I was going to write a single post about how to implement a therapeutic ketogenic (ketone-generating) diet.
But then I thought it was worth spelling out issues in some detail. There are various ways to make a diet ketogenic, and different ways are appropriate in different diseases. Also, different diseases may call for a different balance between three criteria:
1) Safety. Does the diet generate side effects?
2) Therapy. Is the diet as curative as it can be?
3) Pleasurability and practicality. Is the diet unnecessarily expensive, unpalatable, or boring?
I soon realized that with so many factors affecting diet design, it would be hard to fit everything into a single post. So I’m going to split up the discussion into parts. Today I’ll look at the various ways to make a diet ketogenic. On Tuesday I’ll look at how to design a diet for Kindy’s NBIA kids. We’ll look at what they’re eating now, and consider ways they might be able to improve their diets further – and, hopefully, get further improvements in health, longevity, and function.
Maybe we’ll look at some other diseases after that, or maybe I’ll just move on to the lemon juice series I’ve been planning. The lemon juice and acid-base balance issues will fit in nicely since kidney stones and acidosis are risks of ketogenic diets and lemon juice relieves those risks.
So: how can we make a diet ketogenic?
What Is a Ketone?
The liver is responsible for making sure that the body (but especially the brain and heart) have access to a sufficient supply of energy from the blood. To fulfill that responsibility, it manufactures two energy substrates – glucose and ketones – and exports them into the blood as needed.
The most important ketones are acetoacetic acid and beta-hydroxybutyric acid.
Ketones are water-soluble small molecules. They diffuse throughout the body into cells, and are taken up by mitochondria and oxidized for energy.
Ketones are especially important to neurons, which can only consume glucose or ketones. So if something is wrong with glucose metabolism, ketones can be the sole usable energy source of neurons. (Other cell types, but not neurons, burn fats.)
Manufacture of Glucose and Ketones During Starvation
While preparing this post, I was surprised at how long it took for doctors to appreciate that ketones are an acceptable alternative energy source for the brain. The realization that the brain doesn’t perpetually rely on glucose during starvation apparently didn’t sink in until 1967!
The use of prolonged starvation for the treatment of obesity has posed a fascinating problem; namely, that man is capable of fasting for periods of time beyond which he would have utilized all of his carbohydrate resources and all of his proteins for gluconeogenesis in order to provide adequate calories as glucose for the central nervous system.
This study was designed to clarify the apparent paradox, and it was found that beta-hydroxybutyrate and acetoacetate replace glucose as the brain’s primary fuel during starvation. [1]
This makes it a bit easier to understand why ketogenic diets have not yet become standard therapies for neurological diseases. Epileptics caught a lucky break – the ketogenic diet was already in use for epilepsy in the 1920s. The ketogenic diet’s therapeutic potential for other neurological disorders probably couldn’t have been appreciated until after 1967, and by then medicine had turned its back on dietary therapy.
But back to ketones. During starvation, glucose and ketones have to be manufactured from body parts. The body’s resources include:
- Glycogen – a storage form of glucose. However, glycogen supplies are minimal.
- “Complete” protein – a mix of amino acids similar to that found in animal meats.
- Long-chain fats – fatty acids 14-carbons or longer in length, attached to a glycerol backbone as either triglycerides or phospholipids.
During starvation, different raw materials end up as different energy substrates:
- Glycogen can be used to make glucose but not ketones. So glycogen converts 100% to glucose.
- Protein is broken down into its constituent amino acids. Some amino acids can become glucose but never ketones; some can become either; some can become ketones but glucose. “Complete” protein usually found in the body typically converts 46% to ketones, 54% to glucose. [UPDATE: Actually, this is incorrect. As Tony Mach points out in the comments, complete protein converts 20% to ketones, 80% to glucose. The 46-54 ratio is the contribution to Wilder’s ketogenic ratio, see below.]
- Triglycerides and phospholipids are broken up into their constituent parts. The fatty acids can make ketones but not glucose; the glycerol backbones can make glucose but not ketones. Typically, 10-12% of energy from a triglyceride is in the form of glycerol (which has the potential to become glucose) and 88-90% is in the form of fatty acids (which have the potential to become ketones).
As we note in the book, during starvation the body is cannibalizing tissues that are roughly 74% fat, 26% protein by calories. Due to the preponderance of fat, starvation is highly “ketogenic” (ketone generating). The 26% of calories that are protein generate roughly equal amounts of ketones and glucose, but the 74% of calories that are fat generate only ketones.
This doesn’t mean that during starvation ketones are 87% of energy and glucose 13% of energy. Most of the fats are burnt directly for energy without conversion to ketones. But a fair amount of fats are diverted into ketone production, and ketones are abundant during starvation.
A Ketogenic Diet Using “Body Part Foods”
If your diet could include only compounds found in the body – glucose, complete protein, and long-chain fats stored as triglycerides or phospholipids – then we can use the above numbers to estimate the “ketogenic potential” of the diet.
I have to credit commenter “Cathy” at the PaNu Forum for this next part. Kindy posted a question about the ketogenic diet for NBIA on the PaNu Forum in October 2010, and Cathy left an informative comment:
The ketogenic formula was originally developed by Wilder at the Mayo clinic in the 1920’s. By googling WILDER KETOGENIC FORMULA, I found a link to the book “The Ketogenic Diet: A Treatment for Epilepsy” published in 2000. Quite a bit of the book is available for reading online; here is the URL
.
On page 36 of this book is Wilder’s formula for the ketogenic potential of a diet:
This formula basically treats all fats as triglycerides of long-chain fatty acids, and protein as “complete” protein with a typical mix of amino acids. It makes a ratio of the ketone precursors to the glucose precursors.
Wilder’s “ketogenic ratio” was used by Dr. Richard Bernstein in his Diabetes Solution to help people appraise the ketogenicity of a diet. A ratio below 1.5 signifies a minimally ketogenic diet; the higher the ratio goes above 1.5, the more ketones will be generated.
Other Dietary Ketone Precursors
If you’re not starving, you have the opportunity to eat foods that are not components of the body, and that are more ketogenic than “body part foods.”
Specifically, you can eat:
- Short-chain fats such as are found in coconut oil.
- A mix of amino acids that is not “complete,” but is biased toward the ketogenic amino acids.
If you do this then your diet will be more ketogenic than Wilder’s formula would suggest.
Eating these foods may be advantageous. For instance, suppose you want to eat enough carbs to avoid “zero-carb dangers” such as mucus deficiency. At the same time, you want to generate abundant ketones to nourish the brain. You can achieve both by eating carbs for glucose, but also eating short-chain fats and ketogenic amino acids to make ketones.
So let’s look at why these foods are so effective at producing ketones.
Amino Acids
The main metabolic process which converts one metabolic substrate into another is called the citric acid cycle, tricarboxylic acid (TCA) cycle, or Krebs cycle.
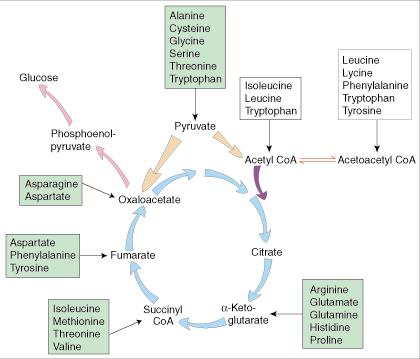
The TCA cycle looks like this (blue arrows):
The passage from succinyl CoA to fumarate is where ATP is made. The cycle can be fed in several ways:
- By pyruvate which is an intermediate produced in glucose metabolism;
- By acetyl CoA which is an intermediate produced by ketones or fatty acid oxidation;
- By amino acids which can enter the TCA cycle at various points.
The green boxes show glucogenic amino acids entering the cycle. The white boxes show ketogenic amino acids that are made into either acetyl CoA or acetoacetyl CoA and thence can either leave as ketones (via HMG-CoA) or enter the cycle by conversion of acetyl CoA to citrate.
The crucial takeaway, as far as this post is concerned, is the distribution of amino acids among green and white boxes:
- Leucine and lysine appear only in white boxes, not in green boxes. They are purely ketogenic.
- Isoleucine, tryptophan, phenylalanine, and tyrosine appear in both green and white boxes. They can be either ketogenic or glucogenic.
- The other amino acids appear only in green boxes and are purely glucogenic.
So if the diet is rich in leucine and lysine, but poor in glucogenic amino acids, then it will be highly ketogenic.
Short-Chain Fats
Fats are made into acetyl CoA. Acetyl CoA can either enter the TCA cycle or be converted to ketones. What decides which way it goes?
One important factor is whether the cell has enough ATP. If the cell has plenty of ATP then it won’t allow the TCA cycle to make any more, and the TCA cycle gets stuffed with succinyl CoA and then with all the other intermediates in the pipeline behind it.
Once the TCA cycle is full, acetyl CoA no longer enters the cycle and instead leaves as ketones.
Long-chain fats can follow this route, but not terribly easily. They have alternatives:
- Long-chain fats can serve as structural molecules in cell membranes throughout the body.
- Long-chain fats can be stored in adipose cells.
- Long-chain fats can be burned by cells throughout the body, and transported to cells that need them.
These factors mean that you have to eat a very large amount of long-chain fats before you produce substantial ketones.
Short-chain fats (12 carbons or less in length; often called medium-chain) are different. Short-chain fats do not appear in cell membranes and are not stored in adipose tissue (except for a little 12-carbon fatty acids). Rather than being transported throughout the body, they are shunted to the liver for disposal.
This means that if you eat a lot of coconut oil (which is 58% short-chain fats), you deliver a lot of fat to the liver for disposal. The disposal process for fat is conversion to acetyl CoA followed by either burning in the TCA cycle or conversion to ketones.
After a big cup of coconut oil is delivered to the liver, the liver’s ATP levels are quickly saturated. The TCA cycle is stuffed and the liver will dispose of the coconut oil by making ketones.
It will do this whether the rest of the body needs the ketones or not. The liver wants to get rid of the coconut oil, and it does it by making ketones whether the rest of the body wants them or not.
Summary
So we have three ways to make the diet ketogenic:
1) Make Wilder’s “ketogenic ratio” high by eating a lot of fat, very few carbs, and not too much protein.
2) Supplement with the ketogenic amino acids lysine and leucine.
3) Supplement with coconut oil or another source of short-chain fats.
If we do (2) or (3), then the diet can be ketogenic even if it has a fair number of carbs.
So now we have an arsenal of ways to generate ketones. We have to look at diseases and diet risks to figure out which way of making the diet ketogenic is optimal.
I’ll look at that next week.
References
[1] Owen OE et al. Brain metabolism during fasting. J Clin Invest. 1967 Oct;46(10):1589-95. http://pmid.us/6061736.







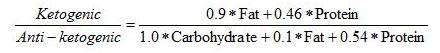




Does anyone know, if supplements (minerals, colostrum etc.) interrupt intermittent fasting?
how should i incorporate l-leucine into my ketogenic diet? ie, when is the best time to take it — time of day, with/without food, etc? i have read that the dosage is approximately 16mg per kg of body weight. is that correct? do you take that all at one time? help!
Hi Paul,
Firstly, thanks for the science. I first stumbled on your book after I read somewhere that a ketogenic diet might help with migraines. At 47 I have suffered for more than 15 years, and now get migraines almost daily. As I have demanding job, this has now led to a chronic level to triptan usage just to cope and do the basic tasks of living. For the most part that works ok, but as the condition is constantly working and becoming more drug resistant I ham constantly searching for new answers. I have read the book and relaxant blog posts and have now started a Keto diet. I have ordered your recommend Keto diet supplements and am committed to the journey. Which I am happy to update you on in the interest of science, and more importantly to help others.
One question, I have read your advice regarding MCTs and leucine and lysine to help ensure the maintenance of ketosis (coconut oil supplementation is underway and other supplements ordered) whilst consuming an appropriate level of carbs, but the one simple answer I can’t find is the minimum percentage of carbs you recommend on the PHD that is needed to prevent the low carb dangers – recognising my desire to remain in ketosis. I know the answer won’t be 5% as per a lot of LCHF blogs, but is it 30%? Can you help, the reason it’s impt is to help me input this into Myfitness pal and other Keto macronutrients tracking tools.
Thank you
I think at a minimum you need 200 calories per day (10-15% of calories) of digestible starches, plus vegetables. You want high-fiber starchy plants like potatoes or other tubers.
Also, experiment. It’s likely you only need to enter ketosis for a few hours per day, which can be done by eating MCT-oil flavored coffee at the end of a 16 hour overnight fast. If that’s the case, you will be able to increase carb intake.
Best, Paul
“… some can become ketones but glucose.”
Misprint?
If not, what does that mean?
Fixed it, thank you!
Hi Paul. Big fan of your work. Thanks for all of the empowering knowledge you provide. I’ve one question with regard to making a diet ketogenic by using coconut oir MCT oil. Let’s say a person is consuming 85 g of carbs a day (from leafy greens and small amounts of safe starch) and that person also consumes 7 tablespoons of coconut oil spread throughout the day (to ensure the liver produces ketones). If there is glucose circulating due to the carbs and ketones circulating due to the coconut oil – how do we know which the body (and brain) will preferentially use for energy? I hope my question makes sense! Thanks in advance, Conor
*coconut oil or MCT oil
The body knows how to partition nutrients to their most desirable destinations. In general, ketones will be consumed first and others later. This is because ketones cannot be stored as ketones (whereas glucose can be stored as glycogen), though ketones can be converted to lipids.
Thanks Paul! Much appreciated!!
Hi Paul,
What amazing work you do. Its just great to have access to a trusted and reliable (well researched) source. So, that’s the love-in bit’;~}. Thanks.
Now a question please.
Its about MCT and coconut oil.
1:
You wrote in this thread ” – – – eating MCT-oil flavored coffee at the end of a 16 hour overnight fast.”
You got me thinking, I’ve been “using” butter in coffee with cocout oil (or sometimes MCT) on awaking. (About 30 grams of each added to a brew made with 19g of organic coffee with 80C water in an aeropress). It gets me through til 13:00 so I’m sticking to my daily intermittent fast. Seems to fire up my brain too and fuels me through my weekly Body By Science session or a mountainbike ride.
BUT, are you suggesting that it should only be taken at the END of the fasting period? Mr. Bulletproof seems to suggest that it’s “allowed” during the fast as there’s no protein in it?
Also I think I’ve seen you mention taking as much coffee with heavy cream as wanted during intermittent fasting?
Have I got it wrong?
Thanks
2:
You seem to use the terms “coconut oil” and “MCT” pretty much interchangeably here and in the book (love that book), but there are some differences, aren’t there. Purveyors of MCT suggest that it’s 6x more “efficient” than coconut oil. Whereas coconut oil supporters suggest that some of the good stuff is removed when making MCT from coconut oil. They even suggest that MCT is a bi-product of the extraction of Lauric acid (that’s the good stuff, right) from coconut oil.
So are they interchangeable or maybe there are times where one is more applicable than the other? Both are food of course I get that.
I wonder if there’s anything to that C-8 MCT (super short chain) that some claim to be magnitudes more “effective” than standard MCT and WAY more effective the plain old coconut oil?
I THINK I’ve noticed being able to fuel a hilly mountainbike ride with regular MCT (a dessertspoonful), but as there are good days and bad days at my age (62) its hardly a controlled test.
Thanks Paul
I hope this is one thats worth answering ‘;~}
Hi Neil,
Calories will suppress many of the benefits of fasting, even if they are fat calories or ketones. (You may still get the neurological benefits of fasting, but you won’t get the cardiac benefits or the anti-aging or anti-infective benefits.) You are taking 60 grams of fat each morning, which is 540 calories. That is about 6 hours worth of calories, for a 2200 calorie daily diet. It’s no wonder it suppresses appetite until 1 pm, but it is not fasting.
I think you should take less fat, and yes, toward the end of your fast if you want more of the benefits of fasting.
Coconut oil is 55% MCT, the rest is more akin to butter in its fatty acid composition.
Best, Paul
Paul
Thankyou for your wise words.
I’ll try having just plain coffee on waking (or maybe with just a tablespoon of coconut milk for taste?), unless it’s a workout day.
Maybe the coffee with fat (maybe 30g fat) can be my lunch, taken about noon.
I should have realised that combining “bulletproof” strategy with yours was something that needed more thought.
I can see that there’s more to coconut oil than plain MCT (eg lauric acid ) so will keep using them both.
Again, thanks for your guidance.
Based on the Wilder formula, which you provide in your letter of February 24, 2011, the “Perfect Health Diet” of 65% fat, 20,% carbohydrate and 15% protein appears to be a ketogenic diet as the wilder number of 1.89 which is mildly ketogenic. Am I correct on that?
Hi Jack, In the 2012 edition of the book we revised our macronutrient recommendations to 55% fat, 30% carb. I would agree that the earlier macro ratios verge on the ketogenic — in the sense that one could readily generate ketones toward the end of a 16 hour overnight fast. However, it wasn’t our intention to make the diet ketogenic, as ketone production generally indicates that one is getting fewer carbs than the body desires, and suggests one should eat more carbs. We see ketogenic dieting as a therapeutic strategy suitable for fairly rare conditions, not as a desirable routine diet. Best, Paul
As one who has struggled with psychiatric disorders and energy issues for years, the ketogenic diet has worked wonders for me in many ways. I ran into a few issues on a severely carb-restricted diet and decided to use caprylic acid as a supplement so that I could still get the benefit of those ketones while avoiding other complications. In any case, I’ve stumbled across a strange problem that not many other people seem to experience, at least as far as I can tell. (I’ve only seen 2 or 3 other people online mention this.) A teaspoon of Brain Octane causes strange sensations of joint and muscle pain throughout my body — fingers, feet, shoulders, all over. It’s not disabling at all but pretty darn annoying and disconcerting. I have some ideas as to why this may be, but I’d like to get an expert’s opinion. I’ve had minor inflammatory issues for years, which I partly control through diet and avoiding extreme cold, so it’s not like this is totally out of the blue. Nevertheless, MCTs are more often associated with a decrease of inflammation and joint pain, not the other way around. And it really does seem like there is a connection between C8 consumptions and the worsening of symptoms. Any ideas?
Hi Eric, interesting. I don’t know what’s causing it, but the likelihood is that the caprylic acid is triggering inflammation through interactions with microbes either in the small intestine, liver, or joints. The inflammation generates symptoms primarily in the joints because those are already somewhat injured (which is a common situation because people don’t eat enough extracellular matrix). To address it, the usually tactics for clearing infections, whether in the gut or systemic, and repairing extracellular matrix should work. Best, Paul
Looks like it must have been something in the gut. I’ve been eating lots of yogurt and drinking lots of kefir along with some probiotic “gut shots” and aloe. The aches and pains have almost completely disappeared. My dermatitis is even clearing up as well.
I am a 51 year old female that just found out I have Parkinson’s about a year and half, but I have been having signs of it for years, tremors, depression, body weakness. ECT. I honestly don’t think my doctor was reading the signs because of my gender and age. A few years ago I had my shoulder lock up on me and I was sent to a P.T since x-rays didn’t show any physical damage. My shaking was getting worse and I began falling. Only when my speech became so bad that it brought concern to my dentist was Parkinson’s even considered. He phoned my doctor with his concerns about my shaking and balance problems. By this time I was forgoing shots in the back of my neck for back and neck pain to which once again I was sent to a P.T (although x-rays showed no damage) I was told I had a few spurs which were most likely causing the pain. Here I was feeling like my whole body was falling apart and doctor could not find anything wrong, maybe in was all in my head? My doctor even seemed annoyed with me and things just kept progressing and I just kept it to myself, why bother going through testing and them finding nothing? Well, it was after my second P.T called my doctor about the weakness in my legs and arms, by this time I have developed a gait in my walk and I fell more frequently. Only then did my doctor send me to a specialist and it was found that I had Parkinson’s, and that I have had it for awhile. I think because I was a woman that my signs and symptoms weren’t taken seriously and therefor left untreated for so long,I was taking pramipexole dihydrochloride three times daily, I Was on carbidopa levodopa but only lasted 90 minutes then wore off.I found that none of the current medications worked effective for me.I got tired of using those medication so I decided to apply natural herbs formula that was prescribed to me by my second P.T, i purchase the herbal formula from totalcureherbsfoundation. com, There has been huge progression ever since I start the treatment plan which will last for 15 weeks usage.all the symptoms and sign has begin to disappear .
Hi. Is it possible for an ectomorph very lean at a very cold temperature and with no to much clothes go in ketosis even if he eats 100 grams of carb per day?
I’m a very strong ectomorph and I used keto-stick to monitor that, and I found if I move a lot (walking 5-7 Kms per day) I can go in a moderate ketosis even with 100 grams of rice per day).
How is this possible?
Best Regards.
Salvatore Esposito.
Hi Salvatore, yes, if you are very active you can go into ketosis eating 100 g of carbs per day.
First, the 100g refers to digestible carbs not weight of food, i.e. 400 calories whatever the weight to get there. Moreover, that is the minimum that is used by a normally active person in comfortable environments. Vigorous activity and cold exposure will consume carbs and increase the number of carbs you need to eat to stay out of ketosis.
Best, Paul
Thanks Paul.
I have another question.
Is there a way to redirect glucose towards muscles for glycogen replenishment so i can minimize the liver load and get back in ketosis in a couple of hours?
What do you think about?
And if I move after 30′