar can solubilize the calcium, iron, and magnesium in biofilms, removing these minerals and weakening the biofilm; citric acid binds calcium and can disrupt biofilms. [9]
- Lactoferrin, a molecule in milk whey, binds iron and inhibits biofilm formation and growth. [10]
- N-acetylcysteine can destroy or inhibit biofilms. [11]
Conclusion
Fecal transplants are the best probiotic. Tactics to disrupt pathogenic biofilms can assist probiotics in bringing about re-colonization of the digestive tract by commensal bacteria.
Along with a non-toxic diet (discussed in Part II) and nutritional support for the immune system and gut (discussed in Part III), these steps to improve gut flora make up a natural program for recovery from bowel disease.
UPDATE: Please read the cautions by two health professionals, annie and Jesse, about potential dangers of self-treatment with fecal transplants and EDTA. It is always better to pursue these therapies with a doctor’s assistance and monitoring.
Related Posts
Other posts in this series:
- Bowel Disorders, Part I: About Gut Disease July 14, 2010
- Bowel Disease, Part II: Healing the Gut By Eliminating Food Toxins m July 19, 2010
- Bowel Disease, Part III: Healing Through Nutrition July 22, 2010
References
[1] Lapaquette P, Darfeuille-Michaud A. Abnormalities in the Handling of Intracellular Bacteria in Crohn’s Disease. J Clin Gastroenterol. 2010 Jul 7. [Epub ahead of print]. http://pmid.us/20616747.
[2] Qin J et al. A human gut microbial gene catalogue established by metagenomic sequencing. Nature. 2010 Mar 4;464(7285):59-65. http://pmid.us/20203603.
[3] Carl Zimmer, “How Microbes Defend and Define Us,” New York Times, July 12, 2010, http://www.nytimes.com/2010/07/13/science/13micro.html.
[4] Donlan RM. Biofilms: microbial life on surfaces. Emerg Infect Dis. 2002 Sep;8(9):881-90. http://pmid.us/12194761.
[5] Tets VV et al. [Impact of exogenic proteolytic enzymes on bacteria]. Antibiot Khimioter. 2004;49(12):9-13. http://pmid.us/16050494.
[6] Kierek K, Watnick PI. The Vibrio cholerae O139 O-antigen polysaccharide is essential for Ca2+-dependent biofilm development in sea water. Proc Natl Acad Sci U S A. 2003 Nov 25;100(24):14357-62. http://pmid.us/14614140. Geesey GG et al. Influence of calcium and other cations on surface adhesion of bacteria and diatoms: a review. Biofouling 2000; 15:195–205.
[7] Vattem DA et al. Dietary phytochemicals as quorum sensing inhibitors. Fitoterapia. 2007 Jun;78(4):302-10. http://pmid.us/17499938.
[8] Art Ayers, “Spices are Antimicrobial and Inhibit Biofilms,” Dec. 7, 2008, http://herbal-properties.suite101.com/article.cfm/spices_are_antimicrobial_and_inhibit_biofilms.
[9] Art Ayers, “Cure for Inflammatory Diseases,” Sept. 2, 2009, http://coolinginflammation.blogspot.com/2009/09/cure-for-inflammatory-diseases.html. Desrosiers M et al. Methods for removing bacterial biofilms: in vitro study using clinical chronic rhinosinusitis specimens. Am J Rhinol. 2007 Sep-Oct;21(5):527-32. http://pmid.us/17883887.
[10] O’May CY et al. Iron-binding compounds impair Pseudomonas aeruginosa biofilm formation, especially under anaerobic conditions. J Med Microbiol. 2009 Jun;58(Pt 6):765-73. http://pmid.us/19429753.
[11] Cammarota G et al. Biofilm demolition and antibiotic treatment to eradicate resistant Helicobacter pylori: A clinical trial. Clin Gastroenterol Hepatol. 2010 May 14. [Epub ahead of print] http://pmid.us/20478402. Zhao T, Liu Y. N-acetylcysteine inhibit biofilms produced by Pseudomonas aeruginosa. BMC Microbiol. 2010 May 12;10:140. http://pmid.us/20462423.











Hi Paul,
You have to simplify. Carbs and fiber are the most likely to give you trouble, so try rice syrup as your only carb – it will be absorbed quickly and won’t leave much food for your pathogens. Gradually introduce fermented vegetables – this will start altering your gut flora in a beneficial direction.
Eat lots of fat and moderate meat with plenty of rice syrup. Ice cream (egg yolks, cream, rice syrup) is a good food.
Supplement for nutrition. Find foods that give you minimal trouble, and work on replacing your gut flora with better bugs.
Best, Paul
Thank you so much for your reply,
You are right i have to simplify because right now it feels like i cant eat anything at all.
I have some more questions:
Right now im eating about 2400 kcal per day. How would you split the carbohydrate/protein/fat ratio in this case?
Another thing would be that my doctor said im not allowed to fast because of the Gilbert syndrome and i have to eat 5 smaller meals per day. Do you think i should do that or go for the 8 hour feeding window.
My last question would be that you wrote that i should go for heavy cream and fermented vegetables. Now the problem is that heavy cream contains lactose and fermented vegetables a lot of histamine. Do you think that i can incorporate them in my diet?
Thank you again you really gave me some hope
Hi Paul,
I think you should start without the vegetables and lactose, starve your gut bacteria for a little while, then gradually introduce yogurt and fermented vegetables in small quantities. The idea is to introduce probiotic flora to replace the bad germs. If that works, then you should be able to gradually increase quantities, and then introduce other foods.
Ok, thanks so much. I will starts straight away 🙂
Hello Paul , I got my mother with ulcerative dyspepsia T3 . Also she was surgered for polyps extraction in the gut, with succesful results.Now she follows the PHD for the major part of her diet and she seems to get great results .But she suffers from diverticular desease as well My question is if the last condition implies she can stick to these recommendations or may be must modify something else in the diet.
Thank you for your great work ¡
Christian
I must say that she was treated via an endoscopy to delete the polyps in the gut. Now the doctor expects to make her a colonoscopy to determine if there are polyps in the colon too.She was diagnosed of IBS too.She tries to avoid nuts and seeds owed her diverticulitis . She is very prudent with adding fats to the diet but after my advise based on PHD and taking her to read the book and the site she bents toward your approach .
Now with a toxin free diet she feels much better than before but maybe she needs more refinement in her diet owed to both diseases.
Thank you very much
Best , Christian
Hi Paul,
First thank you for this great webpage.
To start I’m very disappointed and obsessed by my intestinal system. I have constipation since I was born. I remember with 6 y.o. I squeeze myself to get stools out, till now. Few days ago, didn’t go to bath for 10 days, that’s the normal period for me to go to the restroom, so after 10 days I went to the toilet and squeezed myself and “shit” few lines.. and hours after I got Hemorrhoidis, which I’m treating right now with a creme. I take fiber supplements in powder and Acidophilus in capsules. No results. I think I don’t get the willing to go to the restroom at all. Constipation constantly!!!
I remember I took antibiotics once or twice in my life. I also remember that as a kid I saw very small white worms in my stools sometimes. Is that normal?
Now not anymore. I through out a lot of gases. A lot..
I don’t know if it’s the gut-flora, the diet or something else? I did a x-ray analysis with a doctor in Madrid, he didn’t mention anything relevant, except that I have a large colon than the normal.
I read a lot in this webpage. I would like to know what I Should start with gut-flor restoring? Eliminating food toxics? Anti-constipation supplements you mentioned in this webpage?
I’m also thinking to do a cayenne pepper lemon cleanse? Would that help? I have never had an intestinal cleanse before.
Thank you very much and happy new year.
Tony
Hi Tony,
Sorry to hear that you’ve had to live with this trouble so long without diagnosis or treatment.
No, it’s not normal to have worms in stool, and that does suggest a parasitic infection. It’s quite likely the infection caused your constipation and hemorrhoids.
The thing to do is to get a microbial profile of your stool. See if you can get this test done: http://www.metametrix.com/test-menu/profiles/gastrointestinal-function/gi-effects-microbial-ecology (or an equivalent).
Once you have a diagnosis of what is infecting your gut, then get appropriate antimicrobial medicines.
Also, read our post on Constipation: http://perfecthealthdiet.com/?p=2998. I think your case is going to be infectious.
I would also learn how to make fermented vegetables at home. White radishes are great. See http://perfecthealthdiet.com/?p=5165. This will provide some beneficial bacteria that might be able to outcompete your pathogens, but most likely you will need antimicrobial medicines too.
Best, Paul
Hi Paul,
I have decided to try and get the Metametrix test done. Their website has no information about patients outside the USA – do you have any idea how those of us in the EU can order one? Is it a matter of finding a sympathetic GP to simply write a letter ordering one, or does the GP need to register with them first to do so?
Hi Cb,
They have distributors in Europe: http://www.metametrix.com/international/distributors.
So I would try to find a sympathetic GP who will figure out how to order the test.
Duh me! Thanks for that, Paul, and for all the info on this thread – it’s been a mine of useful info.
Paul,
I’m reading through this series and I know you frequently recommend rice/tapioca syrup for gut dysbiosis as a source of carbs when safe starches are problematic. I was wondering if starch in the form of tapioca starch, potato flour, etc.. (baked goods) would also be a similarly viable choice for providing glucose without the accompanying fiber or are these flours equally as difficult for bacterial dysbiosis (my issue)?
Also, what is your take on the GAPS assertion that a leaky gut is unable to digest poly or dissacharides as the villi are disturbed and unable to secrete enzymes? This may sound a little silly but I’ve had two endoscopies which have both indicated that the villi are undisturbed.
Thanks for the great book and blog!
Elisa
Hi elisa,
Starches are just ground up starch, it is still in the natural molecular form that can feed gut bacteria. I would eat the natural foods, like potatoes or tapioca pearls, before I would eat the ground starches.
The advantage of the syrup is that they’ve been pre-digested down to sugars, eg oligosaccharides like maltodextrose. These are much easier for human digestion, and are typically broken down to glucose and absorbed in the small intestine, whereas a significant fraction of starch reaches the colon.
Re GAPS, certainly digestion can be impaired in gut disorders. But if you couldn’t digest at all, you would be dead. One can’t treat digestion as an all-or-nothing thing. You need to eat, and with a bowel disease you may need to find foods that you digest better, but usually the main issue is keeping foods away from pathogens rather than getting enough nourishment yourself. There is an increased need for micronutrient supplementation in bowel disorders, however.
Best, Paul
So, I got my Metametrix test results back, they showed nothing of interest (no pathogenic bacteria, yeasts/fungi or opportunistic bacteria) EXCEPT for H Pylori and an “Parasite present: taxonomy unavailable” under parasites. Dagnabbit, back to square one I guess. Argh!
This is VERY common, my husband and another friend got the same results. Parasites can mutate, thus be unidentifiable.
My husband eliminated h pylori with raw garlic. He had quite the die off reaction, however, so don’t do what he did by starting with 5 cloves at once, work up gradually. Also, h pylori infection can be a sign of low stomach acid. You could consider a trial of Betaine HCl.
For parasites we have found food-grade diatomaceous earth to be very effective. However you don’t want to take it if you have inflamnation in your gut and, again, you want to start slowly. Once you get to a therapeutic dose, you must continue for 90 days without fail because diatomaceous earth does not kill eggs. Ninety days should cover the lifecycle.
If you do not tolerate diatomaceous earth, ozonated essential oils as well as some herbal preparations that include clove and black walnut can be very effective. If you cannot tolerate any product internally, you can start by putting the oils on the soles of your feet.
Crohns boy,
I just got back the same results. Have you had any luck with treatment for the h pylori or parasite?
None, to be honest. I have been thinking of going all-out and trying the badbugs combination, but I’m understandably apprehensive. What if it doesn’t work?
I’ll be sure to report back here if I make any breakthroughs, though.
Ah ok. You don’t think the triple therapy to eradicate the h pylori would be beneficial? I’m worried it’ll worsen my gut dysbiosis.
Firstly, I don’t believe that H. pylori is much more than a proximal cause of the problem…a lot of evidence suggests that it requires pre-existing inflammation to survive, and that the ultimate cause is another bacterium/protozoan creating the inflammatory conditions necessary for it to survive.
Secondly, I take betaine HCl with each meal, and my symptoms worsen when I don’t…I imagine that the PPIs involved in the triple therapy would screw me up completely, like you said.
Hi Cb,
Well, that’s something anyway. You could experiment with an anti-parasitic medicine, see if it helps.
Hi Paul,
What timing strategy would you use with respect to taking the biofilm degrading enzymes, EDTA, and antifungal/antibacterial supplements? For example, should I take biofilms by themselves for a week or so, then cycle the EDTA (with the enzymes) for a few weeks, then attack with the antifungal/antibacterial supplements?
Cheers,
Alex
Hi Paul
I constantly get bloated with gas and my stomach will be so enlarged. i was treated for Helicobater and still didnt feel better then I went for colonoscopy en gastriscopy and the results were that I have ulcers the specialist gave treatment but Im still experiencing severe bloating
Hi Ace,
I don’t have experience with ulcers so I can’t give you advice with that. Hopefully the doctors can help. Just eat the best diet you can to help support healing and immune function. Avoiding alcohol and fructose may help.
When Shou-Ching had bloating she was helped by betaine hydrochloride, which provides stomach acid. Not sure whether that’s indicated with ulcers. You may want to try it carefully once, or consult your doctor about it.
Paul,
The link provided in your blog does not seem to work (Attached below). I would like to hear what Annie and Jessie has to say. All the best,
UPDATE: Please read the cautions by two health professionals, annie and Jesse, about potential dangers of self-treatment with fecal transplants and EDTA. It is always better to pursue these therapies with a doctor’s assistance and monitoring.
Thanks, Jacob. I’ve updated the links. Since going to pagination of comments a lot of links to comments are broken.
Dear Paul,
How would you approach the task in the case of small intenstine bacterial overgrowth (SIBO), where you can’t simply add fiber, starches and beneficial bacteria since the problem starts upstream, and you’re essentially trying to decrease the number of bacteria, albeit only in a part of the GI tract? I’ve followed the Specific carbohydrate diet with so-so results. The Metametrix test you recommended revealed that there was very little short chain fatty acids , probably a result of my long-term avoidance of fibers, and very low Bifidus levels and high Clostridium sp Some time ago you made an excellent point in a podcast with Chris Kresser: if you avoid all potential nutrients for “bad” bacteria you simoultaneosy starve the beneficial ones. So how to approach the SIBO dilemma?
Hi Lilian,
In SIBO usually potatoes and other starchy cellular foods are helpful. They will mostly be fermented in the colon, unlike simple carbohydrates.
In your case the Clostrium may be a colonic infection, so that could be why you have a starch sensitivity. Still, eating some resistant starch will help the beneficial flora and help the colon.
SIBO may require antibiotics; or simply improving stomach acid, bile flow, and digestive enzymes and eating a balanced diet may be enough. For stomach acid salt, bitter herbs, and potentially betaine hydrochloride with meals can help. For bile, cholesterol, vitamin C, and taurine.
Best, Paul
Thank you so much, Paul, I can’t tell you how much I appreciate your help with brainstorming this dilemma. I’ve tried just about everything over the past 10 years.
I do find HCl and bitters helpful. I believe hypochlorhydria and loss of migrating motor complex caused by un-and under treated low T3 (+10 years) is one of the contributing factors in my case. I am also planning to address the issue with the antibiotic protocol mentioned most frequently in studies
(haven’t found a doc yet to write the Rx).
So monosaccharides would be ok as they are rapidly absorbed, and very long chain carbohydrates would be ok because they are broken down too slowly to be utilized by SI bacteria? That is wonderful news, as I would love to find a way to add more carbohydrate without aggravating the problem. I believe my extremely low carbohydrate diet has aggravated the poor T4 to T3 conversion- a vicious cycle I’d like to escape. I take it starchy tubers would be ok then?
Warmly,
Lilian
Every bowel disease case is unique and requires experimentation, but yes, I would do my best to include some starchy tubers, and experiment to find the ones that are best tolerated.
“In SIBO usually potatoes and other starchy cellular foods are helpful. They will mostly be fermented in the colon, unlike simple carbohydrates.”
I don’t believe this is correct. Isn’t starch easily broken down in the initial phases of digestion and absorbed as glucose in the small intestine? Isn’t this how we get nutrition from it? Soluble fiber, not starch, is fermented in the colon, isn’t it?
I have not seen any of the SIBO docs say starch is helpful. I’m not sure how that would work. However, it is not generally regarded as harmful, either, precisely because it is easily broken down and absorbed and hence does not provide much fuel for overgrown bacteria in the distal small intestine.
Hi Bill,
Yes, starch is broken down quickly starting in the mouth and absorbed as glucose, but resistant starch reaches the colon and is fermented there. Potatoes are especially high in resistant starch.
Starch would not be helpful on the Standard American Diet because people already eat an excess of starch. PHD levels of starch are healthful I think. You need just enough to nourish the body and immune function, no extra.
I’m interested in an answer to Bills comment too because gaps and scd say starch is worst for sibo
please enlighten us Paul or others!
Hi Ben,
GAPS and SCD are optimized for colonic infections (IBS, ulcerative colitis) and so minimize fermentable fiber including resistant starch. They prefer simple sugars because these have no fiber.
What if someone were to use GAPS to address food sensitivities? I had Metametrix testing done, and based on results have been treated for H Pylori, parasites, and pathogenic bateria. I am waiting to retest but in the meanwhile am very frustrated with increased food sensitivities.
For almost two months, in addition to eating a PHD I eliminated nightshades, eggs, dairy incl ghee, nuts and sweet potatos. When I’ve tried a small amount of some of these items I see reactions such as back pain during the night and a face rash in the morning.
In my frustration, I’ve started GAPS intro since it is a good framework for healing the gut and slowly reintroducing foods. I’ve been eating two servings of winter squash per day in an effort to keep my carbs up But I am worried that being this low carb will encourage the wrong bacteria to grow. I have never suffered from IBS or ulcerative colitis but tend toward constipation which I manage using magnesium chelate. Any thoughts?
Thanks for all of your efforts to help others heal.
Hi Elyse,
You can always eat sugar or syrup to increase your carbs. Dextrose and rice syrup are fructose-free; you can mix with table sugar and honey to have a bit of fructose.
GAPS/SCD are relatively low in foods that trigger sensitivities, but you should take care not to be too low carb.
Our thoughts on constipation are here: http://perfecthealthdiet.com/category/disease/constipation/
Oops–I meant magnesium citrate
Hi, do you think grapefruit seed extract can be used instead of antibiotics?
It has a mild antibiotic effect. Whether it will work against any particular condition I can’t say.
Paul,
I have some kind of IBS. I have tried your PHD diet for about 9 months including fermented foods. I take two tablespoons of coconut oil every meal. The coconut oil definitely helps with reducing the IBS. Even after 9 months on PHD the IBS comes back within two days after not taking coconut oil. Is there any gut testing or bacteria testing I should do to find out if I have some kind of bacteria that needs medication? Do you have a recommended list of tests I should take?
BTW, my gut is directly connected to the pain in my lumbar discs so it is a great second indicator of something not being right.
Hi Jacob,
Well, that’s interesting. Maybe you really benefit from some ketones. Or maybe the coconut oil stimulates bile release which helps you. Or maybe something else. Biology can be complicated.
It doesn’t hurt to have a stool test and SIBO testing. Maybe they’ll turn something up. It would be nice to find something you could treat with antibiotics.
Paul,
Should I have the stool and SIBO tested when I am not taking the coconut oil so that all the bacteria show up in the test or should I test when I have things under control by using the Coconut oil?
Thanks for you patience,
I don’t think coconut oil would affect the test results.
Thank you, Paul. I will definitely have the gut tested.
Could you please clarify the following questions:
1) Is the MCT in the coconut oil killing the bad bacteria?
2) Which bacteria is being killed by the MCT and which ones survive?
3) I noticed a bit of improvement in BM when I started eating aged cheese such as Blue cheese and Roquefort cheese? Are there any beneficial bacteria in cheese or is the improvement in BM just the result of supplementing with lipase’s (from the Rennet in the Cheese)?
4) If the lack of a particular gut bacteria diversity is the cause of IBS (causing overflow of none desirable bacteria), would it not be sensible to make sure that the undesirable bacteria is suppressed with continuous use of Coconut Oil (MCT) while you are supplementing with fermented food (thus slowly building up an new bacteria balance)?
5) With reference to my question in 2) above, am I risking killing the bacteria that I am trying to introduce when taking coconut oil at the same time?
Hi Jacob,
1) It’s partially digested MCT, eg monoglycerides of medium-chain fatty acids like monolaurin, that are most toxic to microbes.
2) All microbes good and bad are damaged by it but the oils are absorbed in the small intestine which should be an antiseptic environment, so this shouldn’t be a problem.
3) Aged cheeses have vitamin K2, but smelly cheeses like blue cheese have active mold cultures. So you might have gotten some probiotic fungi.
4) Yes.
5) In general you’ll get more probiotic bacteria into your intestine if you take them apart from other foods like coconut oil. The more stomach acid and digestive enzymes you make, and the slower the stomach empties, the fewer bacteria will survive.
Paul,
I finally got tested by Metametrix. Result was high Clostridia Sp, High Mycoplasma Sp High E. Coli. High Firmicutes/Bacteroides ratio. Somewhat Low Bifidobacter sp. and Lactobacillus sp.
It also noted high levels of Propionate and low Butyrate. No inflammation, but I am infected with Pathogenic Bacteria Campylobacter sp. and Yeast Saccharomyces sp.
The test does unfortunately not specify which type of Clostridium bacteria it is.
I have travelled to Japan for business and while I was there I have found out that in Japan they use a bacteria called Clostridium Butyricum (it produces Butyrate as a waste product and can survive in acidic condition of down to pH 1.5 at very high survival rate). According to the manufacturer, http://www.miyarisan.com/english_index.htm, Clostridium Butyricum outcompetes Clostridium Acetobutylicum (which produces Propionate, butanol, ether and glycerin) Note that my level of Propionate is high.
According to the manufacturer’s information/studies the Clostridium Butyricum makes the environment more friendly to the bacteria we want in the intestine and less friendly to thrones we don’t want.
It is very likely that I also have a mild infection of C. Difficile as well. The Clostridium Butyricum supposedly also outcompetes C. Difficile, Candidas Albican and E. Coli, Klebsiella sp., Salmonella sp. and Vibrio sp.. The interesting part is that it appears that Butyrate is good for you (you cover that very well in your book) while Propionate (you only mention Propionate once in your book but in a good context) is not so good for the brain/body nor for other good bacteria. The reason I am suggesting Propionate is bad for you is that I have read about this here: http://www.psychology.uwo.ca/autism/reviewarticle2012.pdf
I presume you have already read Derrick MacFade’s, study where he can induce Autistic symptoms into rats by injecting propionate into the brain of rats, indicating that Propionate is NOT good for you)
Do you have any information about Propionate in regards to its bad effects on gut and body?
Provided the butyrate story actually works I would think that we can change the gut environment for the better by 1) supplementing with Butyrate and 2) supplementing with Clostridium Butyricum and some disaccharides (the good bacteria need some fuel)
I was wondering if you had some input here?
(I went to a Japanese doctor and showed him my Metametrix results and he prescribed the Chlostridium Butyricum for me. Now I will have to try it 🙂 ).
Hi Jacob,
It’s great that you got some insight into your condition from the Metametrix test.
Proprionate can be synthesized into glucose so it is more bacteria-friendly than butyrate.
I think your plan sounds reasonable. I am not a clinician and don’t have experience with such cases, but this sounds like a fairly minimalist, natural approach to reshaping the gut flora. I hope it works.
Hi Jacob,
Can this strain be bought in the US?
Lillian,
I don’t think so. They sell this in Japan and also in China as far as I know. I’ll update you on how it is working when I try the Clostridum Butyricum. BTW, did you Metametrix test show any other infection other than Clostridia Sp.. Ie fungi or other pathogens?
Thanks Jacob, please do keep us posted on your progress. As to your question, no other pathogens or imbalances showed up, only lack of short chain fatty acids and poor digestion.
Lilian,
What was the ratio of Butyric and Propionic acid acid in your Metametrix test? Which one was higher? My guess is that your Butyric acid level was very much lower?
Jacob,
The butyrate was 10 and Proprionate 13.
i have no idea if this is of any use, or any good, tho may be of interest.
i just did a search of iherb.com for “Clostridium butyricum”, shows up one product,
http://www.iherb.com/Advanced-Orthomolecular-Research-AOR-Advanced-Series-Probiotic-3-Natural-Probiotic-Formula-90-Veggie-Caps/43463
http://www.aorhealth.com/html/products.php?id=230
3 capsules contain,
Streptococcus faecalis T-110 45,000,000 Organisms
Clostridium butyricum TO-A 1,500,000 Organisms
Bacillus mesentericus TO-A 1,500,000 Organisms—
Thank you so much for posting this!
I looked up Streptococcus faecalis. It looks a little scary to take this. http://www.phac-aspc.gc.ca/lab-bio/res/psds-ftss/enterococcus-eng.php
The reason the japanese use the Clostridium Butyricum is due to is Butyric acid production capability (butyric acid is good for you) and the bacteria’s high acid (low pH) and high heat tolerance. I would look for bacteria strain that gives you Butyric acids. One way to make acid tolerant bacterial strains is to ferment vegetables and add raw ginger slices to the mix. It becomes really acidic and it should give you very high survivability of the bacteria when they go through the stomach. I ferment them at 30 Celcius (86F). If they are butyric acid producing bacteria I don’t know.
If your butyric acid is low I would go looking for these kinds of bacteria. Paul’s book talks a lot about the benefit of Butyric acid.
Lillian, Sorry, the Streptococcus faecalis is very common so no worries.
Sorry to keep asking all these questions.
I have noticed that I have low stomach acid. I found this out by trying to take several 1g/each HCL Betaine pills. I can take more than 5 (5g) of them and not notice any reaction in my stomach. Even 6 or 7 pills makes no difference. My concern is:
1) Why is my stomach acid pH high?
2) Would the high pH stomach acid cause the intestines to be too high pH also? Would this not effect the small intestine and cause more bacteria in the small intestine thus worsening the IBS.
A follow up on your previous answer:
If the small intestine is antiseptic, how does the bacteria from the fermented food travel to the large intestine where is needed?
Would it not be more effective to take the fermented juice and spray it up your bottom straight into your large intestine?
Hi Jacob,
Everything in the small intestine travels to the large intestine (unless it’s absorbed into the body), the body is designed to direct traffic that way.
Re your stomach acid, first I’d like to ask: are you taking these on an empty stomach? If with food are they improving digestion? You could be taking too much HCl and just not noticing any effect.
If you are producing insufficient stomach acid, there could be several causes, perhaps as simple as insufficient salt intake (common on low-carb diets) or H pylori infection. A doctor might be better able to investigate causes. Consuming bitter herbs tends to increase stomach acid.
I haven’t heard of fermented food enemas. Fermented vegetables do have nutrients that you’d like to digest, and you would lose that with an enema. It would also be uncomfortable, and potentially risky. The traditional method of taking fermented foods is orally, and I would be inclined to stick with traditional ways.
Butyrate 10 and Proprionate 13, so both very low.
RE Reply to Paul, point 5
I believe you meant to say ..” the faster..” not “slower”
Hi Morris,
No, I meant slower stomach emptying exposes bacteria to stomach acid longer, killing more of them.
I think I asked my question incorrectly : My question should be : How can the small intestine be antiseptic if bacteria from fermented food is able to travel though the small intestine without depositing bacteria thus making the small intestine NOT antiseptic?
With regards to the HCL Betaine pills. I have tried to take them before food, during food and after food in various amounts. No effect on digestion and no stomach burning . I do eat a lot of salt.
I absolutely agree with you in regards to the enemas javascript:grin(‘:grin:’)
I wonder if anyone has ever analyzed the bacteria in various fermented food and compared these bacteria with the bacteria you find in a healthy person?
Hi Jacob,
Well, it’s not completely antiseptic, but compared to the large intestine, the density of microbes is something like a thousand times smaller. Microbes traverse the small intestine; they stay in the large intestine.
One of the reasons we try to ferment vegetables in a sealed, anaerobic, salty, acidic environment is to promote growth of microbes that are appropriate for our gut and death of microbes that don’t belong there. Yes, the bacteria in fermented foods have been analyzed, they’re usually most like the bacteria in our guts if you use low-sugar vegetables, salty brine, low oxygen, and about two-three weeks of fermenting.
Paul,
Do you have any references of studies that has been made for the species of bacteroidetes and Firmicutes we can expect to find in various fermented food?
Hi Jacob,
I looked up a bunch of studies when I did our fermented mixed vegetables posts, you might check those posts to see if they were cited there.
Paul,
I have trawled through your blog and every time I look through I find something new. Anyways, I found something about FODMAPS and I tried eliminating these. This seems to be quite successful for me. I would naturally like to restore the bacteria that can digest the FODMAPS. Would it not make sense to try to specifically ferment the FODMAPS for the purpose of reintroducing these bacteria to the Colon?
Hi Jacob,
Yes, I think that’s a sensible thing to do — make fermented mixed vegetables using FODMAP-containing vegetables.
However, a possible reason for FODMAP sensitivity is SIBO — overgrowth in the small intestine of bacteria that are good at digesting FODMAPs. If this is the problem you may need more stomach acid — try supplementing betaine HCl with meals and see if that helps. It may also help to gain more bacteria of other kinds in the colon — try eating more resistant starch (potatoes) for that.
Paul,
I have concluded that (one of the problems) I have is SIBO. I presume that I should eat more resistant starches because the resistant starches don’t feed the bacteria in the small intestine and instead gets broken down in the Colon? What are other resistant starches I can eat?
My stomach acid is now working again after I cut out FODMAPS and supplements with aged cheese. I have also stopped taking two table spoons of coconut oil at every meal. Now I just use coconut oil mixed with palm oil for cooking.
I also suspect that the aged cheese I started eating provides competing bacteria to the colon that tries to outcompete the FODMAP eating bacteria. There must be a feedback loop somewhere because now my stomach acid seems to work well. It wouldn’t surprise me if the bacteria was so clever that they figured out a way to modulate the stomach acid the body released to ensure their own survival.
Another very interesting point is that (after I cut out FODMAPS and getting some control over the SIBO) I have now started taking Vitamin K1/K2 and I feel a huge difference in my lumbar. I suspect the SIBO has hindered the absorption of Vitamin K and has caused the disk problem in my lumbar. From research Vitamin K is very important for bone and tissues. Your book (which I have read three times) touches on this as well. At first I thought it was the lipase in the aged cheese that helped me absorb the oil in the food. To test this theory I cut out the aged cheese for 5 days and took just the Vitamin K. Still I see improvement every day. If I stop the Vitamin K the lumbar problem gets worse.
What else can I do to get rid of the SIBO for good?
Thanks for all the super advise and I look forward to hearing back on all my questions.
Hi Jacob,
Very interesting that the aged cheese fixed things for you. Vitamin K2 is so important, that is one of my favorite supplements.
It could be also that you needed more bile to absorb the fat-soluble vitamins. Be sure to get extra vitamin D and A, you may be deficient in those as well as K2.
I’m not sure what else you can do for the SIBO – since you’re making real progress you probably don’t want to go the medical route. I would just continue trying to be healthy and well nourished and to gradually diversify the diet. Also, to support immunity circadian rhythm and other tactics are helpful; these are discussed in the new edition.
Best, Paul
Hi Paul
I see where I misunderstood your point, I thought you meant the entire digestive tract. Slow transit time in the intestines favors bacterial proliferation. Sorry
Paul et al,
speaking of pathogens, are there any steps you or anyone else is familiar with to overcome symptoms caused by a predominance (per Metametrix test) of Clostridium sp. (not C. diff., though)? I have tried all the usual steps for years; probiotics, diet etc, but that seems to actually make matters worse, not better. I have tried several rounds of Xifaxan and recently Xifaxan + Neomycin, but to no avail. Because of the symptoms, I have to avoid fiber (fruits, vegetables) almost completely, and this worries me, in addition to endotoxins being produced etc. The only antibiotic I know of that is specifically used for Clostridium sp. bacteria is Vancomycin, but that is a bit cost-prohibitive at the moment ($2000). Any other avenues that might help correct the imbalance?
As a sidenote, I have been on a very low-carb primal/paleo diet informed by the SCD, and adding non-fibrous starches (rice, Udi’s white bread) as per your suggestions has had a tremendous effect on my energy levels, so thank you for that part of the PHD, too! You’re making a wonderful difference on the lives of so many people!
Warmly,
Lilian
Hi Lilian,
Thanks, I’m glad PHD has helped you!
Unfortunately not being a clinician I’m not that knowledgeable about how to address specific difficult cases. I don’t know what would work best for your Clostridium dysbiosis. I would probably stick with diet and fermented vegetables and circadian rhythm therapies, and consider antibiotics and fecal transplant if necessary.
FYI: Udi’s White Bread has brown rice flour and the third ingredient
I had my doctor take my vitamin d levels and they were too low. Last winter I tried taking cod liver oil but after a couple weeks I started to get really clumsy and would feel really odd after taking it. I assumed that its a vitamin a overdose or something, since I usually don’t do well with taking man made vitamins, I tend to get bad side effects. This fall I ordered the fermented cod liver oil, having read that it has its natural vitamins in it. I felt amazing the first few days, then yesterday again the clumsiness, I tripped several times and just felt uncoordinated. What could be causing this? And what should I do now that winters just about here? I get really depressed in the winter.
Hi Alex,
We’ve posted on the possibility that DHA plus vitamin A plus oxidative stress will create highly toxic compounds (see http://perfecthealthdiet.com/2011/05/dha-and-angiogenesis-the-bottom-line/ and earlier posts). So cod liver oil, fresh or fermented, is not entirely risk free.
That said, I don’t know what’s causing your symptoms. It sounds like a toxicity effect but I don’t know why the cod liver oil would lead to an endotoxemia or other severe toxicity syndrome.
The other possibility is as you guessed a vitamin A overdose. Vitamins A and D need to be in balance so with D levels low you really don’t want to supplement A. I would avoid cod liver oil until you get D levels up.
Hi this article is very interesting.
I have a theory that I am kind of researching which led me down the track on healthy gut bacteria.
Could one achieve healthy bacteria by consuming a diet of green leathy vegetables, and fruit, with some oils for fats. No meat and no diary?
Here is what I am thinking. Vegetables can supply all required amino acids, including those used by cells to build proteins, since break down of dense protein into amino acid puts a load on the gut, and really what you want is the basic aminos anyway. and this should support healthy bateria and help kill some of the bad.
Use fruit to provide simple carbs which provides body fuel, some fibre, not too much, and reduces load on system so not having to convert complex carbs into simple carbs ( which body has to do otherwise ) which in turn again reduces load on gut.
Use oils for essential fatty acids.
Then elimiate meat because of the heavy load on gut,
Same with milk.
Elimiate temporily ( 3 months ) all grains, seeds, legumes so that gut has chance to biuld up suficient amounts of mucins which will bind onto the lectins from these foods. Once the gut is healthy and producing good amounts of mucins then these kinds of foods can be re-introduced ( of course as long as person chews food thoroughly to produce adequate saliva and stimulates proper digestion ).
With a healthy gut, all the Hype of Lectins breaking gut wall should be null, considering these foods are actually a good source of easily avaliable carbs, protein and minerals.
Then meat could be introduced back into diet, but only very sparingly.
What do you think of this as a method of gut flora repair through selective food type reduction?
Hi Nigel,
Ingredients for a healthy gut are:
– Good fiber — that means primarily resistant starch and soluble fiber
– The optimal balance of nutrition to promote immune function and wound healing and avert endotoxemia
I think our diet provides that. Evidence in the book.
i just found an interesting post (to me),
it covers digestive problems.
The bit that resonated to me was the zinc deficiency & low stomach acid topics.
It had a part that read,
“One of the causes of hypochlorhydria is zinc deficiency.
Interestingly the last 5 signs of hypochlorhydria (from list in article) are also associated with low zinc levels.
Zinc deficiency is incredibly high in some countries i.e. in Australia around 75% of people are zinc deficient.
A zinc tally test may help you determine if you have a zinc deficiency.
Also white spots on the nails would indicate a zinc problem also.”
& the ‘last 5 signs’ mentioned from the list is,
– Itching around the rectum
– History of food allergies
– Iron deficiency
– Post adolescent acne
– Dilated capillaries on the face (rosacea)
here’s the link,
http://bodymindsoulhealth.com.au/blog/2010/08/are-you-embarrassed-by-belching-burping-or-bloating/
hope it is of interest/help to someone
Dear Paul,
How would you interpret and address intolerance of (due to great abdominal distention) of fermented foods, including their juices, and probiotic supplements? For background, there is, according to Metametrix, an predominance of Clstridium sp.
Best,
Lilian
Hi Lilian,
Well, I’m guessing, but since probiotics do it it could be that adding bacteria sets off a little bacterial warfare that leads to an influx of inflammatory bacterial cell wall components through a leaky gut.
Another possibility is that toxic/inflammatory amines, like histamine, generated during fermentation cause the trouble.
A third is that lactic acid triggers it and the ferments and their juice are lactic acid rich; Lactobacillus probiotics will generate some lactic acid.
Thank you, Paul!
Do you think there’s any way to overcome/circumvent this and achieve gut health and balance ?
Yes, but I’m not sure what the best strategy is. You may want to minimize supplementation, so that you don’t overnourish gut microbes and help them build biofilms; but eat liver and optimize vitamin D to promote gut immunity. Eat a variety of vegetables and starches in PHD proportions. Eat small amounts of fermented vegetables — hoping to gradually alter the microbial ecology.
If the Clostridium overgrowth persists you could try antibiotics or anti-biofilm tactics along with fermented foods and probiotics to try to change the microbes more aggressively.
Thanks a bunch, Paul. I so appreciate your input
D is optimized, liver is on the menu and I have tried many antibiotics, including very potent ones specifically chosen to be active against clostridia. Hvent retested post- tx, but symptoms are the same so I assume no change occurred.
By decreasing supplementation do you mean any and all supplementation? Would ionic minerals be ok, based on the Assumption that they will most likely be absorbed prior to reaching the large intestine?
Most importantly, do you think persisting with fermented vegetables despite the reaction might eventually lead to the reaction to go away, so that it in the long run might lead to normalization I got for?
Dear Paul,
I have read your book and think it is amazing! I constantly refer to it whenever I need to. I am a 22yo male and seem to get allot of gas and slight bloating every time I eat resistant starch of any kind – I suspect this is from a problematic large bowel. If I avoid resistant starch for a couple days(stick to warm jasmine rice instead of potatoes) I get constipation, so I’m forced to introduce resistant starch back into my diet. I’m not quite sure how to fix this, I suspect the constipation is from the lack of bacteria in the large bowel as a result of the reduction in resistant starch.
In addition to this lingering problem I went on large binge of fruit juice this time last year when I had no knowledge about health and nutrition(I actually thought it was healthy at the time… damn media). Ever since I have formed red patches on my skin primarily my face, doctors call it ‘dermatitis’. I have tried to avoid fructose altogether successfully but now it hangs around constantly and has worsened. It’s come to the point that I’m questioning whether tomatoe’s may be triggering a reaction due to the small fructose content.
Anti-fungals cause severe eczema across my entire face which I never had before in my life, so you can imagine why I wouldn’t want to blast my small intestine with anti-fungals. The eczema takes around 1 month to heal.
What I’m Doing about it now:
-Follow your macronutrient ratios carefully and feel great, I was eating too much protein before whilst following the paleo diet.
-Supplement Iodine 1-3mg per day, Magnesium 200mg/day, Vit C 1g/day, Vitamin D3 5000IU/day, just started Life extension vitamin k2.
-Eat Liver 1-2 times per week
-Eat Fish 3 times per week minimum
-My fats come from Butter, Ghee, Animal Fats, 3 Yolks/day, Macadamia Nut Oil(Not often)
-Resistance Train 3 times per week and am putting on a nice amount of lean muscle, thus my strength is increasing consistently. I have allways been a very lean “hardgainer” but your diet reigns supreme amongst all the diets I have been on to gain weight.
-My sleep is great, 8 hours per night and live a stress free life
-Made my first fermented cabbage, only a couple more days to go!
-I have taken Bio-Kult probiotics before and experienced nothing but a lighter wallet.
I consume Thyme, Chive, Turmeric, Basil, Corriander, and the occasional ginger and lemon tea on a daily basis. No die off effects so far. As you can imagine my skin is affected, so I am very motivated and disciplined.
I apologise for the long post but I figured the more details I include the better!
Best Regards
Alex.
Alex,
I think you are showing symptoms if Small Intestinal Bacterial Overgrowth. SIBO. All the “perfect health” in the world will not fix that. I have tried. You need to look up Allison Siebecker at http://www.siboinfo.com I would advise to buy her presentation etc. you should also look up dr Pimmental whom is also a specialist at this. Another important clue is FODMAP which is an iPhone app you must buy.
After doing that you should look up SCD diet. Finally you must try to find out root cause. Try somebody that practices functional medicine or similar. I would start with Cyrexlabs Panel #3
Good luck.
Hi, I was astonished to read that there are tens of different probiotic bacteria in the gut. Last year, the doctor diagnosed me with Irritable Bowel Syndrome, gave me a note with Lacto & Bifudum probiotic supplement brands and went his merry way.
I had some embarrassing symptoms which started in the summer, early autumn of 2012. My stomach started to make growling noises and sloshing sounds even though I was not hungry. I also felt pain on my left side which went away after a gas relief or bowel movement, but happened to return hours later.
The weird thing is that I did the necessary tests(bacteria, parasite, ova, celiac), but the doctor told me they were all Negative. I also did an ultrasound to see if there were foreign objects and the report came in the mail saying there is no significant concern or something like that…
The surprising thing is, the Lacto probiotic supplement helped me a little and reduced my bloated stomach..I thought I was gaining weight in that summer.
I started using more garlic, lemon juice and pepper, and I also use peppermint tea and oil capsule….and those have worked moderately well to reduce those stomach growls.
It hurts when you know something is in there making all those noises, but the doctors can’t find out what it is. I hope in the near future doctors can figure out the causes of IBS, Chrons, etc. because a lot of North American people are suffering these ailments.
Riaz,
There is a solution for IBS. SIBO is the major cause of IBS you will find a lot of studies about this. See my note right before your entry.
(I also had IBS)
Hi Paul,
As an anti-biofilm tactic in combination with antimicrobial treatment to clear SIBO and heavy Candida overgrowth prior to fecal transplantation, how many times would you recommend EDTA chelation if administered 1x per week?
Thank you so much for your sharing your incredible knowledge with the world.
Warmly,
Lisa
Would ionic forms of minerals be a better choice in terms of providing minerals for th body but not for the formation of biofilms (assuming they old be absorbed quickly and high up in the GI tract, and presumably never reach the lower small intestine or the colon)?
Hi Paul,
Thank you for all the work that you do. I found a private clinic in the UK that does fecal transplants and I have a consultation with them soon. What should I ask to determine that their procedure is safe and effective?
Hi Paul, I have read your book. Inwas set up to do a fecal transplant and so I read your book first to see how I should eat after. I have had leaky gut and SIBO for 4 years. I got it at 22 and now am 26. I preformed a nj tube fecal transplant and also by enema today. I figured if it works for crohns and croft and uc then why not SIBO if you kill all the bad guys first. I should have had meta matrix testing done first but I didnt. I went on flagyl, rifaximin,and vanco plus an anti fungal and anti parasitic. The doctor I am seeing prescribed my betaine plus to help with the break down of food. Will that interfere with the good bacteria I just placed? Also I was on all of those antibiotics for 14 days and I got a white tongue but most of all I began to get nerve pain. The docs said to stay on it and it would go away. I don’t drink any alcohol so I thought the pains were weird. The. Ftwent well burpt I have peripheral neuropathy going on. They placed me on b12 shots sub q and I am doing pt. I have been off the flagyl for four days…have you heard of this happening. I should have done neomycin instead.. I am freaking out that it won’t go away and I am a professional climber. Any help would be greatly needed!
Hi Portia,
It sounds like you have a fungal infection, maybe other infections too, and the antibiotics killed bacteria allowing the fungi to overgrow creating the oral thrush, and probably similar overgrowths elsewhere.
Ending antibiotics, receiving the fecal transplant, and now eating probiotics and kimchi, should help. Also eat plenty of vegetables which are anti-fungal.
The neuropathy is harder to explain but the simplest explanation would be circulating fungal toxins, eg cell wall components. You might try a low dose of activated charcoal to help excrete toxins, plus glutathione/NAC for liver support.
Betaine shouldn’t interfere with your good bacteria but if you take too much it can inflame your stomach or gut lining.
I think the Metametrix test is a good idea when things settle down.
Also since having leaky gut ihave taken tons of probiotics from natren and others. It makes my stomach hurt more and increase in bloating, so i figured fecal transplant is the way. I have eaten only beef and cabbage for three years because anything I eat including vegetables and fruit and non grass fed meat triggers my immune system and I get swelling and gain thirty pounds in three days and get a rash and joint pain…my LFTs were also elevated due to my liver trying to get rid of the antibodies built. I have the hardest time eating foods. I react to everything I feel like so I thought the ft would help introduced the good bacteria to break down sugars. I am so worried about the nerve pain
Hi Portia,
Hmmm. If so many foods cause problems, I think you need diagnostic testing for your gut. The problem sounds severe enough that doctors should be able to detect something.
I think for serious problems like this you should connect with someone that specializes in MTHFR (or genetic Single Nucleotide Polymorphism, or SNPs).
Contact one of the doctors on http://www.mthfrsupport.com. They can help difficult cases like this. B12 issues are typical for people with MTHFR problems. However, if you don’t know your SNPs you can really screw your self up taking the wrong supplements and/or eating Paleo. Take the http://www.23andme.com test and translate the raw data on http://www.mthfrsupport.com BTW, cabbage and beef are both high in sulfur and if you have a CBS SNP mutation you are never going to heal until you go on a low sulfur diet. However, you don’t know your SNPs so you are just guessing. You can look up Ben Lynch and Amy Yasko’s work if this is of interest to you.
One thing I’d like to point out is that this woman got the c. Dif. Infection from taking antibiotics. Many of us with chronic infections whether they manifest as bowel disorders or other types got sick partially from antibiotic use. I would greatly encourage people to learn about and use natural antimicrobials which don’t cause resistant bacteria because of their complexity. Berberine and berberine containing herbs were what finally healed my colitis. I have had good results with oil of oregano and olive leaf as well, but the most effective for bowel problems and diarrhea is berberine, golden seal, coptis, barberry, etc. Turmeric is highly anti inflammatory as well as antimicrobial and very helpful. High dose natural vitamin e is very effective for eliminating pain during inflammatory flares. 1200 -1600 units stops pain in minutes. Only use this much for a few days then stick with the amount in a multivitamin 200-400 units.