If there will be a general theme to our second year of blogging, it will be chronic infections – how they interact with the body to promote disease, and how we can use diet-related techniques to successfully combat them.
Blood lipids, such as LDL and HDL cholesterol, provide a fascinating window into health. We’ve already discussed both LDL and HDL (Low Carb Paleo, and LDL is Soaring – Help!, March 2, 2011; Answer Day: What Causes High LDL on Low-Carb Paleo?, March 3, 2011; HDL and Immunity, April 12, 2011; HDL: Higher is Good, But is Highest Best?, April 14, 2011; How to Raise HDL, April 20, 2011), but there’s quite a bit more to be said.
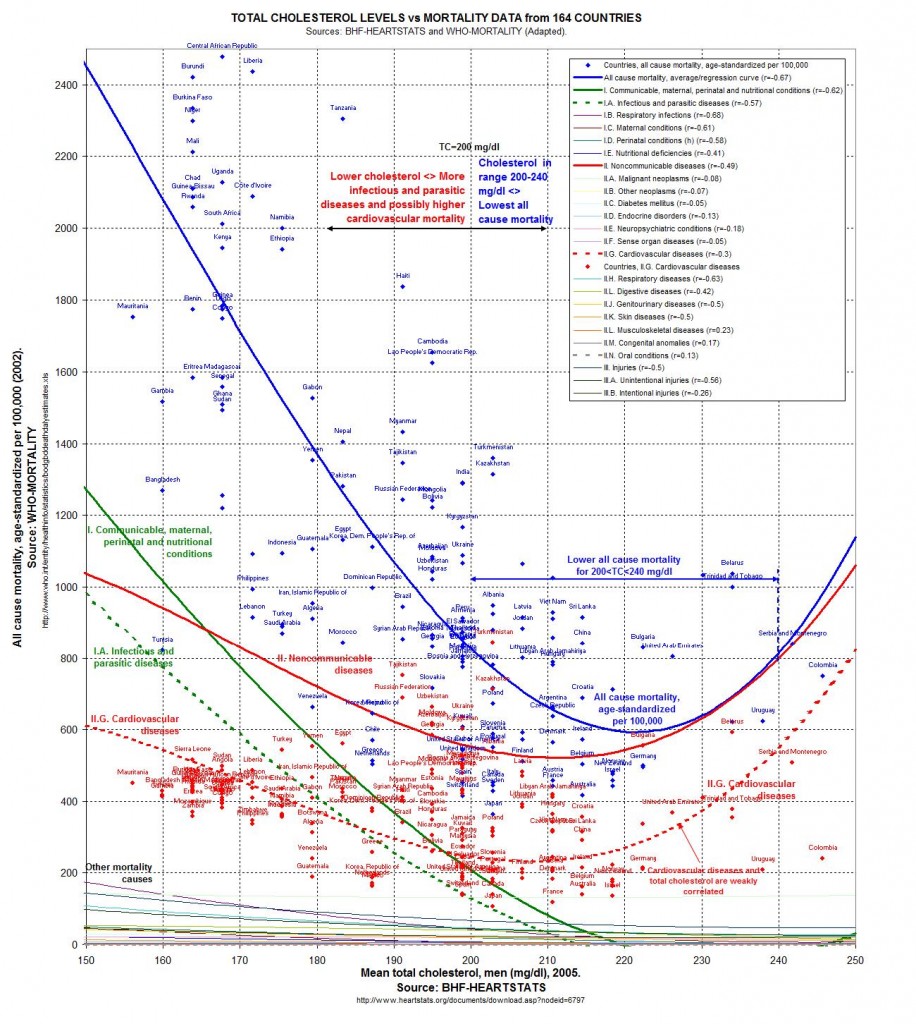
The extraordinary Portuguese blogger Ricardo Carvalho, better known as O Primitivo, of Canibais e Reis did some great work a few years back assembling World Health Organization statistics into an Excel database. One of the fruits of this labor was that he was able to correlate disease rates against serum cholesterol levels for all the countries in the database. His post about that is here and he created a great graphical representation of the results which I’ve reproduced here (click to enlarge):
There’s a lot of interesting information in this graph.
On the upper right are some correlation coefficients between serum cholesterol and disease incidence. Most diseases are either uncorrelated with cholesterol, or negatively correlated, meaning that mortality goes up as cholesterol goes down.
Minimum mortality is found in countries with average cholesterol between 200 and 240 mg/dl. Mortality rises sharply as cholesterol levels fall below 200 mg/dl.
No ecological fallacy
When aggregating over populations, it’s possible to get misleading results – an outcome called the “ecological fallacy”. However, I think this relationship is pretty solid.
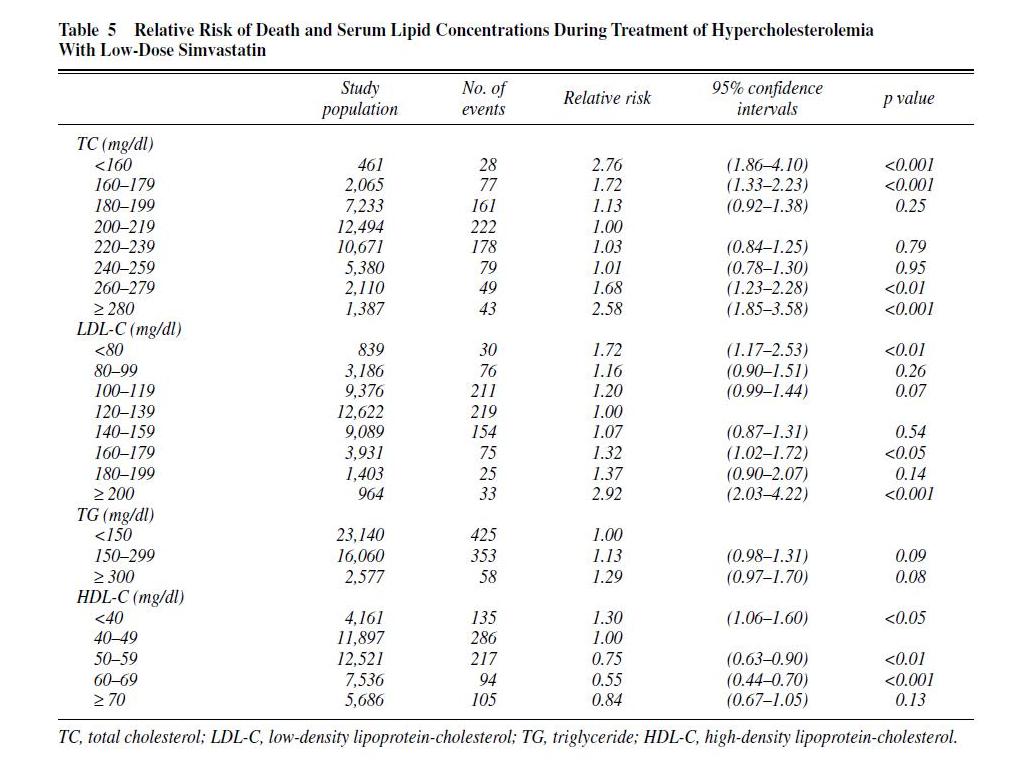
It’s been confirmed in individuals in clinical trials. For instance, in the Japan Lipid Intervention Trial, here was the table of mortality as a function of serum lipids:
You’ll note that the “relative risk” of dying was lowest for TC between 180 and 260, LDL-C between 80 and 160, and HDL-C between 60 and 70.
The minimum mortality region of O Primitivo’s national samples falls right in the middle of the JLIT minimum mortality region.
Infectious disease mortality depends strongly on cholesterol levels
By far the strongest dependence of mortality on cholesterol levels is found for infectious diseases. Infectious disease mortality is shown by the dashed green curve.
Infectious disease mortality approaches zero where TC averages between 215 and 245 mg/dl. It rises very sharply as TC falls. Over a wide range of TC, for every 10 mg/dl drop in average TC, mortality rises by 200 infectious deaths per year per 100,000 population.
Other diseases are partly infectious in origin
As regular readers know, I believe that many other “noncommunicable” diseases are actually caused in part by chronic infections. Cardiovascular disease is one – atherosclerotic lesions are universally found to be infected, macrophages usually need to be infected in order to become “foam cells” which contribute to atherosclerotic plaque formation, and the infectious burden in lesions drives the risk of fragmentation of plaque into the clots which cause heart attacks and strokes.
If cardiovascular disease is partly due to infections, and the protective effect of cholesterol against infections is present here, then we should expect cardiovascular disease mortality (shown in the red dashed line) to rise as TC falls.
It does. Mortality from cardiovascular disease starts rising as TC falls below 205 mg/dl and rises by about 200 infectious deaths per year per 100,000 population for every 25 mg/dl drop in average TC.
Causality probably runs in both directions
We can’t directly infer causality from these statistics. Consider two possible directions of causality:
- Serum cholesterol – LDL and HDL – help defend against infections. As long as you have these infection-fighting lipids in your blood, infections can’t kill you.
- Infections destroy LDL and HDL, and the more severe the infection, the lower blood cholesterol goes. By the time the infection is severe enough to kill you, TC is very low. So countries with high infectious burden have both low TC and high infectious mortality.
The first line of causality is certainly true. I’ve already discussed the important infection-fighting properties of HDL – in fact I’ve argued that infection fighting, not cholesterol transport, is the primary function of HDL (See HDL and Immunity, April 12, 2011). As I’ll discuss, LDL also has immune functions.
The second line of causality is also quite likely. Pathogens evolve ways to suppress immunity; that is what makes them effective pathogens. If LDL and HDL are crucial for immune defense, then pathogens will have found ways to destroy or damage them.
In this series I would like to explore these interactions between blood lipids and infections a little more deeply. They may lead us to ways we can tweak our diet to improve our defenses against disease — or help doctors recognize under what circumstances taking statins will raise, not lower, cardiovascular disease risk.
References
[1] Matsuzaki M et al. Large scale cohort study of the relationship between serum cholesterol concentration and coronary events with low-dose simvastatin therapy in Japanese patients with hypercholesterolemia. Circ J. 2002 Dec;66(12):1087-95. http://pmid.us/12499611.











I’ve been a fan of a healthy(not low!) cholesterol level as you know – what of the reports of hunter gatherers having low cholesterol. Is it the product of fringe environments, or low infectious burden, or what?
Minor issues . . .
I think (hope?) you meant ‘mortality’ in the following: ‘Morality rises sharply as cholesterol levels fall . . ‘
The search function appears not be working.
Feel free to delete this comment.
Thanks, RK, the typo is fixed. I’m not sure why the search widget stopped working. Will look into that later.
Emily, I’m not sure what to make of that. I have to look into the provenance of that data. You know Kitavans have much higher cholesterol, TC over 200. They live Paleo style, so clearly not all Paleo environments produce low cholesterol levels.
Paul,
I have Staffan Lindeberg’s book “Food and Western Disease”. He talks about the Kitavan’s higher cholesterol levels and explains that it is due to their use of coconut in their diet.
Hi Rob, after this post I did a series on that issue. It turns out Kitavan cholesterol is normal, the hunter-gatherers who had low cholesterol were ridden with parasites.
Its seems that most hunter/gatherers have low cholesterol. Are they all infested with parasites? It would seem to me that anyone living in that environment without medicine would have parasitic infestations.
Any cholesterol numbers available for the Okinawans? Japanese? Asians in general? They are mentioned as the example we should follow. Also, have you written or plan to write a piece on the Tarahumara Indians?
Thanks.
Rob
In the 1988 Eaton/Konner/Shostak paper that claimed low serum cholesterol for hunter gatherers, they presented no references. http://www.direct-ms.org/pdf/EvolutionPaleolithic/EatonStone%20Agers%20Fast%20Lane.pdf. I haven’t seen other reports of this, will have to search.
I’m rather doubtful this data is trustworthy.
There is this one from professor Cordain making the claim, he even has a chart, although I don’t see any references, but I’m tired and about to go to bed so I might just have missed it. http://www.sciencedirect.com/science/article/pii/S0735109704007168
These sorts of blog posts is why you rock. High-quality and useful information that other people simply aren’t covering very well; hard to beat that.
while being treated with the oral chelator DMSA my LDL increased from 130 to 165. Makes sense.
Hi Paul. You might find this article by Stephanie Seneff interesting: http://people.csail.mit.edu/seneff/statins_pregnancy_sepsis_cancer_heart_failure.html I liked especially the sepsis part.
Outstanding. I’m licking my chops. Looking forward to more of this chronic infection angle. I think this is what sets your approach apart from the other ones.
Paul, I know that having low TC is bad, but how high is too high of a number?
Glad to see you’re back. Another great post and interesting topic. Looking forward to your second year of blogging.
Hi Stabby,
Thanks, looks like I have to make a detour to examine this issue.
Hi Valtsu,
All of Stephanie’s essays are good. Hard to believe anyone would think statins would help sepsis, but I’ve seen those papers.
Hi Kevin,
I think the JLIT numbers are a fair guide – LDL over 160, TC over 260 are probably a matter for concern.
Adequate cholesterol is necessary for the production of Vitamin D. Vitamin D has proven to greatly strengthen the immune system.
Jake,
Our body manufactures all the cholesterol we need. The dietary requirement for cholesterol is zero!
Hope this helps.
And the medical profession tries to bring total cholesterol 200 mg/dl or below with statin therapy?
That seems a bit misguided…
I guess it’s good if you’re a cardiologist, but not so hot if you’re an infectious disease specialist, or a patient.
This is really interesting — I look forward to more!
I had a question about the PHD though…
You list white rice as a safe starch. However, as far as vitamins and minerals go, rice doesn’t appear to have anything on starches like potatoes or yams. So should we opt for the latter types of starches over the former? Or is the fact they are a starch the healthfullness you are going for?
Basically, I’m asking if rice is optimal or just “it won’t hurt you.” Does white rice have an actual health benefit? Thanks!
Hi Mimi,
“Safe” just means low in toxins; it doesn’t mean high in nutrients.
Higher nutrient density diets are better, but if you’re taking a multivitamin-multimineral it’s not a big deal. Remember this is only ~20% of calories we’re talking about, so if rice has half the nutrient density of potatoes, then you’ll be getting 10% less nutrients by eating the rice. Given rice’s convenience, usefulness for noodles/crackers/bread, and the benefits of variety, there’s no reason to exclude it from the diet.
Glucose from starch is a nutrient and, in moderation, does have health benefits. I did a “Zero-Carb Dangers” series explaining some of the risks of being deficient in that nutrient, see http://perfecthealthdiet.com/?cat=105.
Best, Paul
I remember learning in med school (as part of the lipid learning) that cholesterol tends to rise as we get older, which was suggested to be pathologic and didn’t happen in people eating a low fat diet… I don’t have references for that, but I remember graphs and charts were used in the lecture.
check out this author’s reply to a Lancet article about how mortality is highest for the lowest quartile of cholesterol –
http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(01)06910-0/fulltext
“Sir—The central, surprising, finding from our study was that low serum cholesterol, persisting for 20 years, increased subsequent all-cause mortality. We have no logical explanation for this finding, nor, apparently, do any of our correspondents.”
Another chart – the data is remarkably consistent, I must say…
http://www.google.com/imgres?imgurl=http://jmarkp.co.uk/ramblings/wp-content/uploads/2010/02/CholesterolGraphs.jpg&imgrefurl=http://jmarkp.co.uk/ramblings/%3Ftag%3Ddiet&usg=__L_Dykjd7HwvK0bQ6lJO8wgn8Z3o=&h=865&w=1326&sz=174&hl=en&start=0&zoom=1&tbnid=wNrEdnAa8HWFwM:&tbnh=127&tbnw=195&ei=WkoCTr3OCsHKgQeLkdXaDQ&prev=/search%3Fq%3Dwomen%2Bcholesterol%2Bmortality%26hl%3Den%26sa%3DX%26rls%3Dcom.microsoft:en-us:IE-SearchBox%26biw%3D1259%26bih%3D588%26tbm%3Disch%26prmd%3Divns&itbs=1&iact=hc&vpx=125&vpy=131&dur=3953&hovh=181&hovw=278&tx=120&ty=76&page=1&ndsp=19&ved=1t:429,r:13,s:0&biw=1259&bih=588
(sorry about the crazy long link!)
Hi Emily,
Very nice figures. I agree – the data is remarkably consistent – unless it comes from someone named Cordain or Eaton!
Higher cholesterol is beneficial in old age. Don’t a lot of the centerians (sp?) have higher cholesterol?
Or is it higher HDL and lower LDL?
Both are beneficial, within limits; but HDL especially.
Hi Paul
From a study of nearly half a million Koreans lasting 6 years:
” The cholesterol level related with the lowest mortality ranged from 211 to 251 mg/100 ml, which was higher than the mean cholesterol level of study subjects.”
http://www.ncbi.nlm.nih.gov/pubmed/10965970
free full text available
Take care
Paul,
Your data and discussion matches the research, data and conclusions from Kendrick’s “The great cholesterol con” (not to be confused with similar title Copolo book) as well as Ravnskov’s “Fat and Cholesterol are good for you”.
Both useful reads on this topic.
Hi Miki,
Thanks much, hadn’t seen that one. Consistent with the idea that diseased people have lower cholesterol than healthy people.
Hi Chris,
Yes, good writers, thanks for the recommendations.
I’m sure you are aware of this one:
Ravnskov U, McCully Kilmer S. Inflammation in atherosclerosis. Roles of microbes and the lipoprotein immune system. Letter to Journal of the American College of Cardiology; sent on December 21, 2009.
Thanks, Stipetic. This one is available online: http://www.thincs.org/unpublic.UR,KMcCully%2009.htm. That’s basically the topic of next week’s blog posts.
My Grandmother-in-law just turned 93. Her TC is over 500 and has been for decades. She just keeps on living with it. Docs tried to put her on statins multiple times over the years. Instead, she just lets her body do it’s thing.
Who is winning?
Also, check out this graph from a huge study done regarding heart attack incidents and the corresponding cholesterol levels. Of all the people with incidents, fewest came from the group who had above 60 HDL and above 160 LDL. Quite interesting, isn’t it?
http://astute.cardiosource.com/2007/vposters/pdf/275_Fonarow.pdf
Hi Jack,
My wife’s aunt Hilda smoked up into her 70’s. She went on to live to the ripe old age of 99. I wouldn’t recommend smoking though. ;o)
I don’t understand why LDL 160 and higher would be associated with fewer cardiac incidents unless those people had the large type A kind.
Hi Jack,
Congrats to your grandmother-in-law! May she keep winning.
The graph is quite interesting but actually one of the interesting parts is how weakly mortality depends on LDL. If you scale by numbers to get a relative risk, there’s not a huge variation across the cohorts.
In any case, there’s no support for statins in it!
Paul one more comment on the graph.
Beyond a TC of 220, the curves trend back up. HOWEVER there are so few datapoints beyond 220 I wonder that its seems to be a very weak correlation when trending back up. I am tempted to discount that.
Still great to have another great article that can be sent to people!
Paul:
What role does Lipoprotein fractions play in this? Many docs care more about LDL particles than LDL, and the mix of the LDL particles between large and small via NMR. As you know you can have an LDL of 180, but particle count of only 1100(great) or 2200( not so great).
Total cholesterol is pretty meaningless in my view if heart disease is the issue. Be interested in your thoughts
Hi steve,
I haven’t yet decided how deep I’ll get into the biology in this series. LDL particles are designed to be modified in various ways during infection or presence of toxins, and modifications affect particle sizes and other characteristics of the particle, and determine the ultimate destination and disposition of the particle.
So LDL particle characteristics are in some ways a good biomarker of health.
What each aspect means, particle number, size, chemical modifications, etc., is a fairly complex topic and still a subject of research. We might be able to have a fuller discussion of that later in this series.
Best, Paul
Hi Paul:
Could not agree with you more regarding its complexity, but i for one believe it is behind heart disease and the oxidation of the particles, particularly the small one leads to plaque which is related to infection, at least in my view.
Be interested in hearing your thoughts at the appropriate time. I would also add that for some their underlying biological processes are out of kilter: they may hyper-absorb fat in the intestine, or they may excessively synthesize cholesterol,etc in the liver all of which will some level of infection/inflammation leads to the CAD we see.
While some Paleo bloggers feel an anti-inflammatory diet is high in fat, and animal fat in particular, the Japanese experience of low heart disease and a low animal fat diet seems to be otherwise. Interested in your thoughts. Thanks
Hi steve,
Yes, the many destinations and sources of LDL is another complexity.
The relationship of diet and inflammation is also complex. Food toxins and omega-6 are almost always inflammatory, but when it comes to macronutrients I almost feel it’s not worth discussing the “inflammatoriness” of the diet except in the context of an individual patient. For someone with Candida & protozoal infections low carb can be inflammatory; for someone with bacterial infections high carb is inflammatory.
Best, Paul
I may be jumping the gun here, but from my understanding oxLDL is a major factor in the onset of disease; it is stongly associated with heart disease, for example. And it wouldn’t surprise me if oxLDL was also partly to blame for other infections.
And (surprise!)oxLDL is associated to the usual suspects: excess PUFA & sugar & hyperglycemia.
But this begs the question. Would a higher LDL number reflect a greater liklihood of that LDL becoming oxLDL? So if your TC is >260 would it be even more important to restrict those oxidizing factors from your diet? Does risk increase in a linear fashion? I just wonder if this is what’s being addressed in that Cordain paper Stabby posted. When eating the SAD maybe it would be beneficial to lower TC as this would limit oxLDL and all its problems, no? Would this provide favourable short-term benefits but maybe harm in the long term?
Looking forward to the rest of the series!
Rober:
I believe some of the literature indicates that the higher the LDL particle count the greater the risk regardless of the size of the LDL: See Atvos, i think, on Pubmed. The longer the particles hang out in the bloodstream the greater the danger.
Hi Paul,
What are your thoughts on this critique? I’m paraphrasing. I’d like to look beyond the style the critique is presented and focus on the content constructively.
Primitive Nutrition 40 Playing Games with Your Heart, Part I
1. http://perfecthealthdiet.com/wp/wp-content/uploads/2011/06/O-Primitivo-Cholesterol.jpg
Could the worse mortality be infectious disease and/or sanitation in less favorable health care populations, as opposed to animal vs. plant consumption?
2. http://perfecthealthdiet.com/wp/wp-content/uploads/2011/06/JLIT-Mortality-Table.jpg
Could the higher risk at low cholesterol be due to the statin drug, as opposed to having low cholesterol due to healthy diet?
Thanks,
Mark
Hi Mark,
1. Yes, all these things go together. If people are healthy then their total cholesterol will be 200 to 250 mg/dl. They have to get sick to have low cholesterol; globally low cholesterol is mainly due to parasitic infections or malnourishment. The same factors that cause low cholesterol cause high mortality and are associated with low income.
2. Yes, that’s a possibility. But people with low cholesterol who don’t take statins have higher mortality too, so there’s plenty of reason to think that low cholesterol is a problem in and of itself.
Thanks Paul,
It’s confusing and I still wonder if healthy people can have low cholesterol. I understand there are some correlations with sickness and low cholesterol, but I’m not sure that I see the proof low cholesterol means sickness.
For example, Peter Attia seems pretty focused on healthy lifestyle. Is his low cholesterol a sign of ill health?
http://eatingacademy.com/how-low-carb-diet-reduced-my-risk-of-heart-disease
TC: 160
LDL: 59
HDL: 85
TGs: 81
Thanks Paul.
Do you have any recommended reading material or studies to direct me to showing that “people with low cholesterol who don’t take statins have higher mortality too”?
I’m relatively new to all of this (I was introduced to the PHD by some friends and just started reading your book last week), but I was surprised to be reading that lower cholesterol was dangerous.
Thanks again, and I look forward to your response (or the response of anyone else that can help me).
Does Paul not get comment notices for old posts? He’s usually pretty quick at responding to people, but Mark above received no response to the questions about the critique from the “Plant Positive” website’s “Primitive Nutrition” video, “Playing Games with Your Heart, Part I”. Paul, can you please provide a response to these questions?
Thank you,
Chris
Hi Chris,
OK, I’ve replied.
My cholesterol is normally around 240 with high hdl, low trigs. I had a flu (fever, muscle aches and phlegmy cough) recently and had labwork done about 7 days after the onset. My fever had been gone for about 4 days prior to the test but I was still coughing, and I couldn’t move my appointment because of work. The doc always tests cholesterol despite me mentioning my recent illness and it came back the lowest it’s ever been in my life — 169! Could a very recent virus create such a drop? I’m concerned that the low level will lower my immunity.
Infections can have a significant effect on cholesterol. It probably means the your serum lipoproteins are helping fight the infection. Probably when you recover they’ll come back to normal.
Thank you so much for taking the time to respond. I’m gonna double up on my daily eggs. So many people at my office are sick with the flu and coughing everywhere so I want my “high” cholesterol back stat. 🙂
Good grief! Now I’ve heard everything!!! Increasing your dietary cholesterol to “protect” you from colds and flu? If you really want to protect yourself, get lots of rest and make sure you get adequate zinc. Fruits and vegetables would be a good idea also.
Paul,
It appears all the Ricardo Carvalho / O Primitivo links are dead.
Hi Paul,
Dead links to Ricardo Cavalho.
Thank for this graph anyway.
Aviva Evron
making assumptions by correlating two dependnt variables when there are many interrelated dependencies is what we call bad science. You need to control fo so many factors to tease out any actual relationship. Namely all of the conditions for the diesease that are related to increses in cholesterol levels. Like access to medications and medical procedures that are dependent upon income levels. Cholesterol levels increase with increases in income which results in access to antibiotics. So on a basic level cholesterol levels are positively dependent upon income levels. This will mess up all of these assumptions made here.
Correlations are suggestive and an observed correlation is generally the starting point for research that ultimately determines causality. Such research must take account of confounders such as income. But, I’m puzzled what “assumptions” you think I’m making here. Did you not notice this was the introduction to a series? Correlating two variables is not an assumption.
It seems like you didn’t read the series of articles and just made a random comment with no substance. He’s taking into account the lack of causality with the data and the whole issue with the confounding variables at hand. Not a single assumption he made would be messed up by income levels as a confounding variable. It would actually support the point he is making.