We’ve learned enough in the last two years to revisit the supplementation advice from our book, and toward that end I am starting a series on micronutrients.
I’ve recently been looking at some papers studying the effects of food fortification with micronutrients. These changes provide a sort of “natural experiment” which may provide insight into the benefits and risks of supplementation.
Fortification of Food
Grain products are the most important category of fortified foods. Industrially produced baked goods must generally use enriched flour, and Wikipedia (“Enriched Flour”) tells us what they’re enriched with:
According to the FDA, a pound of enriched flour must have the following quantities of nutrients to qualify: 2.9 milligrams of thiamin, 1.8 milligrams of riboflavin, 24 milligrams of niacin, 0.7 milligrams of folic acid, and 20 milligrams of iron.
This is an ironic choice of nutrients. While thiamin and riboflavin are harmless, niacin, folic acid, and iron are three micronutrients we recommend NOT supplementing in the book. Another nutrient we recommend NOT supplementing, vitamin A, is also a fortified nutrient, although not in flour.
Perhaps not even for that!
A history of nutrient fortification over time can be found at this USDA site. Enrichment has a long history, but the amount of fortification has increased substantially since the 1960s. Enrichment mixtures were added to rice, cornmeal/grits, and margarine beginning in 1969, and to ready-to-eat cereals, flour, and semolina beginning in 1973. Inclusion of high levels of folic acid in all enriched foods became mandatory in 1998.
You may have noticed that when putting raw rice in water, a white powder comes off the rice. This is the enrichment mixture which contains folic acid. According to the American Rice Company (hat tip: Matthew Dalby),
The enrichment mixture is applied to rice as a coating. Therefore, it is recommended that rice not be rinsed before or after cooking and not be cooked in excessive amounts of water and then drained. The enrichment … would be lost.
This is useful information: We can remove the enrichment coating by rinsing rice before cooking. That may turn out to be a good idea!
The Contribution of Fortification to Nutrient Intake
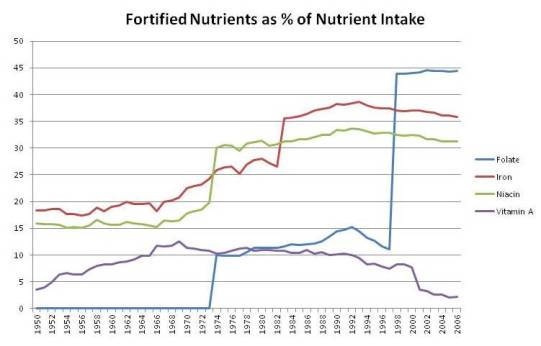
Using USDA data for the four nutrients most likely to be harmful in excess, I made up a chart of the contribution of fortified nutrients to total nutrient intake among Americans. It looks like this:
You can see sharp rises in fortified niacin and folic acid in 1973, in iron in 1983, and again in folic acid in 1998. By 1998, folic acid in fortified foods constituted 44% of all dietary folate, and enrichment mixtures provided one-third of all iron and niacin. Fortified vitamin A provided about 10% of all dietary vitamin A from 1964 through 2000.
Folic Acid
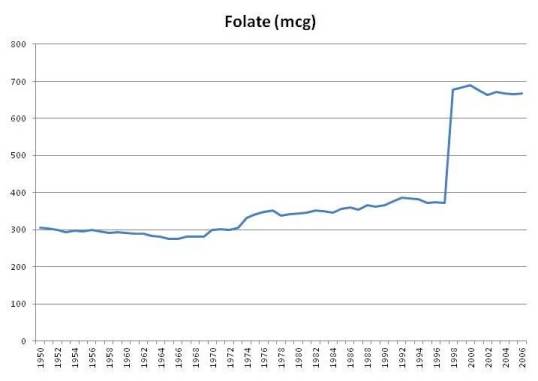
Here is a chart of per capita daily intake of fortified folic acid plus natural food folate in the United States since 1950:
Folate intake from foods has always been around 300 mcg per day, and jumped sharply when folic acid intake became mandatory in 1998. The USDA estimates that intake of folate, including folic acid, jumped from 372 mcg per person per day in 1997 to 678 mcg in 1998, and has remained above 665 mcg ever since (source).
For those who eat a lot of wheat products, intake may be even higher. A pound of enriched white flour has 770 mcg folic acid along with its 1660 calories. If Americans were getting 372 mcg folate from food prior to folic acid fortification, then someone eating a pound of enriched wheat products per day would be getting about 1,142 mcg folate from all food sources.
It’s not uncommon to eat substantial amounts of enriched wheat. The typical American eats 474 g (1800 calories) carbohydrate per day. Most of that is from enriched grains. Those eating industrially produced breads, cookies, crackers, and breakfast cereals may have a very high folic acid intake.
Add in a multivitamin – most multivitamins have 400 mcg and prenatal vitamins have 800 mcg – and a sizable fraction of the population has a folate intake of 1,500 to 1,900 mcg per day, 1200 to 1600 of it as synthetic folic acid. This is well above the tolerable upper limit (UL) for folic acid of 1000 mcg (Wikipedia, “Folate”).
Averaged over all Americans, folic acid from fortified foods comprises 44% of all food-sourced folate, but for Americans taking a multivitamin folic acid becomes 65% of all folate and, for those taking a prenatal vitamin, 75%.
There are several potential health problems that could arise from excessive intake of folic acid, and I’ll explore a few in this series.
Iron and Niacin
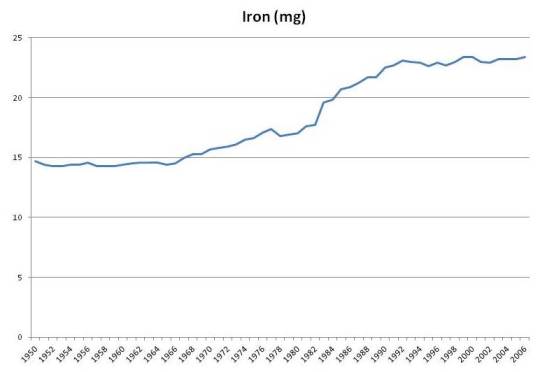
Iron intake has risen by about 50% due to fortification:
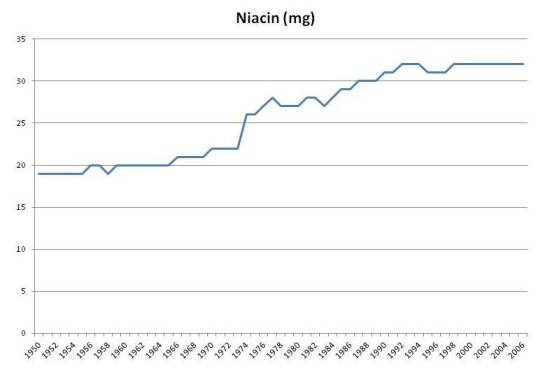
Niacin intake has also risen about 50%:
These two nutrients have similar concerns:
- An excess of each promotes infections. Niacin (in the NAD+ form) is the rate-limiting factor in bacterial metabolism. Iron is a critical mineral for oxygen handling and is needed by most infectious pathogens; in fact the immune response tries to lock up iron in ferritin during infections.
- Both niacin and iron are involved in oxygen handling during metabolism and an excess of each can aggravate oxidative stress.
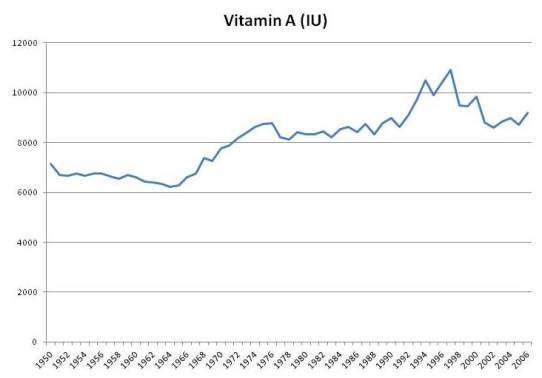
Vitamin A
Although fortification never increased vitamin A intake by more than 10%, it may serve as a marker for consumption of artificial sources of vitamin A from supplements. Moreover, total food intake of vitamin A was apparently affected by fortification; food intake of vitamin A rises in the 1960s when fortification was growing, and falls after 2000 when intake of fortified vitamin A decreased:
In the book we noted studies showing that people whose intake of vitamin A was above 10,000 IU/day tended to have higher mortality. This was most commonly observed in people taking multivitamins.
There was a period of enthusiasm for vitamin A supplementation between the 1960s and 2000. Multivitamins had more vitamin A in that period. After studies showed negative results, the vitamin A content of multivitamins was reduced.
It is possible that the source of problems may not be vitamin A per se, but degradation products of vitamin A. I’ve previously blogged about how vitamin A plus DHA (a fatty acid in fish oil) plus oxidative stress can produce highly toxic degradation products (see DHA and Angiogenesis: The Bottom Line, May 4, 2011; Omega-3s, Angiogenesis and Cancer: Part II, Apr 29, 2011; Omega-3 Fats, Angiogenesis, and Cancer: Part I, Apr 26, 2011).
Naturally occurring vitamin A in foods is located in lipid fractions and protected from oxidation by accompanying antioxidants (eg vitamin E) and oxidation-resistant lipids. Vitamin A from fortification is not so carefully protected. The Food and Agriculture Organization of the United Nations comments:
Foods which have been successfully fortified with vitamin A include margarine, fats and oils, milk, sugar, cereals, and instant noodles with spice mix. Moisture contents in excess of about 7-8% in a food are known to adversely affect the stability of vitamin A. Beyond the critical moisture content there is a rapid increase in water activity which permits various deteriorative reactions to occur. Repeated heating, as may be experienced with vegetable oils used for frying, is known to significantly degrade vitamin A. The hygroscopic nature of salt has prevented its use as a vehicle for vitamin A fortification in countries of high humidity. In trying overcome this problem, a new vitamin A fortificant, encapsulated to provide an additional moisture barrier, was evaluated with limited success. The cost of using highly protected fortificants can be prohibitive in many cases.
There aren’t many foods that don’t contain 7% water, or acquire it after fortification, so degradation is a real concern.
Vitamin A in multivitamins may also be exposed to degradation. The possibility of vitamin A degradation, especially in combination with DHA from fish oil and oxidative stress, is why I’m skeptical of the health merits of fermented cod liver oil.
Conclusion
I think exploring the effects of fortification will be an interesting topic.
We will consider whether fortification may play a role in various diseases that have become more common since 1970 or 1998, such as obesity, diabetes, and autism.
And we will consider what the health effects of food fortification may tell us about how to optimize micronutrient supplementation.












Dr. Jaminet, when you get to your review of Niacin, can you please include your comments on studies showing Niacin’s use as a treatment for hypochlorhydria? (See, for example, http://orthomolecular.org/library/jom/2001/articles/2001-v16n04-p225.shtml for more info). I just started supplementing at 500mg per meal (x3; total is 1.5g daily) 2 days ago and I’ve been very pleased to see my weight increase from my recent low of 98 lbs (I’m 5’6″ with a small frame; used to weigh about 110-115). If the mechanism is increased insulin resistance, I’m not disappointed, although I’d prefer that it actually IS addressing the hypochlorhydria. Thanks, I’ll look forward to reading your blogs on this subject.
Hi Julia,
I’m glad you’re getting your weight up. You might want to get some other B vitamins (B1, B2, B5, biotin) with the niacin.
Best, Paul
Very interesting.
first thoughts: I do not buy that niacin is harmful, as levels are regulated by tryptophan degradation, which is responsive to NAD+ requirements. Niacin supplementation seems safe enough (or indeed beneficial) at high doses, so why would smaller ones be harmful?
Folic acid: I have thought, there might be a reason why folic acid breaks down in the skin exposed to UV radiation. This might be a way of protecting irradiated skin from melanoma. Otherwise, there would be a mechanism for protecting such an important vitamin.
If they want women to have folic acid when they get pregnant, they should put it in alcohol.
Hi Paul — have you seen this study?
http://www.ncbi.nlm.nih.gov/pubmed?term=american%20journal%20of%20clinical%20nutrition%20selenium%20brazil
It seems significant that the brazil nut supplementation raised the glutathione production. Your thoughts?
Hi Kathy,
2 Brazil nuts have 100-200 mcg selenium, so it’s as expected that they worked similar to 100 mcg selenium. Selenium is needed for the glutathione peroxidase enzyme that interacts with glutathione.
Selenium is a tricky nutrient, you need some, too much is highly toxic, there’s a narrow plateau range before toxicity begins, and the selenium content of food is highly variable. Even 4 Brazil nuts a day can be enough for toxicity.
There are regions of the USA that are very high in selenium (in groundwater etc) where natives get an average 750mcg. There seems to be no obvious toxicity at this level, but higher levels in Chna have produced disease. Methionine and cysteine in the diet are probably protective against Se toxicity (which results when S-S bonds are replaced with the weaker S-Se).
If you lived in a high-Se area you wouldn’t want to eat brazil nuts, but everywhere else, you could do it safely.
The super brazil nuts with 200mcg each are NOT the ones in the shops; these have an average 19mcg each.
Hi George,
I’m pretty sure that 750 mcg selenium a day is not safe long-term. I’ll try to revisit the selenium literature in coming months.
Paul, do you think that the prevalence of Retinyl Palmitate being used in skin care products could be negatively contributing to the “Vitamin A + DHA + Oxidative Stress” problem?
Thanks,
Barry.
Hi Barry,
I doubt it but I don’t know.
Folate and methylation;
folate is methylated from serine-glycine conversion. As far as I know it can’t be methylated from methyldonors. It goes serine + folate = MTHF + glycine, MTHF + B12 = methylcobalamin + folate (I am cutting some corners here), with methylcobalamin as the methyl donor co-enzyme that recycles methionine (betaine can also do this), which then becomes SAMe, which produces choline.
the other pathway is THfolate into nucleotides, rate limiting for DNA and RNA synthesis. So uncoverted folate could be a cancer promoter under some circumstances.
Brazil nuts 19mcg Se http://www.ajcn.org/content/87/2/379.abstract
Vitamin A (as its metabolite all-trans retinoic acid) is needed for Treg – Th17 differentiation (immune tolerance), for example, the anti-allergic effects of probiotics.
ATRA is a powerful antinflammatory in the right milieu, and Vit A may be an important adjunct when taming inflammation.
Pyridoxine is the only vitamin that’s harmed me. Neuropathy and optic nueritis that’s taken years to fix. Easy to mistake for MS. Still don’t understand what pathways are involved. Very localised effect peculiar to neurons, I suspect. Sensitivity to B6 is one after-effect, which makes it hard to find a good multi. Luckily, eating enough meat supplies all the Bs.
I blame taking B6 when not eating, and being deficient in Mg and B2. Otherwise eveyone would get SFx.
You may already know this by now: B-6 pyridoxal-5-phosphate, for me, eliminated the numbness I had taking “standard” B-6.
Whether retinol is toxic seems to depend on a CYP conversion that is induced by alcohol.
Chronic alcohol consumption interferes with vitamin A
metabolism and may lead to a striking vitamin A
depletion due to a competitive antagonism for the
same hepatic enzymes alcohol dehydrogenase (ADH)
and cytochrome P4502E1 (CYP2E1). Vitamin A supplementation
may correct this deficiency, but chronic
alcohol consumption enhances the intrinsic hepatotoxicity
of vitamin A. We have recently demonstrated in rat
that ROH and RA are biotransformed by induced
CYP2E1 into the PRMs 18-OH-RA and 4-oxo-RA, while
the selective inhibition of CYP2E1 by chlormethiazole
prevents PRM production.
http://www.fasebj.org/content/19/7/845.full.pdf
What else induces CYP21E?
http://www.prodinra.inra.fr/prodinra/pinra/data/2010/09/PUB980000923406741_20100920021024914.pdf
CYP2E1 is also capable of metabolizing endogenous chemicals including acetone and acetol, which are key metabolites in the methylglyoxal and propanediol pathways of gluconeogenesis (8, 9). CYP2E1 can also carry out the metabolism of arachidonic
acid, resulting in the production of several hydroxyeicosatetraenoic acids (10), some of which may have physiological and pharmacological properties (11).
CYP2E1 is inducible by ethanol and other low molecular weight substrates (5, 12). This induction is primarily due to a postranscriptional mechanism where presence of the substrate stabilizes the enzyme from degradation (13). However, transcriptional mechanisms have not been ruled out (14). This enzyme is also induced by starvation and in uncontrolled diabetes (15, 16).
Very interesting………………..
Hmmmm … Well, if CYP21E is induced by ketosis as well as ethanol, then does a ketogenic diet increase vitamin A hepatotoxicity?
Well, you’d have to assume the Inuit diet is very high in retinol. And a low-carb diet is usually a good source. Saturated fat may beneficially influence CYP21E downstream effects:
http://jn.nutrition.org/content/134/4/904.full
Thus, saturated fat protected rats from alcoholic liver disease in a dose-responsive fashion. Changes in dietary fat composition did not alter ethanol metabolism or CYP2E1 induction, but hepatic CYP4A levels increased markedly in rats fed the saturated fat diet. Dietary saturated fat also decreased liver triglyceride, PUFA, and total FFA concentrations (P < 0.05). Increases in dietary saturated fat increased liver membrane resistance to oxidative stress. In addition, reduced alcoholic steatosis was associated with reduced fatty acid synthesis in combination with increased CYP4A-catalyzed fatty acid oxidation and effects on lipid export.
Very interesting discussion!
I have been taking a closer look at vitamin A (real not beta carotene 😉 for some time now and am still not 100% sure we (let alone I) understand its exact metabolic function.
Wrt to the increase in vitamin A consumption from retinol (or retinyl palmitate), a 1970 study by Stock et al. (http://www.ajcn.org/content/23/7/948.long) suggests that the latter is not greater on a low carb diet (67g of carbs vs. 216g of carbs) – so I am not sure that it is a “given fact” that low carbers necessarily get more retinol in their diets than “normal carbers”. Moreover, in view of the debatable negative effects on thyroid function the conversion of beta carotene could be hampered.
Vitamin A and obesity?
I have come across this study
only recently, which provides rodent and epidemiological evidence for the anti-obesity effects of vitamin A (probably mediated via its anti-inflammatory effects), about which I have read in in-vitro studies before.
What’s the role of the retinol binding proteins?
I am yet still not sure about the role the various binding proteins have in this context. Obviously there are elevations of RBP in obese individuals, the question is though, whether those are just corollary or of any causative nature (binding A would diminish its effects at the cellular level I would think)
With the current hype on vitamin D interesting studies like
have totally been overlooked and my personal believe is that we will soon be sorry for the huge emphasis we have been putting on vitamin D as of late.
I’ve been reading a few blogs recently that have been talking about the importance of the Vitamin A/D balance.
Here’s some text from one that interested me (as my night vision is not great);
“Vitamin A deficiency affects vision by inhibiting the production of rhodopsin, the eye pigment responsible for sensing low light situations. Rhodopsin is found in the retina and is composed of retinal, which is an active form of vitamin A, and opsin a protein made by the retina.
Basically, if you “over do” the use of Vitamin D3, you will not make enough rhodopsin (from a relative Vitamin A deficiency) and you will suffer from night blindness.”
Source:
http://jackkruse.com/what-can-you-find-about-your-own-health/
From under the heading “How do you tell if you are taking too much Vitamin D to get to optimal?”
although I have really done my homework on that one, I could find only a single study from the mid 20th century with at least some information, where *tadaa* people still used vitamin A to counter vitamin D toxicity. If I recall correctly the ratio where A countered D was somewhat about 10 to 1 or so…
that being said I am not sold on the idea that we are supposed to get the lions-share of Vitamin D from dietary sources, let alone supplements, anyway. And I suspect that its local effects on calcium absorption from the gut (when taken orally), as well as its inhibitory effect on vitamin A are soon going to come back on us.
Good stuff.
The immunological effect of ATRA relates to it being essential for Treg (immune tolerance-promoting cells) differentiation. If it’s deficient, Th17 (hyperinflammatory T helper cells) stay in circulation. If you were using probiotics in post-infection, ATRA would help produce the desired response. And some infections, e.g. measles, really chew through vit A stores.
Ketones and Vit A; it seems to be acetone that induces CYP21E. Acetone is a “use it or lose it” spillover of excess ketone body producton and I don’t think levels get very high in normal dietary ketosis.
I remember from the 70s, stories of IRA prisoners like Bobby Sands starving to death on hunger strikes.
The medical experts always said the biggest danger of permanent harm in a hunger strike was from vitamin A deficiency, which presented first and did lasting damage to the eyes. Now we know why.
Zinc is protective against vit A toxicity
Zinc deficiency is thought to interfere with vitamin A metabolism in several ways: (1) zinc deficiency results in decreased synthesis of retinol binding protein (RBP), which transports retinol through the circulation to tissues (e.g., the retina) and also protects the organism against potential toxicity of retinol; (2) zinc deficiency results in decreased activity of the enzyme that releases retinol from its storage form, retinyl palmitate, in the liver; and (3) zinc is required for the enzyme that converts retinol into retinal (8, 9).
http://lpi.oregonstate.edu/infocenter/vitamins/vitaminA/
Reliable and thorough, if somewhat conservative, summary as always at the Linus Pauling Institute website.
Saw this in a Men’s Health. http://i.imgur.com/ba3Af.png Men with 1000mcg folic acid supplement were 2.6x likely for prostate cancer in 10yrs vs placebo.
I think I have it, Paul.
It’s not (just) the niacin but the thiamine and other TCA cycle co-enzymes, in a high-carb context.
Thiamine deficiency suppresses lipogenesis as thiamine is needed to convert pyruvate to Acetyl-CoA.
What does marginal thiamine status do on a high-carb diet? One eats less and stores less fat.
I posted this on hyperlipid a minute ago:
“Consider the triage theory of micronutrient disposal, and the fact that deficiency of TCA co-enzymes like thiamine suppresses both lipogenesis and appetite.
Consider low obesity in the past on unfortified white bread and sugar, and low obesity in white rice cultures.
Hypothesis:
On a high-carb diet that is optimal for TCA co-enzyme vitamins, lipogenesis is favoured and appetite increased so that fat can be stored.
On a high-carb diet that is marginal for TCA co-enzymes, direct conversion of glucose to ATP is favoured, appetite is decreased, and lipogenesis is suppressed.
For example, alcohol depletes thiamine and absence of normal body fat often results from alcoholism.
Yet beer drinkers can gain weight; beer is a source of thiamine and other TCA co-enzymes.
Pathological reactions to toxins (such as alcoholic fatty liver) may be somewhat less influenced by triage than processes which are part of the evolutionary round.
Paul Jaminet considered the epidemiological evidence against flour supplementation a while ago.
I’ll go back and have a look at that.
The effect ought to differ on a case by case basis; genetics and other factors influence micronutrient uptake and usage.”
Looking at you evidence for niacin, niacin supplementation matches thiamine and riboflavin.
Deficiency of these vitamins causes anorexia; does marginal status lower appetite and fat storage?
Is this why asian rice eaters are thinner?
Interesting hypothesis, George. I’ll have to think about that one.
If you’re right then thiamin status should be positively correlated with obesity but negatively correlated with diabetes, since lipogenesis protects against diabetes.
The Zhou et al paper did find the correlation of thiamin status with obesity was almost as strong as that for niacin: http://www.ncbi.nlm.nih.gov/pubmed/21126339. However, that was with a long lag — 10+ years.
But a paper claims thiamin prevents obesity in certain strains of rats: http://www.ncbi.nlm.nih.gov/pubmed/21422702.
Thiamin deficiency is associated with diabetes: http://www.ncbi.nlm.nih.gov/pubmed/22719800
Obese individuals as thiamine storers:
http://www.ncbi.nlm.nih.gov/pubmed/15098017
thiamine probably protects against fat-induced obesity in rats, as rat researchers are blind to fattening carbohydrates.
If thiamine is a factor in obesity it is also protective. Thiamine facilitates normal fat storage, not pathology.
I would expect the big difference to be between marginal thiamine (meat with polished rice, cheese with unfortified bread and sugar) and 2x RDA thiamine.
I’m not expecting an extra effect of thiamine excess; but with super-storers, who knows?
Posted it here; we’ll see what discussion results.
http://hopefulgeranium.blogspot.co.nz/2012/08/the-role-of-vitamin-fortification-in.html
Interesting question about the fermented cod liver oil. Guided by my longterm membership in WAPF, I’ve been taking cod liver oil since 2000. I tried the fermented CLO for a couple of years, but didn’t like it. The taste was not a problem for me, it’s more that I just didn’t feel right while taking it (even combined with the butter oil). I have now switched to Sonne’s, which has a good A/D ratio, but is not fermented, and I feel fine with it. Not scientific, just my experience!
Hi Paul,
Re: Neu5Gc – Is eating grass-fed beef liver a significant source of Neu5Gc? I have been eating a quarter pound per week, as your book recommends.
Would chicken liver be better in this regard?
Jim
Hi Jim,
All cells are coated in Neu5gc, so liver will have similar amounts to other meats. Joints will probably have the most.
Chicken liver is a good non-Neu5gc replacement but you should probably supplement copper if you switch.
Sign the White House Petition to end Mandatory Flour Fortification with Folic Acid linked to Cancer
http://1.usa.gov/1wlovWv
Paul, please help spread the word. Tweet it. Share it on Facebook.
Thanks!
Please post the link to the next article in this series – the one you referenced: “There are several potential health problems that could arise from excessive intake of folic acid, and I’ll explore a few in this series.” Can’t find it under a search for folic acid. Thanks.
He’s also said “Natural forms of folate can also be problematic in excess.” So it would be interesting to see that article.