Jan Kwasniewski developed his Optimal Diet something like 40 years ago and it has become extremely popular in Poland.
Kwasniewski recommended that adults should eat in the ratio
(Source).
In terms of calories this is roughly 240 calories protein / 1640 calories fat / 120 calories carbohydrate on a 2000 calorie diet.
The Perfect Health Diet proportions are more like 300 calories protein / 1300 calories fat / 400 calories carbohydrate. So the diets would be similar if about 300 calories, or 15% of energy, were moved from fat to carbohydrate in the form of glucose/starch (not fructose/sugar!).
Note that we recommend obtaining at least 600 calories per day from protein and carbs combined. This ensures adequate protein for manufacture of glucose and ketones in the liver. But the Optimal Diet prescribes only 360 calories total (less in women), suggesting that gluconeogenesis cannot, over any long-term period, fully make up for the dietary glucose deficiency.
In the book, we note that a healthy body typically utilizes and needs about 600 glucose calories per day. On the Bellevue All-Meat Trial in 1928 Vilhjalmur Stefansson ate 550 protein calories per day, which is probably a good estimate for the minimum intake needed to prevent lean tissue loss on a zero-carb diet.
With only 360 carb plus protein calories per day, the Optimal Diet forces ketosis if lean tissue is to be preserved. Since at most 200 to 300 calories per day of the glucose requirement can be displaced by ketones, the Optimal Diet is living right on the margin of glucose deficiency.
Gastrointestinal Cancers in Optimal Dieters
I learned over on Peter’s blog that Optimal Dieters have been dying of gastrointestinal cancers at a disturbing rate. Recently Adam Jany, president of the OSBO (the Polish Optimal Dieters’ association), died of stomach cancer at 64 after 17 years on the Optimal Diet. Earlier Karol Braniek, another leader of the OSBO, died at 68 from duodenal cancer.
A Polish former Optimal Dieter who has now switched to something closer to the Perfect Health Diet noted that gastrointestinal cancers seem to be common among Optimal Dieters:
The impression we get is that there’s rather high occurrence of gut cancer, including stomach, duodenum, colon … [source]
I want to talk about why I think that is, since the danger that the Optimal Dieters are discovering was one of the key factors leading us to formulate and publish the Perfect Health Diet.
Zero-Carb Diets Can Induce Mucus Deficiency
I ate a high-vegetable but extremely low-carb diet from December 2005 to January 2008. At the time I thought I was getting about 300 carb calories a day, but I now consider this to have been a zero-carb diet, since I don’t believe carb calories are available from most vegetables. Vegetable carbs are mostly consumed by gut bacteria, whose assistance we need to break down vegetable matter, or by intestinal cells which consume glucose during digestion.
Throughout my 2 years on this zero-carb diet, I had dry eyes and dry mouth. My eyes were bloodshot and irritated, and I had to give up wearing contact lenses. Through repeated experiments, I established that two factors contributed to the dry eyes – vitamin C deficiency and glucose deficiency. After I solved the vitamin C issue, I did perhaps 50 experiments over the following few years, increasing carbs which made the dry eyes go away and reducing them which made them immediately come back. This established unequivocally that it was a glucose deficiency alone that caused the dry eyes.
Rebecca reports similar symptoms in herself and her low carb friends.
This is also a well-known symptom during starvation. As a review cited by LynMarie Daye (and referenced by CarbSane in the comments) notes,
Since hepatic glycogen stores are depleted within 24 h of fasting, blood glucose concentrations are maintained thereafter entirely through gluconeogenesis. Gluconeogenesis is mainly dependent on protein breakdown (a small amount comes from the glycerol released during lipolysis) and it thus results in protein wasting. It is the effects of protein malnutrition that lead to the eventual lack of ability to cough properly and keep the airways clear, in turn leading to pneumonia and death during prolonged starvation; hypoglycaemia does not occur. [1]
Another common symptom of very low carb diets is constipation. This is often attributed to lack of fiber, but I am skeptical. I will get to the various possible causes of constipation in a future post, but for now I’ll just point out that a deficiency of gastrointestinal mucus would create a dry colon and cause constipation.
What connects a zero-carb diet to dry eyes, dry mouth, dry airways, and dry gastrointestinal tract?
Tears, saliva, and mucus of the sinuses, airways, and gastrointestinal tract are all comprised substantially of glycoproteins called mucins. Mucins are primarily composed of sugar; they typically have a number of large sugar chains bound to a protein backbone.
For instance, the main mucin of the gastrointestinal tract, MUC2, is composed of a dimerized protein – each protein weighing 600,000 Daltons individually, so 1.2 million Daltons for the pair – plus about 4 million Daltons of sugar, for a total mass of 5 million Daltons. In the mucus, these large molecules become cross-linked to form “enormous net-like covalent polymers.” (source)
If, for whatever reason, mucin production were halted for lack of glucose, we would have no tears, no saliva and no gastrointestinal or airway mucus.
Mucin Deficiency Causes Cancer
There is a strong association between mucus deficiency and gastrointestinal cancers.
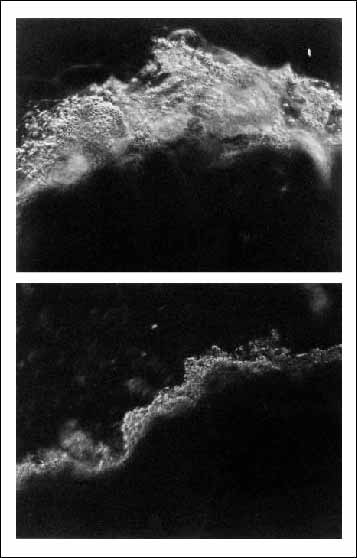
H. pylori is the strongest known risk factor for stomach cancer. [2] H. pylori infection is found in about 80% of gastric cancers. [3] One reason H. pylori promotes stomach cancer so strongly may be that it diminishes mucus in the stomach, as this photo shows:
Top: Normal stomach mucosa. Bottom: Stomach mucosa in an H. pylori infected person.
Scientists have created mice who lack genes for the main digestive tract mucins. These give us direct evidence for the effects on cancer of mucin deficiency.
Experiments in Muc1 knockout mice and mice with Muc1 knockdown have shown that under Helicobacter infection, mice deficient in Muc1 develop far more cancer-promoting inflammation than normal mice. [4]
The main mucin of the intestine is Muc2. The group of Leonard Augenlicht of the Albert Einstein Cancer Center in New York has studied mice lacking Muc2. They develop colorectal cancer. [5]
Tracing backward one step toward the source of mucin deficiency, the sugars in mucin are built from smaller pieces called O-glycans. It has been shown that mice that are deficient in O-glycans are prone to colorectal cancer: “C3GnT-deficient mice displayed a discrete, colon-specific reduction in Muc2 protein and increased permeability of the intestinal barrier. Moreover, these mice were highly susceptible to experimental triggers of colitis and colorectal adenocarcinoma.” [6]
Nutrient Deficiencies Can Also Play a Role
Some micronutrients are required for mucin production – notably vitamin D. [7, 8] Poland is fairly far north, and many of the Optimal Dieters could have been low in vitamin D.
Other important micronutrients for cancer prevention are iodine and selenium. Poland in particular had the lowest iodine intake and among the highest stomach cancer death rates in Europe. After Poland in 1996 began a program of mandatory iodine prophylaxis, stomach cancer rates fell:
In Krakow the standardized incidence ratio of stomach cancer for men decreased from 19.1 per 100,000 to 15.7 per 100,000, and for women from 8.3 per 100,000 to 5.9 per 100,000 in the years 1992-2004. A significant decline of average rate of decrease was observed in men and women (2.3% and 4.0% per year respectively). [9]
So among the Polish Optimal Dieters, the elevated gastrointestinal cancer risk caused by mucin deficiency may have been aggravated by iodine and sunlight deficiencies.
Conclusion
A healthy diet should be robust to faults. The Optimal Diet is not robust to glucose deficiency.
There’s good reason to suspect that at least some of the Optimal Dieters developed mucin deficiencies as a result of the body’s effort to conserve glucose and protein. This would have substantially elevated risk of gastrointestinal cancers. Thus, it’s not a great surprise that many Optimal Dieters have been coming down with GI cancers after 15-20 years on the diet.
We recommend a carb plus protein intake of at least 600 calories per day to avoid possible glucose deficiency. It’s plausible that a zero-carb diet that included at least 600 calories per day protein for gluconeogenesis would not elevate gastrointestinal cancer risks as much as the Optimal Diet. But why be the guinea pig who tests this idea? Your body needs some glucose, and it’s surely less stressful on the body to supply some glucose, rather than forcing the body to manufacture glucose from protein.
Fasting and low-carb ketogenic diets are therapeutic for various conditions. But anyone on a fast or ketogenic diet should carefully monitor eyes and mouth for signs of decreased saliva or tear production. If there is a sign of dry eyes or dry mouth, the fast should be interrupted to eat some glucose/starch. Rice is a good source. The concern is not only cancer in 15 years; a healthy mucosal barrier is also essential to protect the gut and airways against pathogens.
Related Posts
Other posts in this series:
- Dangers of Zero-Carb Diets, I: Can There Be a Carbohydrate Deficiency? Nov 10, 2010.
- Danger of Zero-Carb Diets III: Scurvy Nov 20, 2010.
- Dangers of Zero-Carb Diets, IV: Kidney Stones Nov 23, 2010.
References
[1] Sonksen P, Sonksen J. Insulin: understanding its action in health and disease. Br J Anaesth. 2000 Jul;85(1):69-79. http://pmid.us/10927996.
[2] Peek RM Jr, Crabtree JE. Helicobacter infection and gastric neoplasia. J Pathol. 2006 Jan;208(2):233-48. http://pmid.us/16362989.
[3] Bornschein J et al. H. pylori Infection Is a Key Risk Factor for Proximal Gastric Cancer. Dig Dis Sci. 2010 Jul 29. [Epub ahead of print] http://pmid.us/20668939.
[4] Guang W et al. Muc1 cell surface mucin attenuates epithelial inflammation in response to a common mucosal pathogen. J Biol Chem. 2010 Jul 2;285(27):20547-57. http://pmid.us/20430889.
[5] Velcich A et al. Colorectal cancer in mice genetically deficient in the mucin Muc2. Science. 2002 Mar 1;295(5560):1726-9. http://pmid.us/11872843.
[6] An G et al. Increased susceptibility to colitis and colorectal tumors in mice lacking core 3-derived O-glycans. J Exp Med. 2007 Jun 11;204(6):1417-29. http://pmid.us/17517967.
[7] Paz HB et al. The role of calcium in mucin packaging within goblet cells. Exp Eye Res. 2003 Jul;77(1):69-75. http://pmid.us/12823989.
[8] Schmidt DR, Mangelsdorf DJ. Nuclear receptors of the enteric tract: guarding the frontier. Nutr Rev. 2008 Oct;66(10 Suppl 2):S88-97. http://pmid.us/18844851.
[9] Go?kowski F et al. Iodine prophylaxis–the protective factor against stomach cancer in iodine deficient areas. Eur J Nutr. 2007 Aug;46(5):251-6. http://pmid.us/17497074.











Hi Shane,
Thanks! That’s more detail than I’ve gotten elsewhere.
I still find the physiological basis for some of those recommendations to be obscure.
Personally, I don’t see anything wrong with ketosis per se, but I guess he’s using it as a proxy for carb+protein deficiency, and wants people to raise carbs high enough to eliminate the deficiency condition. That’s prudent since his numbers seem to be right on the edge of deficiency, without such guidance many people would have difficulty.
I agree with the preference for starches.
Well, it makes some sense. Thanks for the info.
Best, Paul
Drs. Jaminet,
I could have missed this, as I’ve just recently encountered your site and dietary observation & adherences to which you are inclined. I am, and have
been notably so inclined for the past 9 years, although admittedly, not so compliant…notably more so over the past few years.
The “missed” issue refers specifically to the omission of focus on the individual…and, again, please forgive
my ignorance if somewhere there is a good deal of address to this issue. To liken all human beings as having relatively identical functioning metabolisms seems to ignore the various races, and even more specifically, regional/tribal differentiations in physiologic predispositions to any particular diet, and
the same would perhaps apply to the varying human responses to supplemented vitamins, minerals and nutriceuticals. The remarkable work of Dr. Weston A. Price seems to have established the relevant individual-specific issues of optimizing diet/food as primary medicine for over-all health balancing.
Not being a health practitioner, I do not get to witness the multitudes of people’s reactions to dietary adherences, but only by review/independent research, which, certainly is limiting. However, there is the notable work of Dr. Nicholas Gonzalez, MD, (preceded by William Kelley, DDS) who works most often with cancer patients…and pancreatic cancer, at that, with exceptional results (unless one believes the many detractors he has coming from the allopathic ranks–including members of BigPharma with vested and markedly conflicting interests). Dr. Gonzalez utilizes whatever version he does for an approach of metabolic-typing of each patient to determine/optimize diets which are intended to largely reverse the toxic and burdensome insult which ill-suited diets are prone to
manifesting…along with, of course, many chronic illnesses. Dr. Mercola also preaches this, yet (to me)
curiously also comes to generalized conclusion in such passionate manner, about eating, say, a low-carb diet, when perhaps, and individual’s metabolic/nutritional type inclines them–like Dr. Price’s global review–more to such a diet. From Northern Indian/Eskimo’s to Incan-Aztec-Mayan, to Africans,notably Masai, to Polynesian, Asian, SE Asian, S.Asian, Europeans, Mid-Easterners…there is such possible variation, due to the mixing of races and regional peoples (and I’ve not nearly named the gambit), each which initially remained relatively genetically undiluted, and for significant periods of time. When referring to V. Steffanson’s ground-breaking dietary experiment in 1928 (of which I’ve been influenced by for years), after his life amongst Inuit–and exclusively consuming their diet for years with such healthy results, I yet am continuously left wondering how such experiment would work itself out with a large and broad array of genetically-differing types/mixes.
So I ask if or how much you take pause to consider the
individual, and the genetic dynamics of each body’s metabolic-nutritional type (I believe nutrigenomics is
onr newly-coined term, here). Do you consider everyone throughout the world so statically inclined as to dietary requirements? My life-experiences have taught me to consider spectral relationships, and I simply can’t imagine how this wouldn’t apply to dietary preferences and optimization amongst the generally varied metabolic-nutritional types, just, again, as Dr. Mercola, along with others have been quite keen to point out–and ostensibly, for worthwhile consideration and practice.
Additionally, I am aware that you, unlike, say Dr. Rosedale, do advocate relaxing of restricted-carb intake, with the appearance of symptoms (dry mouth, eyes…which indicate mucus-production deficiency related to dietary glucose)–a most astute and responsive observation, caution, and advise of.
I further, grapple with the notion that any given indi-
vidual, after, say, even 15 years–and certainly 40-70
years–can so entirely be able to change their dietary
“spots” so efficiently, in each and every case, anyway,
as to evidence entirely effective solutions for the
health disorders which their otherwise poor dietary habits contributed to…especially without, at least, creating yet another dilemma. A bit too optimistic, perhaps? This is not referencing the rather normal
resistance to dramatic dietary shift, whereby the perception of “lack” and other–perhaps either worth-
while or false–cravings occur, wherein compliance, and thus results are significantly impaired.
I also ask that you kindly forgive what might be interpreted as any manner of assault or insult to your
admirable work to date in this field. Would it were
that I had such a scientific background, along with such keenly impassioned and dedicated focus on helping
others. It is rather, that I am, of bias, no doubt, trying to see if there is not good reason to temper the
absolutes which so many find in a particular theory which is inclined towards such metabolically restrictive approaches, ie, carbs and grains are no good for everyone. I do find–and feel–that they’re not very good for me, incidentally. I have had several bouts of cancers, and from the conventional therapies of Cut-Poison-Burn (no burning, only 15 or more CT & PET scans..way more than acceptably safe rad-exposure, I’m convinced), have also sustained numerous other surgeries/insults…I have severe GERD, along with a gall-bladder removal (also spleen), so I really have my hands full trying to find suitable dietary direction so as to best optimize–for my (perhaps imagined?) nutrigenomically-inclined type. Having had
lymphoma as the last bout of cancer, I do fit Dr. Gonzalez’s categorization of a parasympathetic- dominant type…and flesh and high fats seems to suit me quite well…except for digestive complications, which are, as mentioned, complicating and confounding.
I am fond of and consume raw dairy of all sorts, but,
alas, the ever encroaching mania of the FDA with regards food just took yet another swipe at taking such
raw dairy availability of the table–literaly–here in Calif…more of the same looms everywhere, woefully, as I’m certain you are quite aware, having just participated at the Wise Traditions Conference this year. I made it to last year’s…not this recent one,
unfortunately.
Hi Mark,
Briefly:
1) There is no difference among humans in the nutrient needs of our bodies ex the digestive tract;
2) There are some variations in the digestive tract among human populations and this makes for slight variations in optimal carb and fiber intake;
3) However, bigger variations in optimal diet occur in disease states. A big part of our blog is devoted to discussing how diet interacts with disease, and how diet can be used to diagnose and treat diseases.
Hope that helps!
Hi Paul, loved the book by the way. Your comment on hydraulic pressure caught my attention as it reminded me of Thomas Cowans book The Fourfold Paths to Healing where he quoted Steiner’s theory that the heart is not a pump, rather a listener and that most of the power of the cardiovascular system comes from the colloidal osmotic pressure? and that pressure is increased when there is more fat in the diet than any other macronutrient. I noticed you didnt elaborate on the subject and was interested if you were familiar with Steiner’s theory and that concept that dietary fat can increase the osmotic pressure, providing the pumping mechanism for the heart.
thanks, james ardagna, exercise physiologist.
Hi James,
No, I’m afraid I’m not familiar with Steiner’s theory.
Keen mention from James Ardagna…
I have met with and heard Dr. Cowan present…I believe he was at this past Price Foundation “Wise Traditions” in Dallas…and moreover have read his presentation of Steiner’s remarkable and seemingly alternative understanding as to the function of the heart relevant to blood flow throughout the body. It does not seem, indeed, at all possible that the beating of the heart could function as a pump capable of moving all that blood through all that much vascular ducting–especially the uphill part. The reason that fat…saturated fat at that…is of such import to the requisite “osmotic pressure” input–so as to “drive” the complex, vortexed flow of blood–is that it has the most readily available hydrogen to donate…for the increased production/provision of H2O, which in turn creates the requisite “osmotic pressure” without which the entire circulatory system
would not function. The heart has enough work to constantly perform just “squeezing” or opening on unending cue.
Hence, Steiner somehow, not being formally schooled in cardiovascular research, managed to issue, without reservation, that “the heart is not a pump”. Which Tom
Cowan and others–being puzzled at first–set out to
discover the real meaning of this controversial statement. It seems that he/they have done just that.
So one solution to coronary dysfunctions is to consume saturated fats, and not avoid them…just make sure to source from healthy/suitable products, as in quality virgin coconut oil, and pastured dairy and animal fat,
nuts/seeds (for those that approve and can tolerate),
wild caught fish/shellfish, and even virgin palm oil,
where possible to obtain. And toss in avocados and
olive oil, ‘though they’re more in the mono-unsaturated
fat realm.
Thanks for the input Mark, as I feel there is very little on the subject and talking about such a thing one feels one is committing heresy to say the least!
Agreed, James, that there is no dirth of studies on
subject: “the heart is not a pump”. Healthy fat/oil
consumption–particularly saturated–are generally recognized on this remarkable site as asset for improving/maintaining healthy cardio-functions, and
perhaps more study of this hydrogen donation for H2O
production–to osmotically provide the pressure to help drive blood circulation–can be undertaken.
If one knows of Dr. Tom Cowan and his success in treating cardio issues of his patients for over 2
decades, such a new concept might be easier to
consider, further discuss, while not seeming too far off into wild nor foolish speculation.
The best our comments can do is to lead to sound, healthy, dietary approaches; sharing/exchange of (hopefully) sincere & sufficiently informed dietary-
health wisdom to help each of us learn how to best
select foods which we enjoy, along with fueling our bodies to optimal extents of preventing and turning about disorders which, apparently, most of our current conventional “wisdom” has been failing to provide us with. So much new to be learned, and implemented.
Certainly much tinkering and blunders as well–all a
part of normal pioneering effort.
Pardon my enthusiasm with a subject that might be
better placed in another category…or not; with
the appreciation of being able to absorb and share
so much beneficial health-diet info, Paul…Thank You.
The Optimum Diet favours pork, and may not exclude accohol(?); but Nanji and Bridges identified possible problems with pork plus moderate alcohol in 1985 and other researchers have confirmed the pattern since.
Hi Dr Jaminet,
You often state that Calories(protein) + Calories(starch) >= 600 Calories based on the bodies need for glucose.
Since it seems that the consumption of coconut oil can result in an increase in ketone bodies available for fuel, perhaps reducing the need for glucose, can the equation be modified to be Calories(protein) + Calories(starch) + X*Calories(coconut oil) >= 600 Calories? If so what do you think the factor X would be?
Hi Scott,
Yes, it could. However, the value of X is fairly small and highly uncertain, and I think it’s prudent to treat it as zero. You can still generate adequate ketones to heal neurological disorders with 200 carb calories and 400 protein calories per day, so it doesn’t seem necessary to reduce intake further.
Agreed; in fact normal everyday ketone level is about 1/4 that seen in low-carb ketosis, so there is a sliding scale; a mild elevation of ketones over a lifetime (say a doubling of output) is probably better than (or at least as good as) periodic Atkins induction levels, with ketone overspill, if ketone benefits rather than weightloss is the goal.
hi paul, have been recommending your book to my clients (exercise physiologist) with success! was just wondering about puffy bags under the eyes – could it be indicative of a deficiency of some sort, a chronic infection or an inflammatory response? am following the diet and feel great:
take brazil nuts for selenium and kelp tablets for iodine
vitamin c tablets
bovine adrenal gland/liver for copper
raw milk for fat solubles, vitamin k
palm oil
coconut oil in copious amounts (can eat spoonfuls without side effects)
raw organic cream
safe starches
sauerkraut for digestion, vitamin c
3 eggs a day, fish, meat, etc
himalayan salt in good amounts
fermented cod liver oil/high vitamin butter oil (no fish oil)
as I said have lots of energy, am strong (strength training) don’t have dry eyes or mouth any ideas as to the baggy eyes which i’ve had for years?
thanks, james.
Hi James,
I don’t know what causes the baggy eyes, I suspect there are many causes, but one thing I would work on is extracellular matrix precursors, such as: vitamin C; sulfur/MSM; collagen eg from bone broth soups; adequate carbs. That should help both skin and vessels keep their integrity.
Baggy eyes – I have the same problem, but in my case it’s hereditary; I was born with them and I could be my dad’s twin. And they’re getting worse as I get older.
But those suggestions are good to know, Paul, thanks! Definitely worth trying. I don’t have time for the bone broth soups, unfortunately, but may try the collagen supplements from the Supplement Recs page.
James: let us know if you see signs of improvement!
thanks Connie will let you know of any progress. Yes my dad also has baggy eyes so i guess there is a hereditary component – it would be interesting to see if this could be overcome (the hereditary component) through experimentation of supplementation. will get onto the collagen as i feel i probably get enough sulfur from eggs (two dozen a week) and do bone broths (mainly fish and chicken though).
james.
Baggy eyes are caused by the loss of minerals (the balance between sodium and potassium is altered). Gary Taubes suggests supplementing with salt, in his book ”
Why we get fat”.
Hello, you commented that one of the indicators of infection by eukaryotes, protozoo, parasites and candida is a worsening of disease symptoms. Since most people I know are accustomed to a diet high in sugar and carbohydrates, it is normal the first few days of changing to a ketogenic diet causes symptoms such as headache, mild hypoglycemia … until the body adapts, how long is normal adaptation time to see if the symptoms are due to infection or metabolic adaptation? (sorry for my bad english).
Thanks.
Hi Luisa,
As you say, you can’t really judge in a few days. The best way would be to try switching on and off between, say, a ketogenic low-carb diet (10% carbs + coconut oil) and a 30% carb diet, 3-4 weeks on one, 3-4 weeks on the other, and see if you consistently feel better on one or the other. Three cycles = ~6 months should give a reasonable amount of data.
I feel like when I have less than 240 grams of carbs a day, I get glucose deficiency. My mouth gets very dry. If I wait too long to eat some starch my heart rate and blood pressure go up. Maybe I can reduce carbs more gradually. I think advising people to put up with the ‘low carb flu’, puts them in an unhealthy state.
If the human body is designed for anything, it is designed to function without food. We wouldn’t any of us be here if humans needed to eat carbs, or anything else, every day, and if missing a meal, or part of one, made us unhealthy.
If you’ve ever withdrawn off heroin, you’ll know that flu-like sensations are not always an accurate guide to what is or is not harmful.
I found myself that going on an “all-meat” bender, sausages and eggs and steak and cream and not much else, was a way to reduce crabs without noticing the difficult stages of ketogenisis.
I also think that taking time, and many attempts, to lower carbs is a good way of adapting the body to it.
Whether this is actually necessary is unknowable.
The trouble with counting crabs is, they know when you’re looking, and pop back in their holes before you can get an accurate number.
Dear Doc Jaminet, I’ve supposed that adrenal fatigue can drive to glucose deficiency in ectomorph guys.
So ectomorph, who usually use adrenal to raise up his blood glucose, after has eaten lot of cabs (it seems that ectomorph have very insulin resistance, cause lots carbohydrate are eaten), so can this drive him to adrenal fatigue? I suppose lots of carbs having high IG, create a stress, cause Cortisolo needs to make glycemia constant in so little time.
I mean, that this guys, doesn’t usually gain weight, and in fact usually they have low glycemia , cause their ractive hypoglycemia, cause thay have not much muscular mass and adipocytes.
Now if a ectomorph don’t eat carboydrate can make his adenal fatigue worse and this can cause severe intestinal problems?
Thanks for your answer, good job Doc Jaminet!!
Hi Salvio,
I think our diet is a pretty good fix for those issues. Try eating in accord with our food plate, http://perfecthealthdiet.com/?page_id=8, for a while.
You want moderate carbohydrate intake, 20-30% of calories is a good range I believe.
Oh yeah, firstly, thanks for your answer.
But I noticed that when I’m under terrible stress, I feel I need more carbohydrates than I usually use.
Tell a thing. But if I eat fructose, and I burned all amount I’ve eaten in a day, can fructose help me to avoid ketosis?
Glucose load especially muscles and liver if the amount is very high. But if glycemic load is high liver takes glucose to release it later in fast time. Now if I use less carb than I need but I use fructose, maybe I’d like to balance sugar for enter body (from liver by fructose) and sugar for muscular use(glucose).
So for this reason, can fructose avoid or retard ketosis insted use glucose???
If this is true, fructose is like to be a potent anticatabolic carboydrate.
Liver can distribuite glucose in all part of body, muscles don’t, so a little part of fructose should retard ketosis, or this isn’t correct?
What do you think about???
Fructose does retard ketosis but I don’t see what ketosis has to do with your issues. Ketones are not intrinsically catabolic. How much carbs do you normally eat?
Because I’m sure that Ketosis is a natural catabolic Human state, because GH help to retain proteins, but I’m sure that Ectomoph can go into Ketoacidosis state.
Ectomorph usually eats a lot of carbs because he has problems with adrenal fatigue, but I suppose this create insulin resistance, so if ectomorph doesn’t suddenly eat carbs, he has too little insulin and too much resistance, that means that ectomorph just using about 100 grams of carbs can go in ketoacidosis.
There is a problem about the word “catabolic”. Lot of people think that catabolic means “loss of proteins”, but catabolic means “destroy energetic substrate to create energy”, now ketosis is anticatabolic proteine state in a catabolic energetic state. I mean I know the difference between them.
But I’d like to know, if can ectomorph retard ketosis (at the beggining of diet) in order to let his body to raise his insulin sensibility and in this way avoid ketoacidosis?
I usually eat about 100 grams of carbs, and I recharge at Sunday with 200 grams, otherwise I feel to tired in the week.
I noticed that, if I eat less Monday there’s no problem, probably my insulin levels drop because reduce my cals intake.
Anyway I eat only 50-75 carbs on Monday, other days I eat about 100 grams, and on sunday I eat about 200 grams.
I know I ask strange things but I’m curious to know why people who are mesomorphes and endomorphes can switch easily in your diet and in other low-carb diet (like paleo diet) and ectomorphes have terrible trouble to do that.
Thanks a lot!!!
First I just want to say that I absolutely love the PHD. Thanks!
As far as criticisms of Kwasniewski goes, I think there are many factors other than carbohydrate restriction that are not being taken into account when assessing why patients who followed his protocols are getting sick
Wheat flour is used in the recipes for that diet.
Also, I seem to recall there is no discussion of pastured-pork, grass-fed beef or organic vegetables on his site or in the stuff I have read. So, quality of food is not considered either.
We also do not know what the environmental issues in Poland are.
Just a few thoughts.
Thanks for your very fine work!
Thanks Michael!
Look at this Paul: insulin stimulates gut barrier via lipogenesis;
http://www.cell.com/cell-host-microbe/retrieve/pii/S1931312812000315
Highlights
•Deficiency in intestinal fatty acid synthase (FAS) results in intestinal inflammation
•FAS-deficient mice have a disrupted intestinal mucus barrier
•FAS is required for S-palmitoylation-dependent secretion of Mucin 2
Summary
The intestinal mucus barrier prevents pathogen invasion and maintains host-microbiota homeostasis. We show that fatty acid synthase (FAS), an insulin-responsive enzyme essential for de novo lipogenesis, helps maintain the mucus barrier by regulating Mucin 2, the dominant mucin in the colon and a central component of mucus. Inducible Cre recombinase-directed inactivation of the FAS gene in the colonic epithelium of mice is associated with disruptions in the intestinal mucus barrier as well as increased intestinal permeability, colitis, systemic inflammation, and changes in gut microbial ecology. FAS deficiency blocked the generation of palmitoylated Mucin 2, which must be S-palmitoylated at its N terminus for proper secretion and function. Furthermore, a diabetic mouse model exhibited lower FAS levels and a decreased mucus layer, which could be restored with insulin treatment. Thus, the role of FAS in maintaining intestinal barrier function may explain the pathogenesis of intestinal inflammation in diabetes and other disorders.
Great find George! Maybe I’ll squeeze a mention into the book. If so I’ll give you a hat tip.
And insulin can be generated in the gut:
Generation of functional insulin-producing cells in the gut by Foxo1 ablation
Chutima Talchai1–3, Shouhong Xuan4, Tadahiro Kitamura5, Ronald A DePinho6 & Domenico Accili1,2
Restoration of regulated insulin secretion is the ultimate goal of therapy for type 1 diabetes. Here, we show that, unexpectedly, somatic ablation of Foxo1 in Neurog3+ enteroendocrine progenitor cells gives rise to gut insulin-positive (Ins+) cells that express markers of mature b cells and secrete bioactive insulin as well as C-peptide in response to glucose and sulfonylureas. Lineage tracing experiments showed that gut Ins+ cells arise cell autonomously from Foxo1-deficient cells. Inducible Foxo1 ablation in adult mice also resulted in the generation of gut Ins+ cells. Following ablation by the b-cell toxin streptozotocin, gut Ins+ cells regenerate and produce insulin, reversing hyperglycemia in mice. The data indicate that Neurog3+ enteroendocrine progenitors require active Foxo1 to prevent differentiation into Ins+ cells. Foxo1 ablation in gut epithelium may provide an approach to restore insulin production in type 1 diabetes.
Fox01 in diabetes:
http://www.sciencecodex.com/fox01_the_molecular_link_between_insulin_resistance_and_inflammation
Thanks are due to my friends Silvia, Glenn and Elizabeth for these links.
“Suppression of FoxO1 activity by MEDICA analogs may partly account for their antidiabetic anti-inflammatory efficacy. FoxO1 suppression by LCFA analogs may provide a molecular rational for the beneficial efficacy of carbohydrate-restricted ketogenic diets in treating diabetes. ”
http://diabetes.diabetesjournals.org/content/60/7/1872.full
There are some researches showing the opposite – high mucus secretion is connected with cancer.
http://www.news.harvard.edu/gazette/2004/04.29/01-mucus.html
http://phys.org/news/2011-03-mucus-barrier-unveils-cancer-cell.html
Mucus may protect the cancer cells and tumors from medicines and the actions of the immune system.
Mucus is dangerous in that case, cause infiammatory state is the problem not mucus. Anyway you can use salt o other strong ionic salts that cause decreasing Van Der Walls interaction between mucopolysaccarides and dissolve
them.
It’s the same tenants used by NAC when someone catch a cold to dissolved mucus.
Otherwise the mucus deficiency is really dangerous cause bacteria and yeasts attack the tissutes directly with no protection.
I’ve question to Paul. Can I use some wood ashes in my rice? I know they are rich in minerals like Potassium, Calcium and Magnesium, so I was wondering to myself if I can use it to get more minerals in my diet.
Futhemore I read that amylose can be got in amorphous state, simply cooling everything quickly, can I eat cold rice but cooled quickly to digest it easly without raising up my glycemia fast?
Thanks.
Hi Salvio,
I don’t know about wood ash. Charcoal is eaten as a detox agent but it can easily induce lipid deficiencies and potentially other nutritional deficiencies. In general burning organic materials generates toxins / carcinogens. It seems to me food would be a safer source of nutrition.
Cooling rice in a refrigerator after cooking does generate some resistant starch which is healthful. The rice still has a high glycemic index however, you should still follow the advice in this post to mix it with acids and fat and vegetables: http://perfecthealthdiet.com/2011/10/how-to-minimize-hyperglycemic-toxicity/
RE: Low carb and dry eyes.
I read this with interest and added potatoes or white rice each day to see if I could help both my dry eyes and my weight gain. I also took 3 x 500 mg Vit C per day. The results? My eyes got far worse, and within a week I had gained 6 pounds. I couldn’t take any more, so I dumped the ‘safe’ starches.
My body is insulin resistant and my liver makes glucose like no ones business from almost anything, so I highly doubt I am glucose deficient. Certainly my blood glucose tests don’t suggest a deficiency. I don’t think everyone needs glucose (starches) in their diets.
Hi Beedee,
Sounds like you are diabetic. I would look into gut flora. Stool tests for DNA from pathogens may turn up something helpful to you.
Best, Paul
Hi there, i have recently been on a low carb diet and have experienced very dry eyes (i could not wear contacts) and also a very dry mouth. The saliva was watery and lacked mucus. A contributing factor in my case was the presence of high risk papillomavirus which effects all mucus membranes of the body including the mouth and eyes. Although not widely recognized, it is a primary cause of red, dry eyes. There are other viruses and pathogens with similar effects but hpv is the most common and least understood. Dry mouth can also cause an increase in dental caries.
Brilliant write up, I have experienced this mucus dry up and its definitely noticeable, trying to avoid this by having just enough carbs to avoid this and at the same time I fast a lot!
Here is another more article that agrees that carbs are important for building a healthy gut mucus layer: http://syontix.com/the-importance-of-the-gastrointestinal-mucus-layer/
Hi there,
Thank you for addressing this topic! I’m curious to know your thoughts on why one might be experiencing dry eyes (noticeably red), yet still has excess nasal and oral mucous. I have recently added more safe starches into the mix, as I think I was too low for too long, but haven’t noticed an improvement. I stick to real food, mycotoxin-free coffee in the AM, water throughout the day.
I’d love to clear this up, and any suggestions would be much appreciated!
Hi Jessica,
There are innumerable reasons for dry eyes besides being on a low carb diet. Unfortunately very little research has been completed on the causes for dry/red eyes which is unfortunate because it is extremely common.
I believe the most common cause of red eyes in the general population results from being exposed to certain viruses, particularly the human papillomavirus group, which is also extremely common.
Some researchers believe that pathogens can induce an immune response in which the immune system attacks specific cells in the body, the exocrine glands which produce tears, saliva and mucous in other areas of the body. (http://en.wikipedia.org/wiki/Sj%C3%B6gren's_syndrome).
In terms of your dry eyes without nasal or oral mucous, try to increase carbs and see what happens. Try to avoid constipation. If no improvement go and see an ophthalmologist.
On a side note, a recent report shows yet again that high protein is linked to increased cancer:
http://www.theguardian.com/science/2014/mar/04/animal-protein-diets-smoking-meat-eggs-dairy
You may have to consider allergies with your symptoms.
Justin
Paul has debunked that protein study on this very blog. http://perfecthealthdiet.com/2014/03/case-killer-protein/