So I thought I’d finish up the series on DHA and angiogenesis by discussing 2 issues:
1. First, an assertion: The pathway by which oxidized DHA drives angiogenesis may be really important for human health.
2. Second, the $64,000 question: Is there evidence that high levels of dietary DHA promotes diseases of pathological angiogenesis? What about other dietary factors bearing on DHA oxidation?
Significance of the Oxidized DHA Link to Angiogenesis
The papers discussed in Friday’s post about a major angiogenesis pathway stimulated by oxidized DHA (Omega-3s, Angiogenesis and Cancer: Part II, April 29, 2011) may not seem important to many readers. But to cancer researchers and pharmaceutical companies, this is blockbuster work.
A tumor is, in the words of Hal Dvorak, “a wound that never heals.” [1] To support growth, cancers invoke the wound healing process – especially, creation of new blood vessels, or angiogenesis. But the tumor prevents the wound healing process from completing. If it ever did complete, then the tumor itself would be healed. It would cease to grow and become benign.
It’s been recognized for decades that an ability to block angiogenesis would effectively constitute a cure for cancer. The William Li video explains why: nearly everyone gets microscopic tumors that never develop the ability to induce angiogenesis. Life-threatening cancer is the result of tumors that can induce angiogenesis. No angiogenesis, and no one would die of cancer.
But existing anti-angiogenic cancer therapies have produced disappointing results. Avastin, an anti-angiogenic drug targeting VEGF (vascular endothelial growth factor), has been estimated to extend colon cancer patient lifespan by only 6 weeks. (Nevertheless, Avastin generated $7.3 billion in revenue last year. Imagine how much money there would be in an anti-angiogenic therapy that worked!)
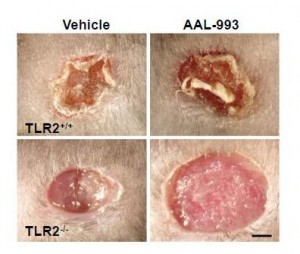
The work I discussed last Friday suggests a reason for that failure. Recall these pictures:
If only the VEGF pathway is blocked (upper right), there is almost as much angiogenesis and wound healing as in a normal wound (upper left). But when both the VEGF and TLR-2 angiogenic pathways are blocked (lower right), there is no wound healing.
If these are the operative pathways in cancer also, then blocking the TLR-2 angiogenesis pathway might be the key to cancer therapy.
But cancer is not the only disease of pathological angiogenesis. Others include:
- Age-related macular degeneration, diabetic retinopathy, and retinopathy of prematurity – three common causes of blindness.
- Atherosclerosis, which often features angiogenic vessels in thickened arterial walls.
- Vascular malformations and tumors.
- Obesity. Adipose tissue utilizes angiogenic pathways, and angiogenesis inhibition prevents the deposition of fat.
- Rosacea, psoriasis, and some other skin conditions.
- Endometriosis, uterine fibroids, and some other causes of female infertility.
- Rheumatoid arthritis.
- Crohn’s disease.
- Preeclampsia.
It may be that the TLR-2 pathway is key to these diseases as well, and that a treatment that inhibits this pathway can cure or improve all of these diseases.
Add up the size of these markets and a pharmaceutical company executive would swoon.
Luckily, we’re not pharmaceutical company executives. But we can still get excited over possibilities to improve these diseases through diet and anti-microbial medicine.
Infections as Contributing Causes of These Diseases
TLR-2 is stimulated by other things besides oxidized DHA. In particular, TLR-2 is an immune molecule which is stimulated by pathogen proteins. As Wikipedia notes:
TLR-2 recognizes many bacterial, fungal, viral, and certain endogenous substances.
This tells us that many pathogens may stimulate angiogenesis through the TLR-2 pathway. As a result, anti-microbial medicines might help treat some diseases of pathological angiogenesis.
Some antibiotics, including doxycycline and minocycline, are known to exercise anti-angiogenic effects independent of the antibiotic effects. [2]
Diet-Induced Angiogenesis
Many foods affect angiogenesis. In fact, cancer studies have identified dozens of plant foods, from garlic to tomatoes to leeks, that possess anti-angiogenic properties.
However, foods can also promote angiogenesis. Let’s stick to the oxidized DHA pathway and see if there’s evidence that foods drive it.
You’ll recall the recipe was:
If this pathway is important in human disease, then we should expect diseases of angiogenesis to be worsened by adding the ingredients on the left.
Specifically, cancer, AMD, rosacea, and so forth should be worsened by high doses of DHA, high doses of vitamin A, and low doses of antioxidant minerals like zinc or selenium.
Is there any evidence for that pattern?
Cancer Studies
First, let me give my bottom line on the Brasky study that kicked off this series. High tissue levels of DHA were associated with increased risk of high-grade prostate cancer, and the oxidized DHA angiogenesis pathway provides a mechanism for this association. What’s not clear is why tissue DHA levels were high. EPA levels were also elevated in the high-grade prostate cancers, but not by nearly as much as DHA levels. EPA and DHA appear together in fish and fish oil, so this suggests that fish consumption contributed to but was not the primary cause of the elevated tissue DHA. The drug finasteride greatly raised risk of high-grade prostate cancer, but the paper did not break down the DHA-cancer association between the finasteride and placebo arms. The most likely explanation, in my view, is that finasteride increases conversion of EPA to DHA and creates artificially high tissue DHA levels. The high DHA levels combined with oxidative stress drive cancer through the TLR-2 angiogenesis pathway.
A clever but unlikely alternative explanation was suggested by Peter at Hyperlipid: perhaps extra dietary fish oil raises testosterone levels. Prostate cancer is a hormone-dependent cancer and can be promoted by testosterone, just as breast cancer is promoted by estrogen. Possible supporting evidence comes from a paper showing an inverse association between metabolic syndrome / diabetes and prostate cancer. The trouble with this idea is that (a) this effect should have been strongest in the low-grade cancers, since diabetes reduced the incidence of low-grade cancers, but in the Brasky study DHA had no association with low-grade cancers, (b) fish oil lowers testosterone levels in rats, (c) in the Brasky study high-grade prostate cancers were strongly associated with obesity and the obese generally have low testosterone levels, and (d) surprisingly, high-grade prostate cancers are associated with low testosterone, not high. So one could argue that fish oil might promote high-grade prostate cancer by lowering testosterone!
A unified explanation along this line would be: Finasteride raises DHA levels, and DHA lowers testosterone. Low testosterone reduces incidence of low-grade prostate cancers but makes it much more likely they will progress to high-grade. Thus, finasteride reduces prostate cancer incidence but increases high-grade prostate cancer incidence and overall prostate cancer mortality. Fits all the facts. Could be.
My bottom line: the Brasky study is weak evidence for anything, but it does raise a whiff of evidence that high dietary fish oil intake might encourage a transition from low-grade to high-grade cancer.
What about other ingredients in the recipe? Does increasing retinyl levels raise cancer risk?
Retinyl palmitate (vitamin A) has been tested in clinical trials for its effect on cancer risk. The trials had to be cut short when it was found that vitamin A increased cancer mortality:
The Carotene and Retinol Efficacy Trial (CARET) was a multicenter randomized, double-blind placebo-controlled chemoprevention trial testing whether daily supplementation with 30 mg β-carotene + 25,000 IU retinyl palmitate would reduce lung cancer risk among 18,314 heavy smokers, former heavy smokers and asbestos-exposed workers. The intervention ended 21 months early in January, 1996 when interim analysis found evidence that the supplements increased the risk of lung cancer and total mortality in this high-risk population by 28% and 17%, respectively (10). [3]
After the study ended participants were tracked for years afterward. Those who had received vitamin A during the trial, but especially those in the vitamin A arm who took additional supplements (mainly multivitamins which are rich in A, but possibly also fish oil), had more high-grade prostate cancers:
As a proportion of the total prostate cancer cases, more men who were randomized to the active arm developed high-grade prostate cancer (Gleason 7-10) than in the placebo arm (44.6% vs. 40.1%, respectively)….
For aggressive prostate cancer, men in the CARET intervention arm who used additional supplements had a relative risk for aggressive prostate cancer (Gleason >or=7 or stage III/IV) of 1.52 (95% CI, 1.03-2.24; P < 0.05), relative to all others. [3]
Interestingly, in the placebo arm taking multivitamins and other supplements reduced cancer risk.
Other studies have found similar results.
Men with higher retinol concentrations at baseline were more likely to develop prostate cancer (quintile 5 vs. quintile 1 hazard ratio = 1.19, 95% confidence interval: 1.03, 1.36; P(trend) = 0.009). The results were similar for aggressive disease. Joint categorization based on baseline and 3-year retinol levels showed that men who were in the highest quintile at both time points had the greatest increased risk (baseline/3-year quintile 5/quintile 5 vs. quintile 1/quintile 1 hazard ratio = 1.31, 95% confidence interval: 1.08, 1.59). In this largest study to date of vitamin A status and subsequent risk of prostate cancer, higher serum retinol was associated with elevated risk, with sustained high exposure conferring the greatest risk. [4]
Carotenoids, which can generally be converted to vitamin A, are also associated with higher cancer risk. There is one exception – lycopene:
Lycopene was inversely associated with prostate cancer risk (comparing highest with lowest quartiles, odds ratio (OR) = 0.65, 95% confidence interval (CI): 0.36, 1.15; test for trend, p = 0.09), particularly for aggressive disease (comparing extreme quartiles, OR = 0.37, 95% CI: 0.15, 0.94; test for trend, p = 0.04). Other carotenoids were positively associated with risk. [5]
What’s special about lycopene? Wikipedia explains:
Lycopene may be the most powerful carotenoid quencher of singlet oxygen,[18] being 100 times more efficient in test tube studies of singlet-oxygen quenching action than vitamin E … The absence of the beta-ionone ring structure for lycopene increases its antioxidant action….
Lycopene is not modified to vitamin A in the body …
So lycopene does not increase retinyl levels, but does act as an extraordinarily powerful antioxidant, thus reducing oxidative stress! If you wanted a good food for stopping the DHA – angiogenesis pathway, you’ve found it: tomatoes.
Hmmm, tomatoes go well with salmon …
That gets us to the third part of the recipe, oxidative stress. If oxidized DHA drives angiogenesis, then antioxidants should be preventative for these diseases.
The evidence here is rather mixed, because with the exception of the negative effects of vitamin A, most antioxidants seem to have little effect on cancer. Nevertheless, I’ll give some studies. Selenium is a antioxidant mineral due to its role in glutathione peroxidase:
Serum selenium was inversely associated with risk of prostate cancer (comparing highest to lowest quartiles, OR = 0.71, 95% CI 0.39-1.28; p for trend = 0.11), with similar patterns seen in both blacks and whites. [6]
Zinc is an antioxidant due to its role in zinc-copper superoxide dismutase. Prostate cancer is associated with low tissue levels of zinc. [7, 8] High dietary intake of zinc is associated with lower rates of prostate cancer. [9]
N-acetylcysteine is an antioxidant supplement that is a precursor to glutathione. N-acetylcysteine has been shown to prevent angiogenesis and has been proposed as a likely cancer preventative, but this is as yet untested. [10]
Other Diseases of Angiogenesis
I’ll skip those for now, other than to note that fish oil is a well-known trigger of rosacea. Is it possible that the mechanism is via TLR-2 activation by oxidized DHA?
Conclusion
At the moment there’s some puffs of smoke but no fire. Observational studies weakly link high DHA, high vitamin A, and low antioxidant status to diseases of angiogenesis such as cancer.
This pattern would be consistent with the idea that the natural pathway used in wound healing to trigger angiogenesis – DHA oxidation and combination with retinyl protein to trigger TLR-2 pathways – is also important for cancer progression.
It suggests a strategy of reduced fish oil and vitamin A consumption and increased intake of certain antioxidants (such as lycopene, zinc, selenium, or NAC) may be helpful against cancer.
However, this idea needs testing. No study in animal cancer models has tested this dietary combination.
Given the many proven benefits of moderate amounts of fish oil, I don’t see a reason yet to alter our recommendation that healthy people should eat a pound of fish per week. That said, I do think very high intakes of fish or fish oil are ill advised. And I’m intrigued by the idea that dietary changes may have the potential to play a powerful role in recovery from diseases of angiogenesis such as cancer.
References
[1] Dvorak HF. Tumors: wounds that do not heal. Similarities between tumor stroma generation and wound healing. N Engl J Med. 1986 Dec 25;315(26):1650-9. http://pmid.us/3537791.
[2] Yao JS et al. Comparison of doxycycline and minocycline in the inhibition of VEGF-induced smooth muscle cell migration. Neurochem Int. 2007 Feb;50(3):524-30. http://pmid.us/17145119.
[3] Neuhouser ML et al. Dietary supplement use and prostate cancer risk in the Carotene and Retinol Efficacy Trial. Cancer Epidemiol Biomarkers Prev. 2009 Aug;18(8):2202-6. http://pmid.us/19661078.
[4] Mondul AM et al. Serum retinol and risk of prostate cancer. Am J Epidemiol. 2011 Apr 1;173(7):813-21. http://pmid.us/21389041.
[5] Vogt TM et al. Serum lycopene, other serum carotenoids, and risk of prostate cancer in US Blacks and Whites. Am J Epidemiol. 2002 Jun 1;155(11):1023-32. http://pmid.us/12034581.
[6] Vogt TM et al. Serum selenium and risk of prostate cancer in U.S. blacks and whites. Int J Cancer. 2003 Feb 20;103(5):664-70. http://pmid.us/12494476.
[7] Sarafanov AG et al. Prostate cancer outcome and tissue levels of metal ions. Prostate. 2011 Jan 26. doi: 10.1002/pros.21339. [Epub ahead of print] http://pmid.us/21271612.
[8] Costello LC, Franklin RB. Zinc is decreased in prostate cancer: an established relationship of prostate cancer! J Biol Inorg Chem. 2011 Jan;16(1):3-8. http://pmid.us/21140181.
[9] Epstein MM et al. Dietary zinc and prostate cancer survival in a Swedish cohort. Am J Clin Nutr. 2011 Mar;93(3):586-93. http://pmid.us/21228268.
[10] Noonan DM et al. Angiogenesis and cancer prevention: a vision. Recent Results Cancer Res. 2007;174:219-24. http://pmid.us/17302199.











Thank you, Paul. That advice is helpful (especially as regards bone broth).
Hi Paul,
New to the site – two questions:
1. Just ordered your book through your link to Amazon. Why does it take 2-3 weeks for it to ship, is it a print on demand book or something?
2. You said “high dose fish oil is a well known trigger for rosacea”. Do you have a reference for that. Everything I am finding after some searching to support that suggests taking fish oil as a therapy for Rosacea, with a single source saying that this recommendation has no merit (implying that it is neutral, not causative).
Looking forward to your response.
Hi Craig,
Normally Amazon keeps a stock but this month they have de-stocked. I expect them to go back to keeping a stock handy by next week but can’t guarantee it.
The fish oil trigger is just something I’ve heard from a number of rosaceans. I didn’t experience that myself, but I also didn’t experience any rosacea relief from fish oil. Rosaceans who flush tend to have a hard time with all oils, but fish oil may be particularly difficult.
Best, Paul
Hi Paul,
Thank you for the expedient response. We will do our best to keep scouring your blog for direction while we await the book.
So you had rosacea then? I suspect my wife and I both have it and we both supplement with 2-3g of n3 daily (per Robb Wolf). You noted that Rosaceans who tend to flush (my wife) have a hard time with all oils. Would this indicate that a high fat diet such as the PHD would make symptoms worse? Have your symptoms subsided in the years since you implemented the PHD?
Sorry for the flurry of questions in that paragraph, but the fresh air afforded by an author who answers questions is truly inspiring.
Hi Craig,
2-3 g of n3 daily is too much. I’ve discussed that often, see eg the first post in this series, http://perfecthealthdiet.com/?p=3287.
I think flushing when consuming oils indicates that fat-soluble toxins circulating in the blood are causing the flushing and they can be carried into the body with fat. There are many steps that can be taken to mitigate that, one is to use fat-soluble detox aids like cholestyramine, bentonite clay, or charcoal. The other is to find and cure the source of the problem, often a fungal or other gut infection.
I would not eat an inferior diet just because of toxicity symptoms, but would treat the toxicity directly. However, for rosacea I would recommend being toward the high end of our carb range.
My rosacea seems to be primarily due to Candida and yes, it was worst when I was on a zero-carb diet in 2006-7 and has generally been steadily improving since with the exception of a Candida flare this last winter. That came in part because I was optimizing for bacteria, not Candida, since my semi-disabling brain infection had been bacterial, while things like the rosacea were just a nuisance. But now I’m taking antifungals and trying to rid myself of the Candida, and I think the rosacea may be gone soon.
Hi,
while your book is on the way to me i`m studying your blog.
Your statement in 2011 is long ago.
You wrote you took antifungals. I have rosacea but dont know if have Candida.Which antifungals did you take, and did it help?
Frank
Paul,
Thank you for the candid and personal response. I am now looking forward to the book more than ever.
Sincerely,
Craig
Paul, if one does not have rosacea symptoms, can one assume candida is not present?
Hi erp,
No, but you may be able to assume you don’t have a systemic candidiasis. You may have more localized Candida infections in the gut, vagina, etc.
Got it. Thanks.
Hi Paul,
your n3 comment to Craig has jogged a question of mine;
do you have any views/recommendations regarding ALA (alpha linolenic acid) intake.
come background: I stopped taking flax oil back in January. This also seems to link to when my skin started getting drier & more wrinkled, there were other changes in diet & supps as well, so I can not say for sure if it was related to stopping the flax.
Anyway, i restarted flax oil 17 days ago as a test & i do believe my skin has improved (& definitely has not worsened), still early days tho.
The flax oil i take is labelled 6g Linolenic n3 per 10ml. & I take around 5 to 10ml per day, so that would be in the area of 3g to 6g of ALA per day.
Hi Darrin,
We don’t really have an opinion about ALA. It’s safer (less fragile) than DHA and EPA, so your dose should be fine. Seth Roberts reports it helping balance and gum health. If it’s helping you, take it.
Thanks Paul,
is ALA less fragile than DHA & EPA because it has less double bonds, is it the number of double bonds that determines how fragile a fatty acid is?
Hi Darrin,
Yes.
& thanks for the ref to Seth Roberts & flax.
Seth has plenty of info on his site. Just had a quick browse, i’ll need to read in detail.
He’s experimented with 1, 2 & 3 tablespoons of flax oil a day.
Looks like he currently takes 2 or 3 tablespoons a day (30ml or 45ml), there are a few posts, so i’ll have to find his most recent posts to confirm.
Hi Paul,
Should we not be eating much liver then, if vitamin A can aggravate cancer? Also, should vitamin A rich foods be consumed with alcohol?
Thanks
This is interesting. I’m intrigued by the idea that too much fish oils are not good. How much is too much?
Is cod liver oil included in fish oils?
Following WAPF recommendations I amd my family have been taking Blue Ice Green Pastures fermented cod liver oil with high vitamin butter oil daily. About 1 tsp daily. I take it partly because it’s good for teeth and bones.
Do you disagree with their advice or is cod liver oil different to fish oil? In your book all the references to cod liver oil were positive.
I have an endometriosis diagnosis pending and also bad skin on face – not sure if it’s mild rosacea or different.
Would you recommend I stop the cod liver oil for now?
I now foud out I’m pregnant.
I’m very confused now about what I should be eating. I previously thought cod liver oil was vital for pregnancy. Now I’m wondering if I should stop it as perhaps that’s wha worsened my skin a few years ago when I discoved traditional healthy eating- WAPF, then GAPS, now PHD. My skin is still bad. Cn’t figure out how to improve it.
Congratulations Claire!
I don’t recommend cod liver oil because it’s more nutritious to eat animal liver, spinach and carrots, and seafood for vitamin A and omega-3 fats. You can overdose on both vitamin A and omega-3 fats, so you want to choose your sources wisely.
For skin, try supplementing pantothenic acid daily, optimizing zinc and copper per our advice, and taking some vitamin C. Also eat collagen (bone, joint, tendon in soups and stews) and fermented foods to work on gut flora.
Best, Paul
Thank you so much for your recommendations Paul.
I’ll try what you say. I’ll read more about what you say about zinc and copper, so I can up those. I’ve started taking Vitamin C 2 months ago (2g ascorbic acid and 3 g magnesium ascorbate daily as per recommendations from my dentist) and I have been eating fermented foods and collagen rich soups for the past 3 years daily.
I’ll try the pantothenic acid, perhaps I’m low on that. I like Viridian brand. Now tha I’m preganant I’m extra cautious with what new supplements I should try. I’m deciding between these two:
Vitamin B5 350mg
http://www.viridian-nutrition.com/Shop/Vitamin-B5-350mg-P512.aspx#
or
B complex with Vit B5 in it: http://www.viridian-nutrition.com/Shop/High-Five-B-Complex-with-Magnesium-Ascorbate-P517.aspx#
Which would you recommend please?
Many thanks again.