UPDATE: This was cross-posted on Jimmy’s site, so discussion is occurring on both sites.
I’d like to thank Jimmy for organizing this discussion on the desirability of including starches in a low-carb diet. (See: Is There Any Such Thing as “Safe Starches” on a Low-Carb Diet?). Not many people could bring such a roundtable together, and it’s an honor for us to be part of it.
I think unfortunately the discussion began with a few misunderstandings. So let me start with a few clarifications:
- We advocate a low-carb diet. “Low-carb” to us means eating less than the body’s actual glucose utilization, so that a glucose deficit has to be made up by gluconeogenesis.
- The concept of “safe starches” has nothing to do with their glucose content. “Safe starch” is a term of our invention and refers to any starchy food which, after normal cooking, lacks toxins, chiefly protein toxins. We do not consider glucose to be a toxin, though it may become toxic in hyperglycemia. Thus wheat, which includes gluten and various inhibitors of digestion that survive cooking, is an unsafe starch, while white rice, in which the known toxins (possibly excepting a recently discovered miRNA) are destroyed in cooking, is a safe starch. To say that something is a “safe starch” is not to imply that it is a desirable food for, say, a Type I diabetic.
- Our “regular” diet is not specifically directed at diabetic or metabolically damaged persons. We have a basic diet that is designed for healthy people (represented in the apple – food plate) and we recommend modified versions of the diet for various health conditions – including diabetes.
- We agree that diseases of metabolic derangement may benefit from lower carb consumption than our regular diet. This is especially the case in diabetes, if beta cell loss has reduced basal insulin levels and excessive gluconeogenesis is occurring. In this case, replacing protein rather than providing dietary carbs may be a more helpful strategy.
- We agree that there is no single prescription that is optimal for every person. We often say, borrowing from Tolstoy, that “every healthy person is biologically alike, every diseased person is unhealthy in his own way.” Obesity, for instance, is a heterogeneous disease and there is not a single prescription that will be optimal for every obese person. Diseases of metabolic derangement raise rather complex issues which we explore regularly on our blog. The science remains somewhat unsettled. But we do favor a low-carb approach.
After reading all the responses, it seems to me the debate boils down to two primary questions:
- On low-carb diets, is it better to eat 400 carb calories per day, as we argue, or some lower number of carb calories, say 100 calories per day?
- Are “safe starches” the best source of carb calories?
After answering these I’ll respond to individuals.
Part I: Why Are 400 Carb Calories Better Than 100?
This is a pivotal claim of our diet and apparently the core issue of debate. Allow me to discuss the biology in some detail.
Glucose Utilization of the Human Body
Brain and nerves typically consume about 480 calories per day of glucose. Ketones can displace up to perhaps 60% of this, but ketones do not diffuse well into cortical areas of the brain and the brain always requires some glucose.
After 3 days of fasting, when the brain’s glucose consumption has been roughly halved by ketosis and the rest of the body is conserving glucose, the body’s rate of glucose manufacture in liver and kidneys is about 600 calories per day. [1]
Two things to note:
- Even in fasting, peripheral utilization of glucose exceeds the brain’s.
- The fasting level of glucose utilization is likely to be suboptimal for health: fasting invokes glucose-and-protein-conservation measures which evolved to make us more likely to survive famine, but almost certainly have a cost in long-term health. (The logic is similar to Bruce Ames’s triage theory [2].)
This fasting level of glucose production of about 600 calories per day is a key number: the body must obtain glucose at at least this level, either through diet or endogenous production, if it is to avoid a glucose deficiency.
When not fasting, the body’s glucose utilization is somewhat higher – say, 800 to 1000 calories per day for a sedentary person. Glucose needs are slightly reduced by some endogenous sources of glucose, such as from glycerol released from lipolysis of triglycerides or phospholipids. So the body’s net glucose needs are on the order of 600 to 800 calories per day.
As I noted above, we consider Perfect Health Diet to be a low-carb diet because we favor eating fewer carbs than the body utilizes. For most people, we suggest 400 to 600 carb calories per day, about 200 less than the body utilizes. The remainder is made up by gluconeogenesis – manufacture of glucose from protein. We are a slightly or moderately low-carb diet.
The Human Glycome
Why is so much glucose consumed outside the brain? Immune function (which may utilize significant glucose in people with infections) and glycogen replacement (high utilization in athletes) are two reasons that can be significant in some persons, but in the vast majority of people the biggest reason for glucose utilization is the construction and maintenance of the human glycome.
There are about 20,000 human genes and, due to transcriptional variants and manufacture of proteins from multi-gene subunits, about 200,000 human proteins. However, these proteins are subject to various post-translational modifications, chief of which is glycosylation. Over half of all human proteins need to be glycosylated for proper function, and such is the variety of ways in which they can be glycosylated that there are an estimated 2,000,000 compounds in the human glycome.
These glycosylated proteins coat the plasma membrane of all cells. For many proteins, only glycosylated forms are allowed to leave the endoplasmic reticulum and Golgi complexes where they are formed; nonglycosylated forms are ubiquinated and destroyed.
Nearly every major extracellular molecule has significant carbohydrate content. Glycosaminoglycans such as hyaluronan and proteoglycan components such as heparan sulfate and chondroitin sulfate are important building blocks of the extracellular matrix. Proteoglycans in general mediate all intercellular interactions.
All the body’s lubricating molecules are rich in carbohydrate. Mucins, the most important molecules in mucus, tears, and saliva, are predominantly composed of carbohydrate. Mucin-2, the dominant mucin of the intestine, is 80% sugar by weight.
Production of hyaluronan alone consumes 5 gm, or 20 calories, of glucose per day. [3] I have been unable to find detailed measurements of daily mucin production, but if mucin constitutes 1.5% of the 400 g daily stool weight, then it consumes 5 gm of glucose per day. Since gut flora can break down and metabolize mucin sugars, this may be an underestimate.
So: whole body measurements indicate peripheral glucose utilization of around 100 to 150 g (400 to 600 calories) per day in normal humans, and a mere two of the 2,000,000 carbohydrate-containing compounds in the human body account for nearly 10% of that.
Glucose Deficiency Symptoms
Several responders argued that there cannot be such a thing as a human glucose deficiency on very low-carb diets because blood sugar levels do not leave the normal range.
However, this argument may prove a bit too much, because blood sugar levels don’t leave the normal range during human starvation either, and yet it still proves fatal. Why, if cells can run on glucose and blood glucose remains normal, do starving people die?
A clue is the fact that starving people develop a hacking cough in their final weeks of life. Despite blood glucose levels in the normal range, they cease producing mucus and their airways become dry and irritated.
The reality is this: peripheral glucose utilization is not determined by blood glucose levels, but is hormonally regulated. The brain may import glucose passively, driven by a concentration gradient, but not so the rest of the body. During times of glucose scarcity, blood glucose levels are maintained to sustain brain and nerve function, but hormonal patterns change to prevent peripheral tissues from using glucose to make compounds like hyaluronan and mucin.
What are the hormones that regulate glucose utilization? This is an understudied area of physiology, but the primary regulators seem to be thyroid hormones. During glucose deficiency, T3 thyroid hormone levels decrease and reverse-T3 levels increase. I discussed this in a recent blog post (Carbohydrates and the Thyroid, Aug 24, 2011).
Decreased production of molecules like hyaluronan and mucin and reduced levels of T3 thyroid hormone, then, are outcome of dietary glucose deficiency. Pathologies this may produce include dry eyes, dry mouth, constipation or hard stools, and slow healing of scratch wounds.
Do Glucose Deficiency Symptoms Actually Occur in Low-Carb Dieters?
Yes.
I discussed the reduced mucus production very low-carb dieters sometimes experience in an early blog post (Dangers of Zero-Carb Diets, II: Mucus Deficiency and Gastrointestinal Cancers, Nov 15, 2010). Since that was published, well over 50 low-carb Paleo dieters have reported to me that dry eyes and other mucin deficiency symptoms were cured by adding safe starches to their diet.
I have put up a “Results” page which has case studies drawn mainly from the comment section of my blog. This includes many cases of glucose deficiency symptoms that developed on very low-carb Paleo or GAPS diets and were cured on our diet. (GAPS is a very low-carb diet.) Here is a sampling.
Angie:
All four people in my family experienced a variety of new symptoms (seasonal allergies, constipation, worsening of heartburn, bladder spasms, dry eyes, increasing tiredness and low energy) when we did GAPS. These problems didn’t resolve until we luckily stumbled upon PHD and added back safe starches.
Susan:
I’ve instituted “Paleo” in our house since 1/1/11. Very strict about only plants and protein. About 4/1/11 I realized I was experiencing extremely dry eyes and mouth. I read your post about glucose deficiency and added rice and potatoes back into our diet. This cleared the problem up within 3 days and I was super grateful.
Melinda:
I had severe dry eyes while eating too low carb. Following Dr. Paul’s recommendations at “Perfect Health Diet”, I upped my carbs to his minimum of 50 grams of starch per day and the dry eyes went away.
There are many more cases; in addition to those on my “Results” page, many anecdotes can be found on PaleoHacks and in my comment thread.
What is the incidence of such deficiency symptoms on low-carb diets? At the Ancestral Health Symposium, two dozen people came up to Shou-Ching and I and told us their health had been improved by adding safe starches to their low-carb Paleo diets. As this was about 5% of conference attendance of 500, and not all people at the conference were low-carb and only a minority had tried our diet, I think it’s a safe bet that at least 20% of people who eat very low-carb diets will experience overt glucose deficiency symptoms.
Another Low-Carb Risk: Impaired Immunity
Low-carb diets generally improve immunity to bacteria and viruses, but not all is roses and gingerbread.
Low-carb diets, alas, impair immunity to fungal and protozoal infections. The immune defense against these infections is glucose-dependent (as it relies on production of reactive oxygen species using glucose) and thyroid hormone-dependent (as thyroid hormone drives not only glucose availability, but also the availability of iodine for the myeloperoxidase pathway). Thus, anti-fungal immunity is downregulated on very low-carb diets.
Moreover, eukaryotic pathogens such as fungi and protozoa can metabolize ketones. Thus, a ketogenic diet promotes growth and systemic invasion of these pathogens.
As the fungal infection case studies on our “Results” page illustrate, low-carb dieters often develop fungal infections, and these often go away with increased starch consumption.
Another issue is that mucus is essential for immunity at epithelial surfaces, and glycosylation is essential for the integrity of cellular junctions and tissue barriers such as the intestinal and blood-brain barriers. Thus, reduced production of mucus can impair intestinal immunity and promote gut dysbiosis or systemic infection by pathogens that enter through the gut.
Finally, a very low-carb diet is not entirely free of risks of gut dysbiosis, and not just from fungal infections. Bacteria can metabolize the amino acid glutamine as well as mucosal sugars, so it is not possible to completely starve gut bacteria with a low-carb diet. Nor is it desirable, as this would eliminate a protective layer against systemic infection by pathogens that enter the body through the gut. As our “Results” page shows, several people who had gut trouble on the very low-carb (and generally excellent) GAPS diet were cured on our diet.
The Possibility of Slow-Developing Problems Cannot Be Ruled Out
The majority of very low-carb dieters may experience no immediate ill effects. However, this does not guarantee that problems cannot develop over time.
Is it possible that peripheral downregulation of glucose utilization may increase the risk of some chronic diseases? There is too little experience with very low-carb diets to answer this question, but I think no biomedical scientist would exclude the possibility.
Biomedical researchers are gradually realizing the importance of glycosylation defects in leading diseases. I’ve mentioned previously that downregulation of glycosylation is an important part of the cancer phenotype (see An Anti-Cancer Diet, Sep 28, 2011; Dangers of Zero-Carb Diets, II: Mucus Deficiency and Gastrointestinal Cancers, Nov 15, 2010). A few papers:
- N- and O-glycosylation of proteins in Golgi bodies is impaired in cancer cells. [4]
- Cancer cells have systematically incomplete glycosylation, including deficient galactosylation of terminal beta-N-acetyl-D-glucosamine residues. [5]
- Genetic defects in O-glycans production increase cancer susceptibility. [6]
A recent report in Nature Medicine found that a specific glycosylation defect may commonly underly Type 2 diabetes. [7] From the abstract:
[A] deficit of GnT-4a glycosyltransferase expression in beta cells … produced signs of metabolic disease, including hyperglycemia, impaired glucose tolerance, hyperinsulinemia, hepatic steatosis and diminished insulin action in muscle and adipose tissues. Protection from disease was conferred by enforced beta cell-specific GnT-4a protein glycosylation and involved the maintenance of glucose transporter expression and the preservation of glucose transport. We observed that this pathogenic process was active in human islet cells obtained from donors with type 2 diabetes … [7]
I report these papers, not because I think they tell us how many carbohydrates we should eat – they don’t – but to remind everyone of the complexity of biology.
We lack data on the long-term effects of very low-carb diets. On the Standard American Diet, many diet-induced diseases do not show up for 40 to 50 years. Very low-carb diets have become popular only in the last few years. We cannot be sure that there may not be negative health effects from severe carb restriction that will show up only after decades.
I am not saying that such insidious health effects exist. I am only saying that while I believe low-carb is good, I don’t believe that very low-carb is better, and I think everyone should acknowledge that very low-carb diets may have unexplored risks.
In conclusion: Moderation in carb-hostility is no vice.
Part 2: Are “Safe Starches” Healthy Carb Sources?
So far I’ve defended our recommendation of 400 carb calories per day. Now we reach the question of which plant foods should provide them.
The main choice is between starchy plants and sugary plants. Sugary plant foods typically provide a mix of glucose and fructose; starches digest entirely to glucose.
Loren Cordain, whose “Paleo Diet” recommends a carb intake similar to or larger than ours, favors sugary plants:
[A]nyone who advocates eating white rice and potatoes obviously is unaware of the concept of either glycemic index or glycemic load … Yams, sweet potatoes, plantains and berries are healthful carb sources that most people can eat without a problem.
Yams, sweet potatoes, plantains and berries – all, by the way, foods our diet recommends and that we eat ourselves – contain some sugars which digest to a mix of glucose and fructose, while rice and potatoes contain starches which digest to glucose alone.
Because the concepts of “glycemic index” and “glycemic load” refer to blood glucose levels, they are sensitive to the glucose content of food, not the fructose content. Pure fructose has a glycemic index of only 19, compared to 100 for glucose.
We favor starchy plants over sugary plants for several reasons:
- Nutritional value. Glucose is more nutritious because, as noted above, it has structural uses throughout the human body. Fructose has no structural uses.
- Toxicity. Glucose is less toxic than fructose for several reasons. First, it is less reactive, less likely to glycate (fructate) proteins or promote lipid peroxidation. Second, Paracelsus’s rule tells us that the “dose makes the poison.” Dietary glucose is distributed via the blood throughout the body, so that levels are low in any one location. Fructose, however, is concentrated in the liver.
The body’s evolved machinery for handling glucose and fructose is a good indicator of their relative healthfulness. Glucose is treated by our evolved physiology as a non-toxic nutrient: it is allowed free entry to the blood where it is accessible to all cells of the body. Fructose is treated by our evolved physiology as a toxin: it is shunted to the liver where it is rapidly disposed of.
The toxicity of fructose is well supported by a host of biochemical, biomedical, and epidemiological data. In general, the more fructose people consume, the worse their health. Dr. Robert Lustig spoke at the Ancestral Health Symposium on this topic.
While I think glucose should be favored over fructose, I don’t want to exaggerate the dangers of limited fructose consumption: fruits, berries, and other sugary plants are, in moderation, fine components of a healthful diet. But I see no obvious reason to tout them as superior to starchy plants.
Glycemic Index and Load in Dietary Context
I do not believe that “glycemic index” or “glycemic load” are sufficient indexes of the healthfulness of foods.
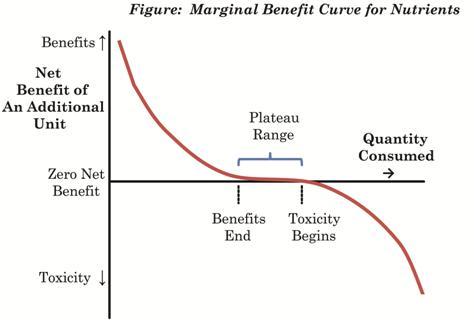
Glucose, as I’ve been arguing, is a nutrient: it has beneficial uses in the body. Nutrients generally deliver their greatest benefits when the body is deficient in them; few benefits when the body is replete; and often become toxic at high doses. Here is a figure from our book (p 4):
A “glycemic load” can be understood as a bolus of glucose delivered to the body. In a condition of glucose deficiency, a “glycemic load” is likely to be highly beneficial: it will be nourishing and repair the nutrient deficiency.
At higher levels of carb intake, a “glycemic load” is likely to be health-neutral – neither damaging nor beneficial. At very high carb intakes, a “glycemic load” may become dangerous.
So knowing a plant’s “glycemic index” or “glycemic load” cannot tell us whether it is good to eat some. That depends on the context of the rest of the diet. On a low carb diet, a safe starch is likely to be nourishing, regardless of its glycemic index.
Issues of Glycemic Control
In interpreting the safety of glucose, there is also the issue of whether postprandial increases in blood sugar can create transient toxicity effects. What is a dangerous level of blood glucose?
In diabetics, there seems to be no detectable health risk from glucose levels up to 140 mg/dl, but higher levels might have risks. Neurons seem to be the most sensitive cells to high glucose levels, and the severity of neuropathy in diabetes is correlated with how high blood glucose rises above 140 mg/dl in response to a glucose tolerance test. [8] In people not diagnosed with diabetes, there is also some evidence for risks above 140 mg/dl. [9]
For several reasons brief excursions above 140 mg/dl are probably not a problem for healthy people. However, for purposes of argument I’ll stipulate that a blood glucose level over 140 mg/dl probably does some mild harm.
Does eating a safe starch necessarily raise blood glucose above this level? No.
I offer as Exhibit A the experience of Haggus Lividus on Jimmy’s thread. Haggus measured blood glucose levels after consuming ~100 calories of rice and found that blood glucose levels peaked at 7.7 mmol/l = 139 mg/dl. Within an hour and fifteen minutes they were back at 5.8 mmol/l = 104 mg/dl. After sweet potatoes, blood glucose peaked at 6 mmol/l = 108 mg/dl.
These are safe levels of blood glucose – below 140 mg/dl at all times. Yet Haggus Lividus took these as levels to be unsafe!
Tom Naughton reports that a potato raises his blood glucose level to 175 mg/dl. This is, indeed, an unsafe blood glucose level.
But he eats a very low-carb diet, and very low-carb diets induce hormonal changes that lead to glucose conservation. One result of these changes is insulin resistance and impaired glucose tolerance.
Thus, an isolated glucose tolerance test is not necessarily a fair test of glycemic control in a very low-carb dieter. Were Tom to eat 400 calories per day from safe starches for a week, he might find his glycemic control was considerably improved. Or, he may find that he is somewhat diabetic and intolerant of carbs in all circumstances.
What is a normal blood glucose response to consumption of a starchy meal? Here is a view of blood glucose levels in normal people as measured by Professor JS Christiansen (from Ned Kock via CarbSane):
Although a majority maintain blood glucose levels below 140 mg/dl at all times, it is not unusual for blood glucose levels to enter the range 140 to 165 mg/dl for brief periods after meals. These measurements were all done in healthy young people.
Vegetables as Poor Glucose Sources
Some responders were understandably confused by a line Jimmy quoted out of context from our book: “don’t count vegetables as as a carb source – they are a fiber (and therefore a fat) source” (page 45).
The point is that vegetables are not usually helpful in repairing a glucose deficiency. A typical vegetable has about 80 carb calories per pound, half as glucose and half as fructose. The digestive tract typically consumes about 50 calories of glucose in digesting a pound of vegetable matter, due to intestinal and immune utilization. Some fructose may be converted to glycogen and then to glucose, but some may be converted to fat and much may be intercepted by gut bacteria. Fructose malabsorption is a widespread problem. So the net contribution of vegetables to the body’s glucose status is small and may be negative.
Since we recommend counting calories only for a few days until one learns how much one must eat to obtain our recommended 400 calories per day of glucose, there is no reason to include vegetables in calorie counting. Vegetables are recommended in our diet due to their micronutrient and fiber content, not their carbohydrate content.
Improved Weight Loss with Consumption of Safe Starches
Since many of Jimmy’s readers eat low-carb diets in the hope of losing weight. It may be of interest to them to know that some of our readers have experienced easier weight loss, reduced appetite, and diminished food cravings after adding “safe starches.” Our “Results” page has examples.
Part 3: Specific Replies
Readers may wish to open Jimmy’s post, Is There Any Such Thing as “Safe Starches” on a Low-Carb Diet?, in another window to follow along.
Colette Heimowitz does not seem familiar with our work, and to have misunderstood the basis for our recommendation of a modest amount of starch. We do not come from a “glucose mentality” and agree that fat and ketones are fine metabolic fuels. However, ketones do not eliminate glucose needs.
The fact that glucose can be formed via gluconeogenesis does not prevent the emergence of glucose deficiency conditions, because the degree of gluconeogenesis is hormonally controlled and may be insufficient to maintain all normal glucose functions.
Maintainance of blood sugar is not an indicator that there is no glucose deficiency.
Glycation is one thing, glycosylation and manufacture of GAGs and other glucose containing structural molecules of the human body is another. We agree that glycation is bad.
I’d like to thank Robb Wolf for his point of view, which is quite reasonable. I am not asserting that no one can do well on a very low-carb diet, only that as carb consumption approaches zero risks of health problems increase. That Robb himself experienced problems on sustained very low-carb is a helpful data point.
I’d like to thank Chris Masterjohn for his contribution. I think Chris has read enough of our work to know that we recommend ketogenic diets as a therapy for various conditions, including neurological disorders of all kinds, and generally hold that dietary adjustments are desirable in many health conditions. So we do not consider that a single macronutrient ratio applies to everyone, but we do believe that intolerance of a “normal” macronutrient ratio is diagnostic of a dysfunction of some kind.
Chris is quite right that it’s a “safe[r] bet” to meet the body’s physiological need for glucose in part by eating glucose. This reduces the risk of failing to provide adequate glucose for optimal cellular and extracellular function.
I’d like to thank Dr. Kurt Harris for his contribution. I discussed Dr. Harris’s post on my blog: https://perfecthealthdiet.com/?p=4802.
Dr Jonny Bowden makes an excellent point: a major advantage of starches over other carbohydrate sources is their lack of fructose. Glucose is, in general, a safer carb source than fructose.
Dr Robert Su directs us to an essay of his, which makes a lot of points that I agree with, but his evidence doesn’t imply the conclusion that all carbs should be excluded, nor does it address the main issues of our diet.
Tom Naughton and I share Irish ancestry, so if he has been extinguished due to lack of ancestral potatoes then so have I. Luckily for both of us, failure to consume safe starches, if that is what our ancestors did, is not so damaging to health as to necessarily result in early death and failure to leave descendants.
That his blood glucose rises to 175 mg/dl after consuming a potato indicates one of two things: his glucose regulation is irretrievably broken and he must never again eat a whole potato in isolation from other foods, or he is insulin resistant in order to conserve glucose and he should eat carbohydrates more often to improve his insulin sensitivity. Which is his optimal course is not something I can know.
Dr Richard Feinman may not have noticed but Shou-Ching and I were at the Ancestral Health Symposium and so were dozens of people following our diet; indeed, about two dozen people came up to us and told us that our diet had improved their health. The most frequently cited benefit was feeling better after adding safe starches to the diet, with relief of dry eyes the most common symptomatic improvement. So if symposium attendees were not dropping like flies, perhaps we deserve a bit of the credit.
Dr. Loren Cordain’s assertion that eating sugary plants like yams, sweet potatoes, and berries is preferable to eating starchy plants like rice and potatoes may be a defensible position, but we believe the evidence is strong that glucose is preferable to fructose as a carb source, and does not support the notion that rice or white potatoes are intrinsically dangerous foods.
Dana Carpender links to one of Mike Eades’s best posts, which we cite and quote in our book’s discussion of why wheat bran is unhealthy. However, it in no way rebuts our observations about the negative health effects of a deficiency of mucus arising from a glucose deficiency.
We agree with Dana that turnips, rutabaga, Jerusalem artichokes, and jicama are fine foods.
Anonymous Prominent Member makes a good point: adding carbs back into a very low-carb diet worked for me, but may not work for everyone. I agree with Anonymous Prominent Member’s point about the importance of practical experience. I think this is one of our greatest strengths. Thousands of copies of our book have been sold, and hundreds of people have reported results back to us. These reports have been overwhelmingly positive. On the blog, I answer questions from people with health problems, ask them to report back results, and many return weeks or months later to report cures or improvements. I invite Anonymous Prominent Member to review the case studies on our “Results” page.
Dr. Uffe Ravnskov can find the scientific studies in support of our views on our blog and in our book. Nowhere do we assert that it is impossible to survive on a zero-carb diet. Rather we assert that a zero-carb diet is suboptimal for health, and not robust to certain health problems, such as some infections.
I would like to thank Adele Hite for her generous statements that our “overall approach is very reasonable” and “may be useful to many people,” and for her engagement on issues of substance.
Adele links to Mike Eades’s excellent fiber post, which we cite approvingly in our book; see my comment to Dana Carpender. The issue Mike discussed, of an excess of mucus due to intestinal injury, is unrelated to the issue we discuss, of a mucus deficiency due to glucose deficiency.
About vitamin C, I think Jimmy may have given this issue quite a bit more prominence than it deserves. It happens that the incidence of kidney stones, glutathione deficiency, and vitamin C deficiency is increased on very low carb ketogenic diets for epilepsy, and other very low carb diets. I made a speculative post attempting to guess the causes of this. To answer Adele, part of the issue is likely a protein deficiency: the need to utilize protein for gluconeogenesis may induce a protein deficiency on an otherwise adequate dietary intake. Other factors are that vitamin C degrades through a pathway that generates oxalate in the kidneys, a risk factor for calcium oxalate stones. Vitamin C does indeed share insulin-dependent receptors with glucose, which implies that glucose competes with C but also that insulin promotes C entry into cells for recycling, so the overall effect of consuming carb-rich foods is unclear. On a low-carb diet adding a little dietary glucose is unlikely to be pro-inflammatory.
About cancer, this is an interesting scientific question. I’ve explained above why a glucose deficient diet can downregulate production of glycoproteins and other structural glucose-containing compounds. However, cancers often evolve an ability to take in glucose independently of insulin and other hormones that regulate glucose utilization in normal cells. As a result, one could argue that things would run the opposite way than Adele proposes: reducing dietary glucose, which generally does not reduce blood glucose levels, will not affect cancer metabolism, but will limit availability of glucose to normal cells for structural use.
I would like to thank Dr. Larry McCleary for addressing matters of scientific substance in a well-reasoned comment. He is quite right that cancers disable glycosylation by suppressing enzymes involved in it. Our reasoning, admittedly speculative, is that (a) the cancer cellular phenotype is a wayward phenotype characterized by reduced intercellular cooperation, cooperation that is largely mediated through glycoproteins, proteoglycans, and glycosylated proteins; (b) cells evolve the cancer phenotype in part by disabling the enzymes which glycosylate proteins; (c) therefore (the speculative inference) dietary steps which downregulate glycosylation may inadvertently serve to entrench or promote the cancer phenotype. This is speculative science, but speculation is the first step in scientific discovery.
Dr McCleary is quite right that depriving cancer cells of glucose is an attractive therapeutic strategy for cancer. However, except in the brain (where ketogenic dieting can significantly reduce glucose levels) this is a difficult strategy to implement. Blood glucose levels are maintained even through the late stages of starvation, and cancer cells can evolve insulin-independence and the ability to import glucose massively from blood. Paradoxically, eating some dietary carbs can even decrease average 24-hour blood glucose levels by increasing insulin sensitivity in normal cells.
I would like to thank Chris Kresser for an excellent comment sharing his clinical experience:
In cases where there is no significant metabolic damage, when I have these folks increase their carbohydrate intake (with starch like tubers and white rice, and fruit) to closer to 150g a day, they almost always feel better. Their hair loss stops, their body temperature increases and their mood and energy improves.
For people that are overweight and are insulin/leptin resistant, it’s a bit trickier. In some cases increasing carbohydrate intake moderately, to approximately 100g per day, actually re-starts the weight loss again. In other cases, any increase in carbohydrate intake – in any form – will cause weight gain and other unpleasant symptoms.
This corresponds precisely with our recommendations. Healthy people will do best on 100-150g per day; obesity is a heterogeneous disease and some will do best on a carb intake in that normal range, others (especially those who are more diabetic) will do best on very low-carb diets. Our “Results” page includes feedback from a number of people who lost weight on our diet better than on other low-carb diets.
I would like to thank Dr David Diamond for a thoughtful comment and for taking the time to read our blog. It is gratifying that he eats largely in accord with our recommendations and has had good results: “This has been my basic diet plan for the past 6 years and my blood lipids have responded in the right directions and I’ve lost about 25 lbs.”
Nowhere do we assert that slipping to 300-400 carb calories is dangerous; rather this is in our “safe range” of 200 to 600 carb calories per day and very close to our estimated optimum. However, I do think that for healthy people the potential harms from very low-carb are greater than the potential harms from excessive carb consumption, so it is perhaps safer to advise eating in the upper end of the range, since a large number of people will deviate from their target.
Dr. Diamond notes that “I haven’t actually seen adverse health outcomes for most people who eat 50-100 gm of carbs/day.” Interestingly, 50 g is sort of a magic number of carbs for many people: there are adverse health outcomes eating less than 50 g, but intake of 50 g or more tends to eliminate them. Our comment threads, and other sites such as PaleoHacks, are full of people who have reported this experience. So I would agree with Dr. Diamond’s statement, but argue that it supports our recommendation to eat at least 50 g of safe starches.
I’ve discussed the cancer issue elsewhere, but I appreciate Dr Diamond’s contribution.
Livin’ La Vida Low-Carb Reader’s carb intolerance is a difficult problem to deal with; I sympathize, and largely agree with what LLVLCR says. LLVLCR may wish to read my reply to Tom Naughton; I would say something similar in LLVLCR’s case. Low-carb is good, control of blood glucose is good, but it is not obvious that zero-carb is optimal.
I agree with Dr. Andreas Eenfeldt that those with diabetes and metabolic syndrome may do better with lower carb intake than is optimal for healthy people.
Dr. Eenfeldt may wish to visit our “Results” page to learn about the mucus deficiency issue on very low carb. It can generally be healed with the addition of 50 g starch to the diet; sometimes vitamin C supplementation is needed as well.
As noted elsewhere, blood glucose levels are not an indicator of the body’s glucose status, and will remain normal even when there is a serious glucose deficiency. Production of glycoproteins such as mucin is a much more sensitive indicator of whole-body glucose status.
Dr. Jeff Volek should be aware that if “there is no defined condition associated with not consuming carbs,” it may be because biomedical scientists have spent little to no time observing people who do not consume carbs. Dr Volek may consult our “Results” page for examples of people who have developed adverse health conditions from very low-carb dieting.
I’d like to thank Dr Jeffrey Gerber for sharing his very interesting clinical experience with cancer patients:
Patients who are ill such as cancer, post surgical, after the hospital are stressed and their basic metabolic rate is increased. In this situation I have found that there is an increased caloric demand. Patients require more calories from fat protein and carbs.
Cancer is a very complex disease and Dr. Gerber’s experience is a helpful reminder that knowledge of the Warburg effect, while helpful for understanding cancer, is not sufficient knowledge to design an anti-cancer diet.
Dr. Jack Kruse’s only substantive sentence is this: “I think avoiding anything that stimulates the IGF1 pathway is ‘smart’ based upon current knowledge and i think using a ketogenic diet is also prudent.”
The dominant dietary factors stimulating IGF-1 release are “protein and energy intake … and energy intake may be of greater importance.” Our diet is generally lower in protein than other low-carb diets, and as a nourishing diet with macronutrient intakes near the body’s utilization needs, it is highly effective at minimizing appetite and total energy intake, as perusal of our “Results” page will show.
Using a ketogenic diet is sometimes prudent. We recommend a ketogenic diet for many neurological disorders and brain cancers, and readers have used our version of the ketogenc diet to cure migraines and ameliorate genetic diseases such as Neurodegeneration with Brain Iron Accumulation (see our “Ketogenic Diet” category for more). We also recommend practices that introduce ketosis intermittently, such as daily intermittent fasting, to everyone as a good general health practice.
Since our diet minimizes IGF-1 and is frequently ketogenic, I would have expected Dr. Kruse to be more positive. Perhaps his reaction may have been just a reflex: more IGF1 reduction, more ketosis, more cowbell. Or perhaps he favors the ultimate in low-IGF1, high-ketosis diets: the Terri Schiavo diet.
Dr. Fred Pescatore should read our book. It is not true that 200 calories of starch will necessarily take a person out of ketosis. Consumption of medium chain triglycerides or coconut oil in conjunction with starches will trigger a mild ketosis, see Ketogenic Diets, I: Ways to Make a Diet Ketogenic, Feb 24, 2011.
Glycosylation of proteins occurs primarily intracellularly in the endoplasmic reticulum and Golgi bodies, not on cell membranes.
I thank Dr. Eric Westman for looking at our web site and trying to understand our diet. Hopefully this response will have made things clearer.
Peter Dobromylskyj of “Hyperlipid” has had a very busy year with a new daughter and new home, so I’m not in the least surprised that he hasn’t yet had time to read our book. I hope he will enjoy it when he does, as he is one of my favorite health writers.
The human glycome is much more than a lectin signaling system: it has a myriad of structural and functional roles, some of them discussed above.
Re “I can’t see glucose deficiency being a gut problem as this is the organ with the highest exposure to dietary glucose,” two factors which limit availability of dietary glucose to gut cells are (a) dietary glucose is absorbed in the small intestine but gut problems are most common in the colon where bacterial populations are highest, and (b) we are considering very low carb diets that provide little dietary glucose. A third factor to consider is that the gut, due to its mucin production, immune activity, and rapid turnover in cells and extracellular matrix, is a major consumer of glucose.
Cancer is an extremely complex and interesting disorder and I’ll be delighted to hear Peter’s ideas.
Peter makes an extremely important point: that minor dietary defects may take decades to reveal themselves. On the Standard American Diet, an unhealthy diet, it often takes 50 years for chronic diseases to appear. If there are problems with very low carb diets, we should not necessarily expect them to appear immediately.
Peter says “I don’t know,” but in truth we all don’t know: dietary science is complex and all of our positions are somewhat speculative. Thus humility is in order.
I thank Dr. William Davis for his assessment that our “diet seems a rational, workable program” and agree with him that diabetics will benefit from reducing starch consumption.
Valerie Berkowitz should be aware that we do recommend tomato consumption, but we do not consider it a “safe starch” because its calories are mainly in the form of sugars. Her other concerns are addressed above.
We agree with Diane Sanfilippo’s observations.
Dr William Yancy seems to be intelligent, reasonable, and unfamiliar with our diet. Perhaps the exposition above will help.
Dr Ann Childers links to an article in Discover magazine and avers that the humans of the Ice Age and the Inuit were “without cancer, diabetes, tooth decay, glutathione deficiency, vitamin C deficiency or gut dysbiosis.” These claims are unsupported. Nor is it the case that Ice Age humans ate zero-carb diets, nor any other humans who had access to starchy plants.
Dr Cate Shanahan makes two important points with which we wholeheartedly agree.
First is her observation that the protein quality of food, especially the presence of immuno-reactive proteins, is extremely important for health. Indeed, our “safe starches” are defined by their lack of these toxic or immunogenic proteins. We strongly agree with this point, and it is a centerpiece of our diet.
Second is the point that just because it is possible to manufacture glucose from protein does not mean that optimal amounts of glucose will actually be manufactured if none are eaten. It is well established that macrobiotic dieters, who eat low-fat diets, can develop lipid deficiencies, notwithstanding the fact that lipids can be manufactured from glucose. Something similar can happen on very low-carb diets, especially if dietary protein is insufficient.
Amy Kubal seems to be under the misimpression that I recommend 1 pound of safe starches daily for “everyone.” No, this is a recommendation for healthy people, I understand that some people with defects of metabolic regulation or neurological disorders will benefit from ketogenic diets or severe carb restriction.
I agree with her advice about the benefits of carbs following workouts. The reason we recommend not counting carb calories from vegetables was discussed above.
It is not obvious to me from her description that her recommended cancer diet differs much from ours.
Dr Robert Su refers us to a column of his. It makes a lot of points whose truth I acknowledge, but doesn’t address any of the arguments I’ve made, and certainly doesn’t support the conclusion that there is no benefit from dietary carbohydrate.
I applaud Mark Sisson’s comment. Primal and Perfect Health Diet are indeed extremely close, and Mark properly focuses on the important points, such as avoiding grains, fructose, and seed oils. Mark’s easygoing attitude toward unimportant differences is praiseworthy.
Dr Lauren Noel notes that other than a few minor cell types, “all tissues can run on ketones,” and supposes this refutes the need for dietary carbohydrate. However, although the brain can run on ketones, it turns out that ketones don’t diffuse well to the cortical areas of the brain, and the brain always requires some glucose even in extreme ketosis. Also, while ketones can replace glucose as a fuel, they cannot glycosylate proteins, or generate ROS in the manner needed by immune cells.
Dr Noel believes that eating white rice and sweet potatoes will aggravate Candida infections. Dietary carbs can feed Candida in the gut, but they also feed competing probiotic bacteria and promote intestinal barrier integrity and immune function, and thus their effect on the gut flora is complex. More importantly, ketosis promotes systemic invasion by Candida and glucose is needed for the immune defense to Candida, so a moderate carb intake is helpful to the defense against systemic Candida. As Candida is an effective intracellular pathogen that can flourish systemically, this is a very important consideration. No one with a Candida infection should eat a ketogenic diet. Dr Noel might wish to consult our “Results” page for a few cases in which fungal infections were exacerbated on very low-carb diets and cured on our diet.
Dr Daniel Chong is quite right that starches have been a part of the evolutionary human diet, since at least Australopithecus 3.5 million years ago. The history may go back even farther: recent anthropology speculates that the common human-chimp ancestor may have been bipedal and lived in open woodlands where starches but not sugary fruits were the predominant food.
Dr Greg Ellis is rather quick to assert that our work is “made up” and “constructed out of thin air” even though he acknowledges not having read our book, and is under the misimpression that we have “bought into the dangers of fat and cholesterol.” He asserts, “If you want to talk about toxins then glucose is at the top of the list” which is absurd; among sugars alone, fructose is more toxic than glucose. He asserts, “If glycosylation is truly important there is enough glucose available to perform this function without eating glucose or carbs” which is precisely the point at issue. He blames cancer on glycation of proteins, a highly dubious claim. He is unaware that fungi are eukaryotic organisms that have mitochondria.
Dr Ron Rosedale has written an extended commentary which deserves a considered response. Since he posted a series on Facebook to which I had already begun drafting a reply, I’ll finish that and post it on my blog next week. I thank Dr Rosedale for the time he’s given to this discussion.
Dr Joe Leonardi’s comments are intelligent, and it sounds as though his own dietary advice is excellent. I thank him for his contribution.
Dr BG makes an excellent point: that carbs do in practice improve the health of many paleo dieters, in part via improving adrenal function. Dr BG herself reports, “I feel ‘better’ on higher carbs for the adrenals.” Dr BG also notes, “On Paleohacks there are countless stories of people on VLC paleo who feel dizzy or lightheaded. H-E-L-L-O this is cardinal signs and symptoms of adrenal fatigue. Many of these folks are also doing HIIT and hard core CROSSFIT!” Of course, exercise utilizes glucose and will exacerbate any glucose deficiency.
These cases of improved health upon higher carb consumption should be a warning to those other writers who question whether it’s possible to have a glucose deficiency.
Zoe Harcombe appears to approach dietary science from premises similar to ours. She shares our nutrient-based view and general orientation.
On the issue of taste, we do recommend that starches be eaten as part of a meal in combination with sauces, vegetables, fats, and meats. So yes, rice will often be combined with curry. In our “Food Plate,” the body of the apple signifies foods that are best eaten as part of a meal – starches, vegetables, meats, soups, sauce – and the “pleasure foods” are good snacks or desserts.
Our bodies do need glucose, and it may be preferable to obtain it directly from diet than to have to manufacture it from protein.
An appropriate population of commensal bacteria tends to stabilize the gut and make it resistant to dysbiosis. Antibiotics, starvation of carbohydrates, and other factors that deplete gut bacteria may increase the risk of fungal or other infections.
We do recommend lower carb consumption for diabetics.
The amount of glucose in blood is not related to the amount of glucose the body consumes in a day. The “stock” of glucose in blood is continually replenished by a “flow” from the liver as tissues draw it down. It is the flow, integrated over 24 hours, which is the daily glucose consumption.
The Taubesian idea of intentionally creating a glucose deficiency to force the body to breakdown triglycerides for glycerol is a clever but flawed strategy for weight loss. Its chief defect is that triglycerides break down to about 11% glucose by calories, but the body’s glucose utilization is close to 30% of energy. As a result, this strategy cannot meet glucose needs without releasing free fatty acids beyond energy needs. If these are not successfully disposed of, then blood free fatty acid levels may become elevated, which leads to the phenomenon of “lipotoxicity” which can promote diabetes. Whether and to what degree glucose deficiency and lipotoxicity would occur in any attempt to execute such a strategy is an empirical matter, but no reader should assume that such a strategy is riskless.
There is room to disagree about the optimal level of glucose intake, and I hope Zoe will look into our arguments for a slightly higher carb consumption than she is used to.
Dr Stephen Phinney seems to be under the misimpression that my term “safe starches” refers to low glycemic index foods. No, it has nothing to do with the carbohydrate; “safe” means that after cooking the food lacks toxic, bioactive, or immunogenic proteins. It is about the plant proteins, not the carbs.
Dr Phinney avers that “there is no absolute human requirement for dietary carbohydrate.” I am not sure what “absolute” means, but I do believe that health will usually be improved if the diet includes some carbohydrate.
Dr. Phinney defends his statement by reference to blood sugar levels. As discussed above, blood glucose levels are not an adequate indicator of the body’s glucose status.
Re the issue of vitamin deficiencies, there are plenty of reports of nutrient deficiencies on clinical ketogenic diets, thus Dr Phinney’s need to include the adjective “well-formulated” before ketogenic diets. I agree with him on this point: it is possible to formulate ketogenic diets in such a way that they don’t generate nutrient deficiencies. However, it is perilously easy to misformulate them. Diets should be robust to error. When carbohydrate intake approaches zero, diets become less robust. Since few people know how to properly formulate a ketogenic diet, this has to be considered a risk to low carb diets.
On the issue of dysbiosis, I assume Dr Phinney will agree that some non-zero level of mucus production is optimal, and that a level of mucus production below that optimum impairs health.
Dr Richard Bernstein is the author of a book we frequently recommend to diabetics, so it’s unfortunate that he may have gotten the mistaken impression we recommend higher carbohydrate consumption for diabetics. Perhaps he’ll look more closely into our diet and reconsider his judgment.
References
[1] Nair KS et al. Leucine, glucose, and energy metabolism after 3 days of fasting in healthy human subjects. Am J Clin Nutr. 1987 Oct;46(4):557-62. http://pmid.us/3661473.
[2] McCann JC, Ames BN. Adaptive dysfunction of selenoproteins from the perspective of the triage theory: why modest selenium deficiency may increase risk of diseases of aging. FASEB J. 2011 Jun;25(6):1793-814. http://pmid.us/21402715. McCann JC, Ames BN. Vitamin K, an example of triage theory: is micronutrient inadequacy linked to diseases of aging? Am J Clin Nutr. 2009 Oct;90(4):889-907. http://pmid.us/19692494.
[3] Stern R. Hyaluronan catabolism: a new metabolic pathway. Eur J Cell Biol. 2004 Aug;83(7):317-25. http://pmid.us/15503855.
[4] Hassinen A et al. Functional organization of the Golgi N- and O-glycosylation pathways involves pH-dependent complex formation that is impaired in cancer cells. J Biol Chem. 2011 Sep 12. [Epub ahead of print] http://pmid.us/21911486.
[5] Satomaa T et al. Analysis of the human cancer glycome identifies a novel group of tumor-associated N-acetylglucosamine glycan antigens. Cancer Res. 2009 Jul 15;69(14):5811-9. http://pmid.us/19584298.
[6] An G et al. Increased susceptibility to colitis and colorectal tumors in mice lacking core 3-derived O-glycans. J Exp Med. 2007 Jun 11;204(6):1417-29. http://pmid.us/17517967.
[7] Ohtsubo K et al. Pathway to diabetes through attenuation of pancreatic beta cell glycosylation and glucose transport. Nat Med. 2011 Aug 14;17(9):1067-75. http://pmid.us/21841783.
[8] Singleton JR et al. Increased prevalence of impaired glucose tolerance in patients with painful sensory neuropathy. Diabetes Care. 2001 Aug;24(8):1448-53. http://pmid.us/11473085. Hat tip Jenny Ruhl, http://www.phlaunt.com/diabetes/14045678.php.
[9] Ziegler D et al. Prevalence of polyneuropathy in pre-diabetes and diabetes is associated with abdominal obesity and macroangiopathy: the MONICA/KORA Augsburg Surveys S2 and S3. Diabetes Care. 2008 Mar;31(3):464-9. http://pmid.us/18039804.











potatoes + meat = increase your iron stores!
milk + meat = decrease your iron stores!
mrs potato doesn’t look safe to me… (meat eater)
or … potatoes + milk + meat = perfect health?!
Hi Marilyn,
One of the privileges of not being a medical doctor is that I get to avoid thinking about how drugs affect the body. 🙂 However, my understanding is that sulfonylurea by increasing insulin levels will inhibit gluconeogenesis and increase peripheral glucose utilization.
Hi Monte,
We’ll consider that for the next edition of our book.
Hi mem,
Thank you!
Hi Oskar,
I’ll discuss that paper on Saturday.
Hi JS,
I would have liked to include a discussion of glycemic index of meals, but ran out of time. I may blog about that next week. Thanks for letting me know about your posts, I’m sure they’ll have the subject well covered.
Hi Ellen,
I’m going to get some kind of “start here” page up when I get a chance … Now that the Q&A and results pages are up, that’s the next addition.
Hi Chris,
It’s certainly true that avoiding starches can be helpful for recovery from some infections / gut dysbioses.
Dr Ebringer’s work linking Klebsiella, branched starches, and specific diseases is very important. I wish more researchers were investigating these food – pathogen – disease connections because I think they are the key to medicine. But he is a rare investigator.
Hi majkinetor,
Since glucose utilization is reduced in fasting, this is an underestimate of glucose needs. So it strengthens my case that dietary glucose is desirable.
That glucose utilization is further reduced on longer fasts is true, but since I want to establish what non-fasting glucose needs are, there’s no value to my argument in looking at longer-term fasts.
I agree that hormonal dysfunction and malnutrition can impair glucose regulation.
You make good points about the connection between pancreatic function and adrenal fatigue.
That glycerol rises to 21% of glucose production during fasting (ie 21% of ~600 calories per day, or 120 calories) confirms my point that it can only provide 100-150 calories, not all of our glucose needs.
Re starvation, that is my point. If normal blood glucose was enough to get tissues to take whatever glucose they wanted, either for structural use or for energy, there would still be mucus in starvation and health wouldn’t decline until blood glucose levels declined.
I agree that we have to look at the interaction of glycemia with bacterial infections, this was actually one of our arguments for low-carb dieting in our book. But I don’t think this is a decisive argument against eating any carbs.
I agree with what you say about cancer. But that doesn’t tell us what the effect of dietary variation on the cancer will be.
Great find showing that alcohol can impair glycosylation. This is a good point, but doesn’t show that low-carb can’t do it too.
I do not believe a hibernating animal is a good comparison for an active human. With our big brains, we use a lot more glucose; in hibernation glucose needs are reduced. There is enough protein-gluconeogenesis to meet a hibernating animal’s needs. Not necessarily so in humans.
I agree that the blood glucose graph probably represented high-carb junk food diets. This supports my point that our diet is safe, because our lower-carb starches-in-meals diet should have reduced blood glucose excursions.
If you read my kidney stone post, you’ll see that vitamin C needs to be doubly oxidized in order to generate oxalate, singly oxidized C doesn’t generate oxalate. So the risk from C to stones is mainly when there is a dire deficiency of antioxidants, especially glutathione. High C intake can improve overall antioxidant status, including glutathione, and move C into the singly oxidized rather than doubly oxidized state. On the other hand it increases the amount of C around to get doubly oxidized. So the effect of C supplementation on stone formation is unclear. But glutathione supplementation should be categorically good.
maj, thanks for all the paper links and ideas. I don’t think you’ve damaged my case for carbs, and I’m glad you eat the carbs yourself!
Best, Paul
Hi Skyler,
My keyboard is 6 years old and still hasn’t been yelled at, punched, or thrown against the wall.
Hi CarbSane,
Since I don’t know what the optimal diet for diabetes is, the science is unsettled in my view, and very basic issues were being contested, I didn’t think this was the proper forum to discuss diabetes diets.
However, I may have conceded a bit less than you think. Low insulin production leading to spontaneous hyperglycemia is characteristic of Type I diabetes but isn’t that common in Type II. I usually put “may” in my sentences about very low-carb being beneficial for diabetics. I haven’t re-read it to check this, but I think for the most part I left the issue of what is optimal for diabetics open.
Thanks for the links, I appreciate your bringing these diabetes papers to our attention, it’s valuable to get a range of views in my reading and yours is a voice that isn’t duplicated elsewhere.
Hi Els,
That’s great news! Keep me posted on how you’re doing.
Best, Paul
Paul, it’s sentences like this, One of the privileges of not being a medical doctor is … that keep me reading your technical posts and comments even when they’re way over my pay scale!
Brilliant exposition, Paul
I especially liked your elaboration on the Glycome.
My only complaint is that your responses were so “nice” in avoiding all the snark and idiocy that was tossed your way that I kept going back to Jimmy’s blog to see what the commenters had actually said. The bowdlerized LLVLC symposium, stripped of the ignorant and obviously incorrect, would have only been a few merciful paragraphs long. We could use more cowbell from you!
Finally, you say:
“As a result, this strategy cannot meet glucose needs without releasing free fatty acids beyond energy needs. If these are not successfully disposed of, then blood free fatty acid levels may become elevated, which leads to the phenomenon of “lipotoxicity” which can promote diabetes.”
I think the free fatty acids would not be disposed of in a regime of energy excess, but that would be the case with any hypercaloric regime of total energy excess, and not particular to VLC diets. Are you intending to give the impression that a low carb diet could cause diabetes when there is energy deficit due to some level of “lip toxicity” unique to VLC? I would take issue with that, I think.
There is no doubt that cellular lipotoxicity exists and is part of the sequence of disturbed metabolism leading to T2, but this is a reflection of energy excess and not really likely to be caused by excess fatty acids due to accelerated lipolysis to scavenge the glycerol backbone for glucose.
I don’t think Taubes’ scenario of elevated NEFA solely as a consequence of glycerol scavenging actually occurs, but perhaps that is the point you are trying to make and I am just being dense : )
Hi Kurt,
If I’d responded to the idiocy, it would have taken me another two days to finish the post.
My statement about the lipotoxicity wasn’t about what actually happens, it was about what logically would happen if somehow glycerol from fats were able to meet the body’s glucose needs. It was really a reductio ad absurdum meant to show that glycerol isn’t adequate for glucose needs, not that a VLC diet causes lipotoxicity.
As I’ve written before (see eg this post http://perfecthealthdiet.com/?p=4383 and scroll down to CarbSane or lipotoxicity), it’s not obvious to me which diet would maximize lipotoxicity. High carb diets might be more lipotoxic than high fat diets.
I agree about the excess energy balance creating lipotoxicity.
Perhaps I didn’t write it well enough. Well, hard to be completely clear when working hastily.
” It was really a reductio ad absurdum meant to show that glycerol isn’t adequate for glucose needs, not that a VLC diet causes lipotoxicity.”
Makes sense to me now and I agree with that.
Again, congratulations on well reasoned and readable response.
Kurt
I am blown away! Thank you Paul, reading your posts especially such as this one, is as always very educational and valuable in many levels. I have ‘liked’ you in Facebook and I can already see some of my friends and family taking an interest in what PHD is all about.
When I read your response here, I thought “Wow, first it was Stephen Guyenet vs. Taubes. Now, it’s Paul Jaminet vs pro low carb gurus”, although I do understand it’s not so much of who vs who.
As always, you remain calm as ever. Is this the result of PHD? You bet 🙂
I am a 68-year-old obese man with diabetes, and I refuse to take any medications whatsoever, which irritates my doctors considerably. Instead of assaulting my body with drugs, I prefer to just get out of the way and trust the body’s healing processes that have worked for our ancestors for millions of years. All I try to do is provide proper nutrition for my body. Unfortunately, as your post illustrates, there is no universal consensus on what is proper nutrition. At the moment, I am on a very low calorie apple juice fast or diet. I have read everything for Ornish to Atkins, and I’m still just having to use trial and error to find what works for me.
USDA DB shows 0.50g fructose for 100g sweet potato baked, and 0.36g for baked white potato. That’s really not a lot of difference. So to get 100g (400 calories) carb from these potatoes would mean only 0.7g difference in fructose. Since sweet potato has a significant difference in vitamin A then, I’d suggest that sweet potato has a superior nutritional value compared to white potato and the fructose difference is not worthy of concern.
Jim Purdy
There might not be a perfect known diet for diabetes, but approximately six months ago, my dad, an obese man in his early 70s with Type II diabetes and recovering from congestive heart failure (with other health problems as well), began following a not-especially low carb version of PHD along with daily intermittent fasting.
Not only has he lost around 30 pounds, he’s been able to go off all his meds except for insulin, which he has cut in half. Although his blood pressure is still high, it’s pretty good for him, and most of his other numbers have gotten better. His glucose is the best and most stable its been in a very long time, possibly decades. I plan to write more about him and show some before and after photos, with more detailed numbers and so forth, when I get the chance.
He feels the best he’s felt in a long, long time. Where he used to say, “If I live,” now he’s sure he’s going to live. Interestingly, he’s stopped snoring as well, along with many other symptoms of better health.
I could write a lot more about him and plan to do so in the future.
Best of luck,
Peter
I wish there was a sort of conclusion in your post, summarizing all your main ideas in one parapraph.. this is too scientific for me to read sometimes..
Cheers
@ Jim Purdy
My step dad was diagnosed T2D and had to take Metformin (high dosage) I convinced him that his problem wasn’t high glucose but high insulin levels and that Metformin was just a bandaid. I managed to get him to read Sisson’s articles at MDA and follow the Primal Blueprint. This was NOT easy-he is very stubborn. But Mark does have a way with words and now my step dad-in 8 months-has great BS readings and does not take any medication. His best friend is also T2D and used to take 6 “mega shots” (his words) of insulin everyday and now, after about 6 months, he is down to one shot per day. They both have lost weight and both are in their late 50’s. Dont give up! the PHD or Primal Blueprint are actually perfect to handle diabetes. Just dont listen to the ADA!! They want you to be sick! Lower the carbs, check your BS after every meal and continue the self experimentation. Only you knows what works best for you. Paul can and will help you. Ask anyone else that posts here. Mark Sisson can and will help you also. Good luck! I hope you can kick diabetes in the ass! —I also know that my advice on glucose and insulin to my step dad was a gross oversimplification but he is NOT a science type so I had to really shock his mind to get him to listen—
While the LLVLC post muddied the waters, it also provided the opportunity to clarify questions many of us had about your recommendations.
Jimmy mentioned that you would be working with him on a protocol for testing his responses to safe starches. Would you be willing to share the protocol with your readers so that we might all share and compare?
It would be good to test a baseline of a single simple ingredient such as 75 grams of plain potatoes or rice, then test the same amount in combination with a fixed amount of fat and/or protein or both. Te protocol and reader’s responses would make for an informative thread of N=many.
awesome! thanks.
on Jimmy’s blog, it’s amusing that
some people’s carb phobia is quite similar to the SFA phobia of most conventional MDs. my respect for some of the well known experts just drops.
(Mark Sisson is a very cool guy/)
cheers,
Hi Paul,
I am a little late reading your posts. I wanted to say that my family and I are very grateful for your work. You bring very fresh ideas and scientific discussion to the “low carb” community. Science is always evolving and it is healthy to have constructive discussions.
I have been seeing a lot of comments about how fructose is toxic. Fruit is often avoided due to it’s fructose content in the low carb community. However, I wonder if this is misguided. Generally, fruit comes with antioxidants and other nutrients that may protect us from the toxic potential of fructose. I think nature added these antioxidants to protect the plant sugars from oxidation or from reacting with other molecules. So there is a possibility, we may be protected from fructose reacting with our own cells, proteins, etc. I think the real problem stems when we consume refined sugars such as soda and candy. These may be far more reactive or inflammatory than eating a piece of fruit due to the lack of antioxidant protection. You could make the same argument for walnuts or nuts too. They come packaged with antioxidants that prevent the pufas from oxidizing.
I think if the only fructose that we are exposed to is from fruit then the risks of toxicity are very minimal.
Hope all is well.
Erik
I have to say, I really like your apple graphic that represents the PHD (saw it on Jimmy’s blog). I really like the use of the yin yang symbol, and the clever use of the shadow, leaves and stem. Too bad the USDA can’t come up with something as honest and useful.
Hi Paul,
Great post. Just to be clear, my comment was not meant as a direct criticism but rather advice about interpretation and application. Jimmy asked me about what I thought of your idea of safe starches and the recommendation to consume 400-600, so I was clarifying that any specific numbers should be taken as a starting point for an individual to tweak, and not trying to imply that you would disagree with that.
Chris
Hi Jim,
Yes, it’s hard to know what’s going to be best for diabetics in the long run. Fasting is a good thing to try. Let me know what you learn.
Hi Cris,
I agree that sweet potatoes are fine foods, but there are different kinds of sweet potatoes with different nutritional profiles. Potatoes are fine too.
Hi Peter,
Fantastic story! I would love to hear more.
Hi Jack,
Maybe I’ll do a conclusion in next week’s post.
Hi daniel,
Our diet is surely much better than the ADA’s! Great story about your stepdad!
Hi Adriana,
We’ll publish a 7-day meal plan that we recommend to Jimmy, anyone else will be able to use that too.
Hi Erik,
I agree with you, fruit isn’t a concern as a practical matter. It typically has only 200 calories per pound, half fructose, so even after a pound you haven’t eaten much fructose. The soda and candy is what really does people in.
Hi Chris,
Maybe we’ll do a hostile takeover of the USDA.
Hi Chris M,
I didn’t think it was a criticism, but thanks for clarifying. Looks like we both met Patrick Timpone this week!
Hi Paul,
You said: “Yes, it’s hard to know what’s going to be best for diabetics in the long run.”
I don’t know in the case of type I, but for type II I suspect that PHD, with some ‘safe’ starches and fermented food, should be best.
If we think about some things that have been show to help in type 2 diabetes, we will realize that gut disbiosis is key. Some examples:
a. Resistant starch (pubmed 20536509, 18356328, 17605234);
b. Colostrum (18602824);
c. Treatment of periodontal diseases (20682017, 21859323, 21782948, etc, etc, etc);
d. Gastric bypass. Gastric bypass is clearer more effective on diabetes over gastric banding and weight loss. It’s effectiveness is because of alterations in gut flora? (19164560, 21853297, 21949514, 20212498);
e. Fermented food (11481402, 11285328).
Excellent post, I appreciate the extensive explanations and the “nice” tone is very refreshing.
I have found that PHD works great for me, going to full-fat dairy from low- or no-fat and keeping white rice and some potato in my diet made giving up wheat and other problematic grains a breeze – no bread or cereal cravings at all! It’s also fairly easy to modify standard recipes to make them PDH-compliant, particularly when using cookbooks like the “Joy of Cooking” that predate the low-fat, high carb fads. My daughter particularly loves French cooking (my mother was French) and PHD is very French-cooking friendly! A more strictly paleo diet would be too restrictive for us.
Hi Mario,
You’re a treasure. Thanks for giving me a lot to think about!
Hi Suzanne,
I agree, if the only version of Paleo I had seen was “lean meat and vegetables” I never would have tried it. We’re big fans of Julia Child and French food!
“My only complaint is that your responses were so “nice” in avoiding all the snark and idiocy that was tossed your way” (quoting Kurt Harris).
I think Dr Jaminet delicately unsheathed his claws once or twice, all the more effectively for having indeed avoided any hint of “snark and idiocy”.
I’ve bought the PHD book, of course, but I’m tempted to buy another copy just as some sort of payment for this highly informative and very clearly written post.
Buy one and send it to me! {wink}
After eating a meat and vegetables diet for a 1.5 years I read PHD and added back starches. I had been craving them, so it wasn’t hard to do.
The addition of starches warmed my body temperature (always an issue because I have Hashimoto’s thyroiditis), improved my energy level, helped with symptoms of adrenal fatigue (as per Dr. BG), improved my bowel function, and improved my mood. I also reduced my grocery bill (which in turn made for a more harmonius family life) because I instantly desired about one-third of the protein I used to eat.
Of all the symptoms of glucose deficiency the most concerning was the flat mood. Clearly my brain was low on energy despite the “no human requirement for carbohydrate” dogma.
Many thanks to Paul!
Phenomenal response with class and dignity. Thanks Paul for this thoughtful and comprehensive post.
Did you see Richard Feinman’s reply over at Jimmys:
“When I suggested people at the AHS meeting were “dropping like flies” from glucose deficiency, that was a joke, like ha, ha. The idea that we have not found glucose deficiency due to low-carbohydrate diets because establishment medicine has not looked for it is ridiculous. That’s all they do look for. In any case, worrying about something that hasn’t been, found for whatever reason, is the flip side of the ADA’s take on how good fiber is for you that I quoted in my blog post ( http://wp.me/p16vK0-6B ): fiber “may contain nutrients that haven’t even been discovered yet!” (their exclamation point).”
I am deeply impressed by your considered, courteous and incredibly thorough response, especially given the impulsive, needlessly offensive character of some of the comments you were responding to. If only more people could argue like you do. When I next get involved in a heated debate, I’m going to try and deal with it in the manner you have done here.
Peter, thanks so much for sharing!
Hi Sue,
Thanks for letting me know, I replied to him over there. (Basically referring him to the results page and VLC dieter experiences which establish the possibility of a glucose deficiency.)
Hi Nicolas, in my youth I would have been more tempestuous but after years in business, I learned to get work done quickly and efficiently.
fats and protein are loaded with carbon and hydrogen , and we are always breathing oxygen rich air . whats a carbohydrate again?
a mere two of the 2,000,000 carbohydrate-containing compounds in the human body but we do have the necessary components to make these without consumption of starchy foods.
that being said ‘ I’m young and lean and like starch in the mix.
Really enjoying this blog. I just have one question. I’ve been reading the Leangains blog on IF and training. They recommend eating starches only on training days and non-training days they recommend sticking to meats, vegetables, nuts, seeds & no starch.
What’s your opinion on this? Do you still recommend starches on training days?
Thanks.
Hi Shameer,
I agree with Martin’s basic recommendations. I’d recommend more starches (and protein) on training days, less starches on rest days, but I would still eat some starch every day. At least 200 starch calories on rest days, you could easily eat 1,000 or more on workout days.
Paul wrote: “you could easily eat 1,000 [starch calories] or more on workout days.”
I’m curious how you arrived at this. Is it based on the amount of glycogen depleted by a high-intensity whole-body resistance workout?
Hi Bill,
Yes, though more based on running … 300-400 glycogen calories per hour for runners, less for resistance exercise.
So 1 hr/day training for a runner may increase glucose utilization to 1,000 calories/day.
Hi Paul,
If you are still planning on posting your Dr Rosedale response. This comment from Rosedale support may be of interest to you; https://drrosedale.tenderapp.com/kb/about-the-diet-and-what-to-expect/body-temperature
excerpt below;
“The best place to measure is under the tongue. Ideal basal temperature is what you have when you first wake up in the morning, and on the Rosedale diet should be upper 96’s lower 97’s. We have found that when someone starts our diet, their basal temperature will go down about 1-2 degrees Fahrenheit which is a great improvement”.
Personally, i did not feel good on a lower body temp when i was low carb (sub 50g). & have been working hard (following phd diet & supps) to get my body temp back up. i would say my basal/morning oral temp is now around the 97.5F on average (up from around 96.5F average pre PHD).
Thanks, Darrin.
Yes, I know he believes the low T3 pattern that accompanies very low carb is beneficial for longevity. I think the evidence for longevity is doubtful and there are plenty of defects.
Best, Paul
Paul,
This LLVLC exchange was your Austerlitz, masterfully executed. Kudos
Regrettably, I must admit that until this point I had not read much of your work. This mistake is now being remedied post-haste.
Thanks, David. Not sure I like the Austerlitz comparison though, I do hope to have a longer career than Napoleon!
Hahah, touché!
I have a question regarding spiking blood glucose, glucose tolerance, and cycling of carbs. I eat ‘safe starches’ two or three times a week (m/w/f) after my workouts, but at all other times I’m VLC. Would my glucose tolerance be lowered if I only eat starches 2-3 meals a week and would that result in harmful bg spikes after those meals?
Hi haig,
You would become more insulin sensitive and glucose tolerant if you ate carbs more often, but unless you’ve tested yourself with blood glucose meter there’s no reason to think you are getting harmful blood glucose spikes now.
I would recommend eating your “safe starches” as part of a meal that includes fats, vegetables, and preferably an acid like vinegar. All of those will lower the glycemic index and prevent any harmful blood glucose spikes.
Best, Paul
Hi Paul,
You say:
“Fructose is treated by our evolved physiology as a toxin: it is shunted to the liver where it is rapidly disposed of.”
I think this argument has a number of problems:
– I’ve learned from your book that short-chained fats are also shunted to the liver, yet they appear to be highly beneficial
– it might be the case that fructose is a more difficult sugar to process, so it requires specialized machinery to do so — that’s might actually be an advantage, as highly specialized tools can extract benefit and mitigate toxicity quite effectively (consider air and gas in a car, air is allowed everywhere, gas is highly toxic, but it is allowed only in the engine were we rip the benefits without much toxicity)
– even if fructose is toxic in high enough quantities (what isn’t?) that doesn’t automatically make it bad. It is very likely beneficial in moderate amounts given that we evolve such a strong taste for it.
– even if fructose is more reactive, this is mitigated by the body by sending it directly to the liver. In the aggregate, it’s not clear what is worse: higher reactivity but short time in the body vs. lower reactivity but diffused all over the place.
– the low GI of fructose (and the lack of insulin response, a pro-inflammatory hormone) is an advantage;
– fructose appear naturally in fruits, which are the most non-toxic parts of the plants for obvious reasons — why would fructose be such a big exception?
– even in the liver we transform it to glycogen (good), or to saturated fat (again, good).
– based on Dr. Lusting’s presentation, fructose seems to be processed quite similarly to alcohol. these suggests a number of ideas:
– alcohol is also a toxin (a lot more so than fructose I might add) but clearly beneficial in moderate amounts
– we know that alcohol is dangerous in presence of PUFAs, maybe that also holds for fructose
– anecdotally, after a heavy (fatty!) meal, we feel the need for either a desert (sweet) or alcohol. They both seem to help.
I find the fructose-phobia less supported in evidence as other claims in the book. I do think drinking soft drinks, or eating large amounts of sugar/HFCS is clearly bad, but I not so sure that limiting fruits is such a good idea, especially since
(1) we are in the low range of the plateau where I didn’t find any clear evidence that there is any fructose toxicity,
(2) there are clearly beneficial nutrients in fruits that are being thrown out with the bath water
(3) fruits are GOOD, and even without a health benefit, we’d be restricting a very delicious, natural food.
Last, but not least, I think the story with fructose is a lot more complicated than it looks. Subjectively, if I drink a can of soda I often *feel* bad (sugar rush + hypoglycaemia). However, I can eat 6+lb of watermelon at one seating and feel great (a bit bloated, but I can’t blame the melon :)). The difference from eating refined sugar/HFCS and fruits (even in large amounts) is night and day for me.
P.S. For full disclosure, I love fruits 🙂 Despite eating a lot of them, I have experienced problems only a few times from too much fructose, which suggests to me that the plateau for fructose is larger then it is believed in the Paleo community, as long as it comes from fruits.
Hi Dimi,
The difference with short-chain fats is that they provide energy which is exported as ketones. They burn cleanly and the only harm they do is provide an excess of energy.
Fructose, on the other hand, depletes ATP during its disposal. So it doesn’t provide ketones, in fact it impairs ketogenesis.
It’s true that a poison may be OK in small quantities, and this may be the case for fructose. That’s why we’re OK with moderate quantities of fruits, berries, and vegetables.
It’s an interesting idea that fructose might have a special advantage post-meal. Or at least be less bad at that time. I will think about that.
I’m not aware of nutrients in fruit that aren’t also available elsewhere.
It’s really hard to get a large dose of fructose from fruit. Most fruits are around 200 calories per pound; watermelons around 100. Half fructose. So even 6 lb of watermelon is only 300 calories fructose = 45 oz Coca-cola. With much slower digestion, the amount of fructose the liver has to deal with at any one time is much lower. So it’s hard to overdose on watermelon.
I basically agree with most of your points, but it is a question of degree. We tend to suggest limiting fruits and berries to a pound a day.
Hi Dimi and Paul,
I think another thing to maybe consider is the interaction of fructose with pathogens. Fructose is a FODMAP, and apparently many people experience fructose intolerance to some degree. Dr. Emily Deans has blogged about this. So I don’t know about toxicity due to absorbing and processing the fructose, but NOT absorbing it seems to be pretty bad. At least for the depressed, IBS, (anecdotally?) eczema patients.